Correlating Quantitative MRI-based Apparent Diffusion Coefficient Metrics with 24-month Neurodevelopmental Outcomes in Neonates from the HEAL Trial
- PMID: 37698478
- PMCID: PMC10546287
- DOI: 10.1148/radiol.223262
Correlating Quantitative MRI-based Apparent Diffusion Coefficient Metrics with 24-month Neurodevelopmental Outcomes in Neonates from the HEAL Trial
Abstract
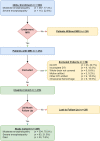
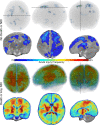
Background Multiple qualitative scoring systems have been created to capture the imaging severity of hypoxic ischemic brain injury. Purpose To evaluate quantitative volumes of acute brain injury at MRI in neonates with hypoxic ischemic brain injury and correlate these findings with 24-month neurodevelopmental outcomes and qualitative brain injury scoring by radiologists. Materials and Methods In this secondary analysis, brain diffusion-weighted MRI data from neonates in the High-dose Erythropoietin for Asphyxia and Encephalopathy trial, which recruited participants between January 2017 and October 2019, were analyzed. Volume of acute brain injury, defined as brain with apparent diffusion coefficient (ADC) less than 800 × 10-6 mm2/sec, was automatically computed across the whole brain and within the thalami and white matter. Outcomes of death and neurodevelopmental impairment (NDI) were recorded at 24-month follow-up. Associations between the presence and volume (in milliliters) of acute brain injury with 24-month outcomes were evaluated using multiple logistic regression. The correlation between quantitative acute brain injury volume and qualitative MRI scores was assessed using the Kendall tau-b test. Results A total of 416 neonates had available MRI data (mean gestational age, 39.1 weeks ± 1.4 [SD]; 235 male) and 113 (27%) showed evidence of acute brain injury at MRI. Of the 387 participants with 24-month follow-up data, 185 (48%) died or had any NDI. Volume of acute injury greater than 1 mL (odds ratio [OR], 13.9 [95% CI: 5.93, 32.45]; P < .001) and presence of any acute injury in the brain (OR, 4.5 [95% CI: 2.6, 7.8]; P < .001) were associated with increased odds of death or any NDI. Quantitative whole-brain acute injury volume was strongly associated with radiologists' qualitative scoring of diffusion-weighted images (Kendall tau-b = 0.56; P < .001). Conclusion Automated quantitative volume of brain injury is associated with death, moderate to severe NDI, and cerebral palsy in neonates with hypoxic ischemic encephalopathy and correlated well with qualitative MRI scoring of acute brain injury. Clinical trial registration no. NCT02811263 © RSNA, 2023 Supplemental material is available for this article. See also the editorial by Huisman in this issue.
Conflict of interest statement
Figures


Comment in
-
Automated Quantitative Apparent Diffusion Coefficient Analysis of Neonatal Hypoxic Ischemic Brain Injury.Radiology. 2023 Sep;308(3):e232135. doi: 10.1148/radiol.232135. Radiology. 2023. PMID: 37698473 No abstract available.
References
-
- Kurinczuk JJ , White-Koning M , Badawi N . Epidemiology of neonatal encephalopathy and hypoxic-ischaemic encephalopathy . Early Hum Dev 2010. ; 86 ( 6 ): 329 – 338 . - PubMed
-
- Liu L , Oza S , Hogan D , et al . Global, regional, and national causes of child mortality in 2000-13, with projections to inform post-2015 priorities: an updated systematic analysis . Lancet 2015. ; 385 ( 9966 ): 430 – 440 . - PubMed
-
- Tagin MA , Woolcott CG , Vincer MJ , Whyte RK , Stinson DA . Hypothermia for neonatal hypoxic ischemic encephalopathy: an updated systematic review and meta-analysis . Arch Pediatr Adolesc Med 2012. ; 166 ( 6 ): 558 – 566 . - PubMed
-
- Sarnat HB , Sarnat MS . Neonatal encephalopathy following fetal distress. A clinical and electroencephalographic study . Arch Neurol 1976. ; 33 ( 10 ): 696 – 705 . - PubMed
Publication types
MeSH terms
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

