Risk factors for the occurrence of infection in patients with oral squamous cell carcinoma after restorative reconstruction and its impact on recurrence and quality of life: a retrospective cohort study
- PMID: 37701120
- PMCID: PMC10493792
- DOI: 10.21037/tcr-23-1150
Risk factors for the occurrence of infection in patients with oral squamous cell carcinoma after restorative reconstruction and its impact on recurrence and quality of life: a retrospective cohort study
Abstract
Background: Worldwide, there are approximately 300,000 new cases of oral squamous cell carcinoma (OSCC) and 100,000 deaths each year. The complexity of oral and maxillofacial structures leads to a high risk of surgical infection such as radical tumor resection and free flap reconstruction. Previous studies have shown that diabetes mellitus, previous radiotherapy, oral-neck communication, etc. are risk factors for postoperative infection, but the influence of time on prognosis has not been clarified in detail. This study supplements this aspect and provided a reference for improving the quality of life of patients.
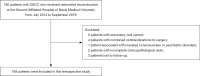
Methods: We retrospectively analyzed a total of 168 patients who developed OSCC from July 2014 to September 2019. According to the inclusion and exclusion criteria of this study, the general data questionnaire designed by ourselves was used to sort out the general characteristics and clinical data of the subjects. The t test, Chi-square test and binary logistic regression were used for statistical analysis. Surgical site infections (SSI) are defined as infections associated with surgical procedures. The quality of life was evaluated by the 36-Item Short Form Survey (SF-36) score. A 3-year follow-up was conducted by telephone, Email and outpatient review.
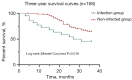
Results: Among the 168 patients, the total number of postoperative infections was 22 (13.1%). Binary logistic regression analysis showed that body mass index (BMI) (OR =0.029, P=0.039), American Society of Anesthesiologists (ASA) classification (OR =21.443, P=0.042), preoperative radiotherapy (OR =19.993, P=0.022), Jaw resection status (OR =29.665, P=0.021), Perioperative transfusion (OR =29.148, P=0.020), preoperative white blood cell count (OR =1.763, P=0.017), albumin level (OR =0.853, P=0.033) were independent influencing factors between the two groups (P<0.05). Except for the social functioning and role-emotional dimensions, all dimensions of SF-36 in patients with infection were significantly lower than those without infection.
Conclusions: The incidence of postoperative infection after restorative and reconstructive surgery for OSCC deserves the attention of clinicians. For high-risk infected persons, relevant anti-infection measures should be taken early against the infectious source, and the possibility of nosocomial infection should be attached great importance in clinical work. After discharge, patients should also actively do follow-up, education and other related work to reduce the incidence of postoperative infection.
Keywords: Oral squamous cell carcinoma (OSCC); postoperative infection; prognosis; repair and reconstruction.
2023 Translational Cancer Research. All rights reserved.
Conflict of interest statement
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://tcr.amegroups.com/article/view/10.21037/tcr-23-1150/coif). The authors have no conflicts of interest to declare.
Figures
Similar articles
-
[Analysis of etiological characteristics and establishment of prediction model of postoperative infections in patients undergoing oral squamous cell carcinoma surgery with free flap reconstruction].Beijing Da Xue Xue Bao Yi Xue Ban. 2022 Feb 18;54(1):68-76. doi: 10.19723/j.issn.1671-167X.2022.01.011. Beijing Da Xue Xue Bao Yi Xue Ban. 2022. PMID: 35165470 Free PMC article. Chinese.
-
[Comparison of postoperative mid-term and long-term quality of life between Billroth-I gastroduodenostomy and Billroth-II gastrojejunostomy after radical distal gastrectomy in patients with gastric cancer: a cohort study based on a case registry database].Zhonghua Wei Chang Wai Ke Za Zhi. 2022 May 25;25(5):401-411. doi: 10.3760/cma.j.cn441530-20220304-00081. Zhonghua Wei Chang Wai Ke Za Zhi. 2022. PMID: 35599395 Chinese.
-
[Study of the risk factors of postoperative surgical site infection in geriatric patients with oral squamous cell carcinoma].Hua Xi Kou Qiang Yi Xue Za Zhi. 2016 Apr;34(2):173-7. doi: 10.7518/hxkq.2016.02.014. Hua Xi Kou Qiang Yi Xue Za Zhi. 2016. PMID: 27337928 Free PMC article. Chinese.
-
Perioperative Risk Factors Associated With Unplanned Reoperation Following Vascularized Free Flaps Reconstruction of the Oral Squamous Cell Carcinoma.J Craniofac Surg. 2022 Nov-Dec 01;33(8):2507-2512. doi: 10.1097/SCS.0000000000008762. Epub 2022 Aug 2. J Craniofac Surg. 2022. PMID: 36409870
-
A model for predicting transfusion requirements in head and neck surgery.Laryngoscope. 1995 Aug;105(8 Pt 2 Suppl 73):1-17. doi: 10.1288/00005537-199508001-00001. Laryngoscope. 1995. PMID: 7630307 Review.
Cited by
-
Preoperative Clinical and Tumor Factors Associated With Adjuvant Therapy for Oral Cavity Cancer.JAMA Otolaryngol Head Neck Surg. 2025 May 1;151(5):466-475. doi: 10.1001/jamaoto.2024.5250. JAMA Otolaryngol Head Neck Surg. 2025. PMID: 40146171
-
Analysis of the current situation and risk factors of nosocomial infections in oral cancer patients after surgery.World J Surg Oncol. 2025 May 22;23(1):197. doi: 10.1186/s12957-025-03836-9. World J Surg Oncol. 2025. PMID: 40405158 Free PMC article.
-
Metabolic biomarker in oral squamous cell carcinoma - a comprehensive review.GMS Interdiscip Plast Reconstr Surg DGPW. 2025 Apr 16;14:Doc01. doi: 10.3205/iprs000190. eCollection 2025. GMS Interdiscip Plast Reconstr Surg DGPW. 2025. PMID: 40535577 Free PMC article. Review.
-
Association of Site and Recurrence in Oral Squamous Cell Carcinoma Patients Visiting Private Hospital in Chennai: A Retrospective Study.Cureus. 2024 Jan 23;16(1):e52774. doi: 10.7759/cureus.52774. eCollection 2024 Jan. Cureus. 2024. PMID: 38389605 Free PMC article.
References
-
- Tumino R, Vicario G. Head and neck cancers: oral cavity, pharynx, and larynx. Epidemiol Prev 2004;28:28-33. - PubMed
LinkOut - more resources
Full Text Sources