Sex and gender differences in intensive care medicine
- PMID: 37676504
- PMCID: PMC10556182
- DOI: 10.1007/s00134-023-07194-6
Sex and gender differences in intensive care medicine
Abstract
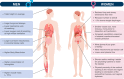
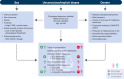
Despite significant advancements in critical care medicine, limited attention has been given to sex and gender disparities in management and outcomes of patients admitted to the intensive care unit (ICU). While "sex" pertains to biological and physiological characteristics, such as reproductive organs, chromosomes and sex hormones, "gender" refers more to sociocultural roles and human behavior. Unfortunately, data on gender-related topics in the ICU are lacking. Consequently, data on sex and gender-related differences in admission to the ICU, clinical course, length of stay, mortality, and post-ICU burdens, are often inconsistent. Moreover, when examining specific diagnoses in the ICU, variations can be observed in epidemiology, pathophysiology, presentation, severity, and treatment response due to the distinct impact of sex hormones on the immune and cardiovascular systems. In this narrative review, we highlight the influence of sex and gender on the clinical course, management, and outcomes of the most encountered intensive care conditions, in addition to the potential co-existence of unconscious biases which may also impact critical illness. Diagnoses with a known sex predilection will be discussed within the context of underlying sex differences in physiology, anatomy, and pharmacology with the goal of identifying areas where clinical improvement is needed. To optimize patient care and outcomes, it is crucial to comprehend and address sex and gender differences in the ICU setting and personalize management accordingly to ensure equitable, patient-centered care. Future research should focus on elucidating the underlying mechanisms driving sex and gender disparities, as well as exploring targeted interventions to mitigate these disparities and improve outcomes for all critically ill patients.
Keywords: AKI; ARDS; Cardiogenic shock; Critical illness; Post-intensive care syndrome; Septic shock; Sex and gender differences; Sex disparities.
© 2023. The Author(s).
Conflict of interest statement
HM: no relevant disclosures. MH: no relevant disclosures. MO: no relevant disclosures. MTL: no relevant disclosures. SNM: no relevant disclosures. SDR: received honorary for lectures from Estor, Fresenius Medical, and Toray. VM: no relevant conflicts of interest. KK: no relevant disclosures. CR: received honorary for lectures from Masimo and Edwards. ADJ: received honoraria for lectures from Medtronic, Viatris, Drager and Fisher & Paykel. JH: received honoraria for lectures from Diagnostica Stago, Pfizer PFE France, Sanofi Aventis France, Inotrem, MSD and Shionogi. CEG: no relevant disclosures.
Figures



References
-
- Arslani K, Tontsch J, Todorov A, Gysi B, Kaufmann M, Kaufmann F, Hollinger A, Wildi K, Merdji H, Helms J, Siegemund M, Gebhard C, Gebhard CE, Swiss Society of Intensive Care M Temporal trends in mortality and provision of intensive care in younger women and men with acute myocardial infarction or stroke. Crit Care. 2023;27:14. doi: 10.1186/s13054-022-04299-0. - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

