EEG pre-burst suppression: characterization and inverse association with preoperative cognitive function in older adults
- PMID: 37711992
- PMCID: PMC10499509
- DOI: 10.3389/fnagi.2023.1229081
EEG pre-burst suppression: characterization and inverse association with preoperative cognitive function in older adults
Abstract
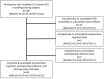
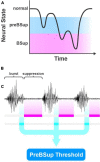
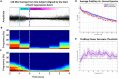
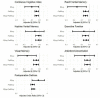
The most common complication in older surgical patients is postoperative delirium (POD). POD is associated with preoperative cognitive impairment and longer durations of intraoperative burst suppression (BSup) - electroencephalography (EEG) with repeated periods of suppression (very low-voltage brain activity). However, BSup has modest sensitivity for predicting POD. We hypothesized that a brain state of lowered EEG power immediately precedes BSup, which we have termed "pre-burst suppression" (preBSup). Further, we hypothesized that even patients without BSup experience these preBSup transient reductions in EEG power, and that preBSup (like BSup) would be associated with preoperative cognitive function and delirium risk. Data included 83 32-channel intraoperative EEG recordings of the first hour of surgery from 2 prospective cohort studies of patients ≥age 60 scheduled for ≥2-h non-cardiac, non-neurologic surgery under general anesthesia (maintained with a potent inhaled anesthetic or a propofol infusion). Among patients with BSup, we defined preBSup as the difference in 3-35 Hz power (dB) during the 1-s preceding BSup relative to the average 3-35 Hz power of their intraoperative EEG recording. We then recorded the percentage of time that each patient spent in preBSup, including those without BSup. Next, we characterized the association between percentage of time in preBSup and (1) percentage of time in BSup, (2) preoperative cognitive function, and (3) POD incidence. The percentage of time in preBSup and BSup were correlated (Spearman's ρ [95% CI]: 0.52 [0.34, 0.66], p < 0.001). The percentage of time in BSup, preBSup, or their combination were each inversely associated with preoperative cognitive function (β [95% CI]: -0.10 [-0.19, -0.01], p = 0.024; -0.04 [-0.06, -0.01], p = 0.009; -0.04 [-0.06, -0.01], p = 0.003, respectively). Consistent with prior literature, BSup was significantly associated with POD (odds ratio [95% CI]: 1.34 [1.01, 1.78], p = 0.043), though this association did not hold for preBSup (odds ratio [95% CI]: 1.04 [0.95, 1.14], p = 0.421). While all patients had ≥1 preBSup instance, only 20.5% of patients had ≥1 BSup instance. These exploratory findings suggest that future studies are warranted to further study the extent to which preBSup, even in the absence of BSup, can identify patients with impaired preoperative cognition and/or POD risk.
Keywords: EEG; anesthesia; burst suppression; non-cardiac surgery; perioperative; postoperative delirium; pre-burst suppression; preoperative cognition.
Copyright © 2023 Reese, Christensen, Anolick, Roberts, Wong, Wright, Acker, Browndyke, Woldorff, Berger and the MADCO-PC and INTUIT Investigators.
Conflict of interest statement
MB has received material support (i.e., EEG monitor loan) for a postoperative recovery study in older adults from Masimo and has participated in Masimo peer to peer educational sessions, for which his honorarium was donated at his request to the Foundation for Anesthesia Education and Research. MB also acknowledges private legal consulting fees related to postoperative neurocognitive function in older adults. The remaining authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
References
-
- Berger M., Ryu D., Reese M., McGuigan S., Evered L., Price C., et al. (2023). A real-time neurophysiologic stress test for the aging brain: Novel perioperative and ICU applications of EEG in older surgical patients. Neurotherapeutics 10.1007/s13311-023-01401-4 [Epub ahead of print]. - DOI - PMC - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

