Waiting Time and Patient Satisfaction in a Subspecialty Eye Hospital Using a Mobile Data Collection Kit: Pre-Post Quality Improvement Intervention
- PMID: 37725529
- PMCID: PMC10414230
- DOI: 10.2196/34263
Waiting Time and Patient Satisfaction in a Subspecialty Eye Hospital Using a Mobile Data Collection Kit: Pre-Post Quality Improvement Intervention
Abstract
Background: Waiting time can considerably increase the cost to both the clinic and the patient and be a major predictor of the satisfaction of eye care users. Efficient management of waiting time remains as a challenge in hospitals. Waiting time management will become even more crucial in the postpandemic era. A key consideration when improving waiting time is the involvement of eye care users. This study aimed at improving patient waiting time and satisfaction through the use of Plan-Do-Study-Act (PDSA) quality improvement cycles.
Objective: The objectives of this study were to determine the waiting time and patient satisfaction, measure the association between waiting time and patient satisfaction, and determine the effectiveness of the PDSA model in improving waiting time and satisfaction.
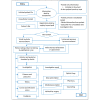
Methods: This was a pre-post quality improvement study among patients aged 19 to 80 years, who are consulting with the Magrabi International Council of Ophthalmology Cameroon Eye Institute. We used PDSA cycles to conduct improvement audits of waiting time and satisfaction over 6 weeks. A data collection app known as Open Data Kit (Get ODK Inc) was used for real-time tracking of waiting, service, and idling times at each service point. Participants were also asked whether they were satisfied with the waiting time at the point of exit. Data from 51% (25/49) preintervention participants and 49% (24/49) postintervention participants were analyzed using Stata 14 at .05 significance level. An unpaired 2-tailed t test was used to assess the statistical significance of the observed differences in times before and after the intervention. Logistic regression was used to examine the association between satisfaction and waiting time.
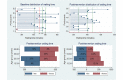
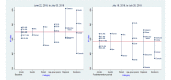
Results: In total, 49 participants were recruited with mean age of 49 (SD 15.7) years. The preintervention mean waiting, service, and idling times were 450 (SD 96.6), 112 (SD 47), and 338 (SD 98.1) minutes, respectively. There was no significant association between patient waiting time and satisfaction (odds ratio 1, 95% CI 0.99-1; P=.37; χ23=0.4). The use of PDSA led to 15% (66 minutes/450 minutes) improvement in waiting time (t47=2; P=.05) and nonsignificant increase in patient satisfaction from 32% (8/25) to 33% (8/24; z=0.1; P=.92).
Conclusions: Use of PDSA led to a borderline statistically significant reduction of 66 minutes in waiting time over 6 weeks and an insignificant improvement in satisfaction, suggesting that quality improvement efforts at the clinic have to be made over a considerable period to be able to produce significant changes. The study provides a good basis for standardizing the cycle (consultation) time at the clinic. We recommend shortening the patient pathway and implementing other measures including a phasic appointment system, automated patient time monitoring, robust ticketing, patient pathway supervision, standard triaging, task shifting, physician consultation planning, patient education, and additional registration staff.
Keywords: clinical audit; ophthalmology; patient satisfaction; patient-centered care; quality improvement; waiting list; waiting time.
©Mathew Mbwogge, Nicholas Astbury, Henry Ebong Nkumbe, Catey Bunce, Covadonga Bascaran. Originally published in JMIRx Med (https://med.jmirx.org), 09.08.2022.
Conflict of interest statement
Conflicts of Interest: None declared.
Figures





Update of
- JMIRx Med. 3:e34263. doi: 10.2196/preprints.34263
References
-
- Kern C, König A, Fu DJ, Schworm B, Wolf A, Priglinger S, Kortuem KU. Big data simulations for capacity improvement in a general ophthalmology clinic. Graefes Arch Clin Exp Ophthalmol. 2021 May;259(5):1289–96. doi: 10.1007/s00417-020-05040-9. http://europepmc.org/abstract/MED/33386963 10.1007/s00417-020-05040-9 - DOI - PMC - PubMed
-
- Abidova A, da Silva PA, Moreira S. The mediating role of patient satisfaction and perceived quality of healthcare in the emergency department. Medicine (Baltimore) 2021 Mar 19;100(11):e25133. doi: 10.1097/MD.0000000000025133. doi: 10.1097/MD.0000000000025133. 00005792-202103190-00075 - DOI - DOI - PMC - PubMed
-
- Abidova A, da Silva PA, Moreira S. Predictors of patient satisfaction and the perceived quality of healthcare in an emergency department in Portugal. West J Emerg Med. 2020 Jan 27;21(2):391–403. doi: 10.5811/westjem.2019.9.44667. http://europepmc.org/abstract/MED/31999247 westjem.2019.9.44667 - DOI - PMC - PubMed
-
- Bruce C, Harrison P, Giammattei C, Desai SN, Sol JR, Jones S, Schwartz R. Evaluating patient-centered mobile health technologies: definitions, methodologies, and outcomes. JMIR Mhealth Uhealth. 2020 Nov 11;8(11):e17577. doi: 10.2196/17577. https://mhealth.jmir.org/2020/11/e17577/ v8i11e17577 - DOI - PMC - PubMed
-
- Jabour AM. The impact of electronic health records on the duration of patients’ visits: time and motion study. JMIR Med Inform. 2020 Feb 07;8(2):e16502. doi: 10.2196/16502. https://medinform.jmir.org/2020/2/e16502/ v8i2e16502 - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources

