Hospitalizations among children with sickle cell disease enrolled in the Kumasi Sickle Cell Pan African Consortium (SPARCo) database: A cross sectional study
- PMID: 37670846
- PMCID: PMC10475768
- DOI: 10.1002/hsr2.1534
Hospitalizations among children with sickle cell disease enrolled in the Kumasi Sickle Cell Pan African Consortium (SPARCo) database: A cross sectional study
Abstract
Background and aims: Sickle cell disease (SCD) is the commonest monogenic haemolytic disorder in Africa. Despite strides made in its management, a significant proportion of patients are hospitalized from the various complications of the disease. This study set out to describe the main causes and outcomes of hospitalizations among pediatric patients with SCD.
Methods: A cross-sectional study was conducted at the Pediatric Emergency Unit of Komfo Anokye Teaching Hospital within a period of 12 months to recruit pediatric SCD patients. This study looked at causes of admission, length of hospital stay (LOS), and outcome of admission.
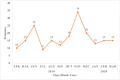
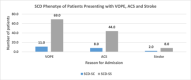
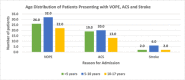
Results: Of the 201 SCD patients recruited, 57.2% were males and majority were of SCD-SS phenotype 83.1%. The median age was 6 years. The three leading causes of hospitalization were Vaso-occlusive pain events (VOPE) (39.8%), acute chest syndrome (ACS) (25.9%), and infections (12.4%). Ten (5.0%) of the patients presented with a stroke. High admissions were observed in June (12.4%) and November (16.9%). The median (interquartile range [IQR]) LOS was 6 days (IQR: 4-10). Six (3.0%) of the patients died from complications of the disease during hospitalization.
Conclusion: VOPE, ACS, infections, and acute anaemia from hyperhaemolysis were observed as the most common causes of admissions among SCD patients. A good outcome of discharge was seen in most of the patients that were hospitalized with a median length of stay of 6 days. This study also strengthens the importance of a good SCD database with patient follow-ups for better outcomes in SCD patients.
Keywords: Vaso‐occlusive pain episodes; acute chest syndrome; hospitalization; infections; length of hospital stay; sickle cell disease.
© 2023 The Authors. Health Science Reports published by Wiley Periodicals LLC.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
Similar articles
-
Establishing a Sickle Cell Disease Registry in Africa: Experience From the Sickle Pan-African Research Consortium, Kumasi-Ghana.Front Genet. 2022 Feb 24;13:802355. doi: 10.3389/fgene.2022.802355. eCollection 2022. Front Genet. 2022. PMID: 35281803 Free PMC article.
-
An analysis of inpatient pediatric sickle cell disease: Incidence, costs, and outcomes.Pediatr Blood Cancer. 2018 Jan;65(1). doi: 10.1002/pbc.26758. Epub 2017 Aug 12. Pediatr Blood Cancer. 2018. PMID: 28801954
-
Hospitalization Events Among Adolescents and Adults With Sickle Cell Disease in a Tertiary Care Center in Central India.Cureus. 2024 May 27;16(5):e61185. doi: 10.7759/cureus.61185. eCollection 2024 May. Cureus. 2024. PMID: 38933640 Free PMC article.
-
Pharmacological interventions for painful sickle cell vaso-occlusive crises in adults.Cochrane Database Syst Rev. 2019 Nov 14;2019(11):CD012187. doi: 10.1002/14651858.CD012187.pub2. Cochrane Database Syst Rev. 2019. PMID: 31742673 Free PMC article.
-
Contemporary Management and Prevention of Vaso-Occlusive Crises (VOCs) in Adults With Sickle Cell Disease.J Pharm Pract. 2023 Feb;36(1):139-148. doi: 10.1177/08971900211026644. Epub 2021 Jun 21. J Pharm Pract. 2023. PMID: 34151636 Review.
Cited by
-
Transition Readiness of Pediatric Sickle Cell Patients to Adult Clinic in a Teaching Hospital, Ghana.Adv Hematol. 2025 Jul 10;2025:2843974. doi: 10.1155/ah/2843974. eCollection 2025. Adv Hematol. 2025. PMID: 40688097 Free PMC article.
-
Beyond Childhood: Adult and Adolescent Sickle Cell Disease and Outcomes in Northern Ghana.EJHaem. 2025 Mar 21;6(2):e70023. doi: 10.1002/jha2.70023. eCollection 2025 Apr. EJHaem. 2025. PMID: 40123794 Free PMC article.
References
-
- Modell B, Darlison M. Global epidemiology of haemoglobin disorders and derived service indicators. Bull World Health Organ. 2008;86(6):480‐487. Available from: http://www.scielosp.org/scielo.php?script=sci_arttext&pid=S0042-96862008... - PMC - PubMed
-
- Dennis‐Antwi JA, Opoku SA, Osei‐Amoh B, Survey of educational needs of health workers and consumers in Ghana prior to the institution of newborn screening for sickle cell disease in Kumasi. Heal Cour. 1995;5(4):28‐32.
-
- Ohene‐Frempong K, Oduro J, Tetteh H, Nkrumah F. Screening newborns for sickle cell disease in Ghana. Pediatrics. 2008;121(2):S120‐S121.
-
- Quinn CT, Rogers ZR, McCavit TL, Buchanan GR. Improved survival of children and adolescents with sickle cell disease. Blood. 2010;115(17):3447‐3452. Available from: https://ashpublications.org/blood/article/115/17/3447/27102/Improved-sur... - PMC - PubMed
-
- Telfer P, Coen P, Chakravorty S, et al. Clinical outcomes in children with sickle cell disease living in England: a neonatal cohort in East London. Haematologica. 2007;92(7):905‐912. Available from: https://pubmed.ncbi.nlm.nih.gov/17606440/ - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources

