Computed tomographic abdominal fat volume estimation - a handy tool to predict the risk of metabolic syndrome
- PMID: 37701173
- PMCID: PMC10493863
- DOI: 10.5114/pjr.2023.131010
Computed tomographic abdominal fat volume estimation - a handy tool to predict the risk of metabolic syndrome
Abstract
Purpose: Abdominal obesity plays a significant role in the development of metabolic syndrome, with individual metabolic risk profiles for visceral and subcutaneous adipose tissues. This study aimed to calculate and correlate the subcutaneous, visceral, and total fat compartment volume in metabolic and non-metabolic syndrome patients.
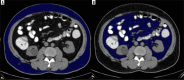
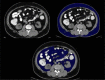
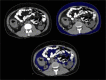
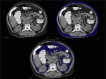
Material and methods: This was a cross-sectional study conducted on 112 patients categorized into Group A (with metabolic syndrome) and Group B (without metabolic syndrome). They were subjected to computed tomography (CT) study of the abdomen using a 128-slice MDCT scanner. Body mass index (BMI), visceral fat volume (VFV), subcutaneous fat volume (SFV), and total fat volume (TFV) were calculated and correlated with biochemical evidence of metabolic syndrome.
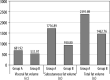
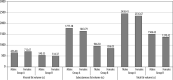
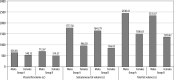
Results: The mean age of patients in Group A was 60.91 ± 12.23 years as compared to Group B, which was 50.12 ± 16.30 years. Overall, a male predominance was observed, i.e. 69 cases (61.6%). BMI was proven to be an inaccurate risk predictor. However, mean VFV, SFV, and TFV was statistically higher in patients with metabolic syndrome (p = 0.001), with visceral fat volume predicting a higher risk in females (p = 0.026).
Conclusions: Abdominal CT is a commonly performed yet unexplored tool for the risk assessment of metabolic syndrome. Through the results obtained in this study, we have proven the need for calculating SFV, VFV, and TFV as predictors of metabolic syndrome in comparison to the conventional practice of BMI assessment. The radiologist can thus work with the clinician to effectively detect and treat this health condition.
Keywords: abdominal subcutaneous fat; abdominal visceral fat; body mass index; computed tomography; metabolic syndrome.
© Pol J Radiol 2023.
Conflict of interest statement
The authors report no conflict of interest.
Figures
Similar articles
-
Cutoff values of body fat composition to predict metabolic risk factors with normal waist circumference in Asian Indian population.Eur Radiol. 2023 Jan;33(1):711-719. doi: 10.1007/s00330-022-09009-6. Epub 2022 Jul 19. Eur Radiol. 2023. PMID: 35852580
-
Optimal cutoff values for visceral fat volume to predict metabolic syndrome in a Korean population.Medicine (Baltimore). 2021 Sep 10;100(36):e27114. doi: 10.1097/MD.0000000000027114. Medicine (Baltimore). 2021. PMID: 34516502 Free PMC article.
-
Visceral adiposity and inflammatory bowel disease.Int J Colorectal Dis. 2021 Nov;36(11):2305-2319. doi: 10.1007/s00384-021-03968-w. Epub 2021 Jun 9. Int J Colorectal Dis. 2021. PMID: 34104989 Review.
-
Association between volume and glucose metabolism of abdominal adipose tissue in healthy population.Obes Res Clin Pract. 2017 Sep-Oct;11(5 Suppl 1):133-143. doi: 10.1016/j.orcp.2016.12.007. Epub 2017 Jan 7. Obes Res Clin Pract. 2017. PMID: 28073639 Review.
Cited by
-
Potential Therapeutic Exploitation of G Protein-Coupled Receptor 120 (GPR120/FFAR4) Signaling in Obesity-Related Metabolic Disorders.Int J Mol Sci. 2025 Mar 11;26(6):2501. doi: 10.3390/ijms26062501. Int J Mol Sci. 2025. PMID: 40141148 Free PMC article. Review.
References
-
- Alberti KG, Eckel RH, Grundy SM, et al. . Harmonizing the metabolic syndrome: a joint interim statement of the International Diabetes Federation Task Force on Epidemiology and Prevention; National Heart, Lung, and Blood Institute; American Heart Association; World Heart Federation; International Atherosclerosis Society; and International Association for the Study of Obesity. Circulation 2009; 120: 1640-1645. - PubMed
-
- Enkhmaa B, Shiwaku K, Anuurad E, et al. . Prevalence of the metabolic syndrome using the Third Report of the National Cholesterol Educational Program Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (ATP III) and the modified ATP III definitions for Japanese and Mongolians. Clin Chim Acta 2005; 352: 105-113. - PubMed
-
- Sato F, Maeda N, Yamada T, et al. . Association of epicardial, visceral, and subcutaneous fat with cardiometabolic diseases. Circ J 2018; 82: 502-508. - PubMed
-
- Reijrink M, de Boer SA, Spoor DS, et al. . Visceral adipose tissue volume is associated with premature atherosclerosis in early type 2 diabetes mellitus independent of traditional risk factors. Atherosclerosis 2019; 290: 87-93. - PubMed
LinkOut - more resources
Full Text Sources
