The role of cytoreductive surgery in multifocal/multicentric glioblastomas
- PMID: 37697210
- PMCID: PMC10522503
- DOI: 10.1007/s11060-023-04410-7
The role of cytoreductive surgery in multifocal/multicentric glioblastomas
Abstract
Purpose: Multifocal/multicentric glioblastomas (mGBM) account for up to 20% of all newly diagnosed glioblastomas. The present study investigates the impact of cytoreductive surgery on survival and functional outcomes in patients with mGBM.
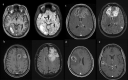
Methods: We retrospectively reviewed clinical and imaging data of 71 patients with newly diagnosed primary (IDH1 wildtype) mGBM who underwent operative treatment in 2015-2020 at the authors' institution. Multicentric/multifocal growth was defined by the presence of ≥ 2 contrast enhancing lesions ≥ 1 cm apart from each other.
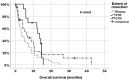
Results: 36 (50.7%) patients had a resection and 35 (49.3%) a biopsy procedure. MGMT status, age, preoperative KPI and NANO scores as well as the postoperative KPI and NANO scores did not differ significantly between resected and biopsied cases. Median overall survival was 6.4 months and varied significantly with the extent of resection (complete resection of contrast enhancing tumor: 13.6, STR: 6.4, biopsy: 3.4 months; P = 0.043). 21 (58.3%) of resected vs. only 12 (34.3%) of biopsied cases had radiochemotherapy (p = 0.022). Multivariate analysis revealed chemo- and radiotherapy and also (albeit with smaller hazard ratios) extent of resection (resection vs. biopsy) and multicentric growth as independent predictors of patient survival. Involvement of eleoquent brain regions, as well as neurodeficit rates and functional outcomes did not vary significantly between the biopsy and the resection cohorts.
Conclusion: Resective surgery in mGBM is associated with better survival. This benefit seems to relate prominently to an increased number of patients being able to tolerate effective adjuvant therapies after tumor resections. In addition, cytoreductive surgery may have a survival impact per se.
Keywords: Biopsy; Glioblastoma; Growth patterns; Multicentric; Multifocal; Resection.
© 2023. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures
Similar articles
-
Resection versus biopsy in the treatment of multifocal glioblastoma: a weighted survival analysis.J Neurooncol. 2020 May;148(1):155-164. doi: 10.1007/s11060-020-03508-6. Epub 2020 May 11. J Neurooncol. 2020. PMID: 32394325
-
Multiple craniotomies in the management of multifocal and multicentric glioblastoma. Clinical article.J Neurosurg. 2011 Mar;114(3):576-84. doi: 10.3171/2010.6.JNS091326. Epub 2010 Aug 6. J Neurosurg. 2011. PMID: 20690813
-
Is There a Role for Surgical Resection of Multifocal Glioblastoma? A Retrospective Analysis of 100 Patients.Neurosurgery. 2021 Nov 18;89(6):1042-1051. doi: 10.1093/neuros/nyab345. Neurosurgery. 2021. PMID: 34662898
-
Newly Diagnosed Multifocal GBM: A Monocentric Experience and Literature Review.Curr Oncol. 2022 May 11;29(5):3472-3488. doi: 10.3390/curroncol29050280. Curr Oncol. 2022. PMID: 35621670 Free PMC article. Review.
-
Congress of neurological surgeons systematic review and evidence-based guidelines update on the role of emerging developments in the management of newly diagnosed glioblastoma.J Neurooncol. 2020 Nov;150(2):269-359. doi: 10.1007/s11060-020-03607-4. Epub 2020 Nov 19. J Neurooncol. 2020. PMID: 33215345
Cited by
-
Patterns of care and survival in patients with multifocal glioblastoma: A Danish cohort study.Neurooncol Pract. 2024 Mar 9;11(4):421-431. doi: 10.1093/nop/npae020. eCollection 2024 Aug. Neurooncol Pract. 2024. PMID: 39006522 Free PMC article.
-
Maximal Intraoperative 5-Aminolevulinic Acid Fluorescence During Surgical Resection of Multiple Lesions in Multifocal Glioblastoma to Achieve Greater Extent of Resection: A Case Report.Cureus. 2025 Feb 16;17(2):e79083. doi: 10.7759/cureus.79083. eCollection 2025 Feb. Cureus. 2025. PMID: 40104462 Free PMC article.
-
Environmental Hazards and Glial Brain Tumors: Association or Causation?Int J Mol Sci. 2025 Aug 1;26(15):7425. doi: 10.3390/ijms26157425. Int J Mol Sci. 2025. PMID: 40806554 Free PMC article. Review.
-
Identifying targetable alterations predictive of distant progression in glioblastoma patients undergoing standard therapy.Neurooncol Adv. 2025 May 7;7(1):vdaf092. doi: 10.1093/noajnl/vdaf092. eCollection 2025 Jan-Dec. Neurooncol Adv. 2025. PMID: 40575417 Free PMC article.
References
-
- Wen PY, Weller M, Lee EQ, Alexander BM, Barnholtz-Sloan JS, Barthel FP, Batchelor TT, Bindra RS, Chang SM, Chiocca EA, Cloughesy TF, DeGroot JF, Galanis E, Gilbert MR, Hegi ME, Horbinski C, Huang RY, Lassman AB, Le Rhun E, Lim M, Mehta MP, Mellinghoff IK, Minniti G, Nathanson D, Platten M, Preusser M, Roth P, Sanson M, Schiff D, Short SC, Taphoorn MJB, Tonn JC, Tsang J, Verhaak RGW, von Deimling A, Wick W, Zadeh G, Reardon DA, Aldape KD, van den Bent MJ. Glioblastoma in adults: a society for neuro-oncology (SNO) and european society of neuro-oncology (EANO) consensus review on current management and future directions. Neuro Oncol. 2020;22(8):1073–1113. doi: 10.1093/neuonc/noaa106. - DOI - PMC - PubMed
-
- Friso F, Rucci P, Rosetti V, Carretta A, Bortolotti C, Ramponi V, Martinoni M, Palandri G, Zoli M, Badaloni F, Franceschi E, Asioli S, Fabbri VP, Rustici A, Foschini MP, Brandes AA, Mazzatenta D, Sturiale C, Conti A. Is there a role for surgical resection of multifocal glioblastoma? a retrospective analysis of 100 patients. Neurosurgery. 2021;89(6):1042–1051. doi: 10.1093/neuros/nyab345. - DOI - PubMed
-
- Baro V, Cerretti G, Todoverto M, Della Puppa A, Chioffi F, Volpin F, Causin F, Busato F, Fiduccia P, Landi A, d’Avella D, Zagonel V, Denaro L, Lombardi G. Newly diagnosed multifocal GBM: a monocentric experience and literature review. Curr Oncol. 2022;29(5):3472–3488. doi: 10.3390/curroncol29050280. - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

