Corneal Endothelial Cell Cultures from Organotypic Preservation of Older Donor Corneas Are Suitable for Advanced Cell Therapy
- PMID: 37722372
- PMCID: PMC10614447
- DOI: 10.1159/000533701
Corneal Endothelial Cell Cultures from Organotypic Preservation of Older Donor Corneas Are Suitable for Advanced Cell Therapy
Abstract
Introduction: The purpose of this work was to evaluate the in vitro growth capacity and functionality of human corneal endothelial cells (hCEC) expanded from corneas of elderly (>60 years) donors that were preserved using an organotypic culture method (>15 days, 31°C) and did not meet the clinical criteria for keratoplasty.
Methods: Cell cultures were obtained from prior descemetorhexis (≥10 mm) and a controlled incubation with collagenase type I followed by recombinant trypsin. Cells were seeded on coated plates (fibronectin-albumin-collagen I) and cultures were expanded using the dual supplemented medium approach (maintenance medium and growth medium), in the presence of a 10 μ<sc>m</sc> Rho-associated protein kinase inhibitor (Y-27632). Cell passages were obtained at culture confluency (∼2 weeks). A quantitative colorimetric WST-1 cell growth assay was performed at different time points of the culture. Morphometric analysis (area assessment and circularity), immunocytochemistry (ZO-1, Na+/K+-ATPase α, Ki67), and transendothelial electrical resistance (TEER) were performed on confluent monolayers.
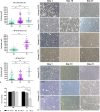
Results: There was no difference between the cell growth profiles of hCEC cultures obtained from corneas older than 60 years, whether preserved cold or cultivated organotypic corneas. Primary cultures were able to maintain a certain cell circularity index (around 0.8) and morphology (hexagonal) similar to corneal endothelial mosaic. The ZO-1 and Na+/K+-ATPase pump markers were highly positive in confluent cell monolayers at 21 days after isolation (passage 0; P0), but significantly decreased in confluent monolayers after the first passage (P1). A weak expression of Ki67 was observed in both P0 and P1 monolayers. The P0 monolayers showed a progressive increase in TEER values between days 6 and 11 and remained stable until day 18 of culture, indicating a state of controlled permeability in monolayers. The P1 monolayers also showed some functional ability but with decreased TEER values compared to monolayers at P0.
Conclusions: Our results indicate that it is possible to obtain functional hCEC cultures in eye banks, using simplified and standardized protocols, from older donor corneas (>60 years of age), previously preserved under organotypic culture conditions. This tissue is more readily available in our setting, due to the profile of the donor population or due to the low endothelial count (<2,000 cells/mm2) of the donated cornea.
Keywords: Cell culture; Cell therapy; Corneal transplant; Endothelial barrier; Endothelial dysfunction; Eye bank.
© 2023 The Author(s). Published by S. Karger AG, Basel.
Conflict of interest statement
The authors have no conflicts of interest to declare.
Figures


Similar articles
-
Proliferative response of corneal endothelial cells from young and older donors.Invest Ophthalmol Vis Sci. 2004 Jun;45(6):1743-51. doi: 10.1167/iovs.03-0814. Invest Ophthalmol Vis Sci. 2004. PMID: 15161835
-
Effects of corneal preservation conditions on human corneal endothelial cell culture.Exp Eye Res. 2019 Feb;179:93-101. doi: 10.1016/j.exer.2018.11.007. Epub 2018 Nov 9. Exp Eye Res. 2019. PMID: 30414971
-
Impact of culture media on primary human corneal endothelial cells derived from old donors.Exp Eye Res. 2024 Mar;240:109815. doi: 10.1016/j.exer.2024.109815. Epub 2024 Feb 3. Exp Eye Res. 2024. PMID: 38316204
-
[Transplantation of corneal endothelial cells].Nippon Ganka Gakkai Zasshi. 2002 Dec;106(12):805-35; discussion 836. Nippon Ganka Gakkai Zasshi. 2002. PMID: 12610838 Review. Japanese.
-
Prospects for endothelial transplantation.Exp Eye Res. 2004 Mar;78(3):573-8. doi: 10.1016/s0014-4835(03)00209-4. Exp Eye Res. 2004. PMID: 15106937 Review.
References
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

