Non-invasive myocardial work in aortic stenosis: validation and improvement in left ventricular pressure estimation
- PMID: 37672652
- PMCID: PMC10824486
- DOI: 10.1093/ehjci/jead227
Non-invasive myocardial work in aortic stenosis: validation and improvement in left ventricular pressure estimation
Abstract
Aims: The non-invasive myocardial work index (MWI) has been validated in patients without aortic stenosis (AS). A thorough assessment of methodological limitations is warranted before this index can be applied to patients with AS.
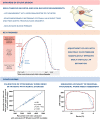
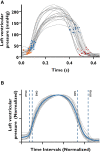
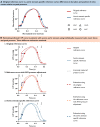
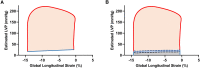
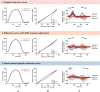
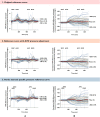
Methods and results: We simultaneously measured left ventricular pressure (LVP) by using a micromanometer-tipped catheter and obtained echocardiograms in 20 patients with severe AS. We estimated LVP curves and calculated pressure-strain loops using three different models: (i) the model validated in patients without AS; (ii) the same model, but with pressure at the aortic valve opening (AVO) adjusted to diastolic cuff pressure; and (iii) a new model based on the invasive measurements from patients with AS. Valvular events were determined by echocardiography. Peak LVP was estimated as the sum of the mean aortic transvalvular gradient and systolic cuff pressure. In same-beat comparisons between invasive and estimated LVP curves, Model 1 significantly overestimated early systolic pressure by 61 ± 5 mmHg at AVO compared with Models 2 and 3. However, the average correlation coefficients between estimated and invasive LVP traces were excellent for all models, and the overestimation had limited influence on MWI, with excellent correlation (r = 0.98, P < 0.001) and good agreement between the MWI calculated with estimated (all models) and invasive LVP.
Conclusion: This study confirms the validity of the non-invasive MWI in patients with AS. The accuracy of estimated LVP curves improved when matching AVO to the diastolic pressure in the original model, mirroring that of the AS-specific model. This may sequentially enhance the accuracy of regional MWI assessment.
Keywords: aortic stenosis; myocardial function; myocardial work index; valvular heart disease.
© The Author(s) 2023. Published by Oxford University Press on behalf of the European Society of Cardiology.
Conflict of interest statement
Conflict of interest: K.R. is co-inventor of the ‘Method for myocardial work analysis’, currently licenced by General Electrics. O.A.S. is also a co-inventor of the method for myocardial work analysis and has filed a patent on ‘Estimation of blood pressure in the heart’. He has received lecture fees from GE Healthcare. The remaining authors have nothing to disclose.
Figures


References
-
- Vahanian A, Beyersdorf F, Praz F, Milojevic M, Baldus S, Bauersachs Jet al. 2021 ESC/EACTS guidelines for the management of valvular heart disease. Eur Heart J 2022;43:561–632. - PubMed
-
- Donal E, Bergerot C, Thibault H, Ernande L, Loufoua J, Augeul Let al. Influence of afterload on left ventricular radial and longitudinal systolic functions: a two-dimensional strain imaging study. Eur J Echocardiogr 2009;10:914–21. - PubMed
-
- Chan J, Edwards NFA, Khandheria BK, Shiino K, Sabapathy S, Anderson Bet al. A new approach to assess myocardial work by non-invasive left ventricular pressure-strain relations in hypertension and dilated cardiomyopathy. Eur Heart J Cardiovasc Imaging 2019;20:31–9. - PubMed
-
- Boe E, Skulstad H, Smiseth OA. Myocardial work by echocardiography: a novel method ready for clinical testing. Eur Heart J Cardiovasc Imaging 2019;20:18–20. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials

