Efficacy of stellate ganglion interventions for complex regional pain syndrome in the upper limb-A systematic review and meta-analysis
- PMID: 37693027
- PMCID: PMC10488587
- DOI: 10.4103/ija.ija_204_23
Efficacy of stellate ganglion interventions for complex regional pain syndrome in the upper limb-A systematic review and meta-analysis
Abstract
Background and aims: Stellate ganglion (SG) interventions for treating upper limb complex regional pain syndrome (CRPS) have been reported in studies. However, more substantial evidence is required to reach a consensus on its analgesic efficacy. To the best of our knowledge, no systematic review demonstrating the effectiveness of SG intervention for upper limb CRPS has been reported. Hence, this meta-analysis was done to ascertain the efficacy of SG intervention in managing patients with upper limb CRPS.
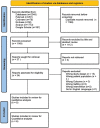
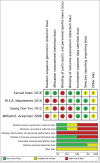
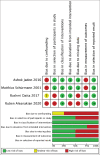
Methods: A database search of PubMed, Cochrane, Embase, Scopus and Google Scholar was done for articles published between January 2001 and December 2021. Two independent reviewers extracted data from the included studies, and the studies were evaluated for any potential risk of bias, and a meta-analysis was performed.
Results: Eight studies were included in the qualitative synthesis, four were randomised controlled trials (RCTs), and the rest were non-RCTs. Six studies were assessed quantitatively. A significant reduction in pain scores post-intervention, up to two weeks, and four to 28 weeks after the procedure was observed, although the included studies exhibited marked heterogeneity. Qualitative analysis of these studies revealed an overall improvement in disability scores and functionality as assessed by an improved range of motion. Most studies reported no complications or only short-term minor complications after the procedure.
Conclusion: Stellate ganglion interventions improve pain and disability scores with self-limiting short-term complications and no long-term complications. However, further studies with a large sample size are required to validate this treatment modality.
Keywords: Chronic pain; complex regional pain syndrome; neuropathic pain; stellate ganglion; upper extremity.
Copyright: © 2023 Indian Journal of Anaesthesia.
Conflict of interest statement
There are no conflicts of interest.
Figures



References
-
- Harden RN, Bruehl S, Stanton-Hicks M, Wilson PR. Proposed new diagnostic criteria for complex regional pain syndrome. Pain Med. 2007;8:326–31. - PubMed
-
- Borchers AT, Gershwin ME. Complex regional pain syndrome: A comprehensive and critical review. Autoimmun Rev. 2014;13:242–65. - PubMed
-
- Money S. Pathophysiology of complex regional pain syndrome and treatment: Recent advancements. Curr Emerg Hosp Med Rep. 2019;7:203–7.
Publication types
LinkOut - more resources
Full Text Sources
