Study of anatomical parameters and intraoperative fluoroscopic techniques for transiliac crest anterograde lag screws fixation of the posterior column of the acetabulum
- PMID: 37723587
- PMCID: PMC10506344
- DOI: 10.1186/s13018-023-04208-3
Study of anatomical parameters and intraoperative fluoroscopic techniques for transiliac crest anterograde lag screws fixation of the posterior column of the acetabulum
Abstract
Background: Currently, there is a lack of research investigating the feasibility of employing anterograde lag screw fixation through the iliac crest for minimally invasive percutaneous treatment of the posterior acetabular column, which encompasses retrograde and anterograde screw fixation in posterior acetabular lag screw fixation. And consequently, the purpose of this study was to examine the anatomical parameters of anterograde lag screw fixation of the posterior column of the pelvis through the iliac crest as well as to investigate the intraoperative fluoroscopy technique, to furnish a scientific rationale supporting the practical utilization of this method within clinical settings.
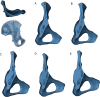
Methods: In this study, pelvic CT data of 60 healthy adults, including 30 males and 30 females, were accumulated. The mimics 21.0 software was developed to reconstruct the three-dimensional pelvis model, simulate the anterograde lag screw fixation of the posterior column of the acetabulum through use of the iliac crest, and precisely identify the insertion point: Utilizing the widest iliac tubercle as the starting point, the insertion point was moved toward the anterior superior iliac spine by 1.0 cm at a time until it reached 4.0 cm. With a total of five insertion points, all oriented toward the lesser sciatic notch, the initial diameter of the virtual screw measured 5.0 mm, and it was progressively enlarged by 1.0 mm increments until reaching a final diameter of 8.0 mm. Besides, the longest lengths of virtual screws with distinct diameters at divergent entry points were measured and compared. At the same time, the intraoperative fluoroscopy technique for optimal access was analyzed.
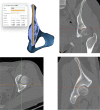
Results: The cross-section from the iliac crest to the lesser sciatic notch was irregular, with multiple curved shapes. Furthermore, the diameter of the screw was determined by the anteroposterior radians and width of the iliac crest plate, while the screw length was determined by the curvature of the square body. On the condition that the screw diameter of the D channel (3.0 cm outward from the widest part of the iliac tubercle to the lesser sciatic notch) was 5 mm, 6 mm as well as 7 mm, the longest screw lengths were (145.6 ± 12.8) mm, (143.6 ± 14.4) mm and (139.9 ± 16.6) mm, correspondingly, indicating statistically substantial distinctions from other channels (P < 0.0001). Intraoperative fluoroscopy demonstrated that the C-arm machine was tilted (60.7 ± 2.9) ° to the iliac at the entrance position and perpendicular to the D-channel at the exit position.
Conclusion: It is possible to use the new channel to fix the posterior column of the acetabulum with an anterograde lag screw through the iliac crest. In specific, the channel is 3.0 cm outward from the widest part of the iliac tubercle to the lesser sciatic notch. Providing a wide channel, long screw insertion, and high safety, this technique offers a novel approach for minimally invasive treatment of posterior column fractures of the acetabulum.
Keywords: Acetabulum; Anatomical parameters; Anterograde lag screws; Internal fixation; Transiliac crest.
© 2023. BioMed Central Ltd., part of Springer Nature.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures

References
MeSH terms
LinkOut - more resources
Full Text Sources

