Impact of Nonsurgical Periodontal Treatment on Blood Pressure: A Prospective Cohort Study
- PMID: 37729932
- PMCID: PMC11132759
- DOI: 10.1055/s-0043-1772246
Impact of Nonsurgical Periodontal Treatment on Blood Pressure: A Prospective Cohort Study
Abstract
Objectives: Arterial hypertension and periodontitis are two of the most common diseases worldwide and recent evidence supports a causal relationship between them. Despite all antihypertensive strategies, an important number of patients are undiagnosed and a large number of the diagnosed fail to achieve optimal blood pressure (BP) measurements. Some studies point out that periodontal treatment could have positive effects on BP levels. The aim of this study is to determine if nonsurgical periodontal treatment can help BP level control in prehypertensive patients with periodontitis.
Materials and methods: Thirty-five patients were included in the study and received nonsurgical periodontal treatment according to necessity. Clinical data, periodontal data, and BP measurements were taken at baseline, periodontal re-evaluation visit (4-6 weeks after treatment), and 6-month follow-up.
Results: Periodontal treatment caused a statistically significant reduction (p < 0.05) of systolic blood pressure (SBP) and diastolic blood pressure (DBP) at re-evaluation visit of 4.7 (p = 0.016) and 3.4 mm Hg (p = 0.015), respectively. The effect was maintained at 6-month follow-up visit with a reduction in SBP and DBP of 5.2 (p = 0.007) and 3.7 (p = 0.003) mm Hg, respectively.
Conclusion: Despite the limitations of this study, it suggests that nonsurgical periodontal treatment can be effective in lowering BP levels in patients with prehypertension and periodontitis. Moreover, it highlights the importance of dentists in prevention, detection, and control of this important cardiovascular risk factor.
The Author(s). This is an open access article published by Thieme under the terms of the Creative Commons Attribution License, permitting unrestricted use, distribution, and reproduction so long as the original work is properly cited. (https://creativecommons.org/licenses/by/4.0/).
Conflict of interest statement
None declared.
Figures


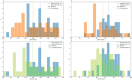

References
-
- GBD 2017 Risk Factor Collaborators Global, regional, and national comparative risk assessment of 84 behavioural, environmental and occupational, and metabolic risks or clusters of risks for 195 countries and territories, 1990-2017: a systematic analysis for the Global Burden of Disease Study 2017 Lancet 2018392(10159):1923–1994. - PMC - PubMed
-
- ESC Scientific Document Group . Williams B, Mancia G, Spiering W et al. 2018 ESC/ESH Guidelines for the management of arterial hypertension. Eur Heart J. 2018;39(33):3021–3104. - PubMed
-
- Drummond G R, Vinh A, Guzik T J, Sobey C G. Immune mechanisms of hypertension. Nat Rev Immunol. 2019;19(08):517–532. - PubMed
-
- Kotseva K, De Backer G, De Bacquer D et al. Lifestyle and impact on cardiovascular risk factor control in coronary patients across 27 countries: Results from the European Society of Cardiology ESC-EORP EUROASPIRE V registry. Eur J Prev Cardiol. 2019;26(08):824–835. - PubMed
-
- Egan B M, Stevens-Fabry S. Prehypertension–prevalence, health risks, and management strategies. Nat Rev Cardiol. 2015;12(05):289–300. - PubMed
LinkOut - more resources
Full Text Sources

