Impact of oral/dental disease burden on postoperative infective complications: a prospective cohort study
- PMID: 37730892
- PMCID: PMC10630249
- DOI: 10.1007/s00784-023-05251-4
Impact of oral/dental disease burden on postoperative infective complications: a prospective cohort study
Abstract
Objectives: This prospective cohort study aimed to assess the association between dental disease burden and postoperative infective complications (POICs) in patients undergoing major surgical procedures under general anaesthesia.
Methods: Pre-surgical dental assessment was undertaken on patients planned for major surgery. Demographic and surgical variables including putative risk factors for POICs and POIC status were documented. The univariable association between POIC status and each factor was examined. Those variables associated at P value ≤ 0.2 were candidates for inclusion in multiple logistic regression models. Backward stepwise variable selection was used to identify the independent predictors for POIC in the best fitting logistic regression model. The area under the receiver operating curve (AUC) was used to quantify the model's global classification performance.
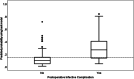
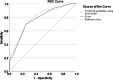
Results: Among the 285 patients, 49 patients (17.2%) had POICs. The independent predictors for POIC were expected length of hospital stay (4-6 days; odds ratio [OR] = 4.80, 95% confidence internal [CI]: 1.30-17.70, P = 0.018, 7-9 days; OR = 5.42, 95% CI: 1.51-19.41, P = 0.009, ≥ 10 days; OR = 28.80, 95% CI: 4.12-201.18, P < 0.001), four or more decayed teeth (OR = 6.03, 95% CI: 2.28-15.94, P < 0.001) and visible tongue plaque (OR = 3.21, 95% CI: 1.54-6.70, P = 0.002). The AUC was 0.78 (95% CI: 0.71-0.85) indicating good discrimination. A simple screening tool for POIC was developed.
Conclusions/clinical relevance: In addition to systemic/surgical factors, this study identified clinically detected decayed teeth and visible tongue plaque as independent predictors for POICs. Preoperative dental assessment/care might be beneficial to assess risk for POICs and improve postoperative outcomes.
Keywords: Oral bacteria; Postoperative infective complications; Preoperative dental care.
© 2023. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures

Similar articles
-
Is Outpatient Management of Mandibular Fractures Associated With Inflammatory Complications? An ACS-NSQIP Study.J Oral Maxillofac Surg. 2021 Dec;79(12):2507-2518. doi: 10.1016/j.joms.2021.03.018. Epub 2021 Mar 26. J Oral Maxillofac Surg. 2021. PMID: 33964241
-
Clinical impact of periodontal disease on postoperative complications in gastrointestinal cancer patients.Int J Clin Oncol. 2019 Dec;24(12):1558-1564. doi: 10.1007/s10147-019-01513-y. Epub 2019 Jul 22. Int J Clin Oncol. 2019. PMID: 31332612
-
Can Patients With Isolated Mandibular Fractures Be Treated as Outpatients?J Oral Maxillofac Surg. 2020 Nov;78(11):2010-2017. doi: 10.1016/j.joms.2020.06.034. Epub 2020 Jul 8. J Oral Maxillofac Surg. 2020. PMID: 32735787
-
Perioperative nutrition for the treatment of bladder cancer by radical cystectomy.Cochrane Database Syst Rev. 2019 May 20;5(5):CD010127. doi: 10.1002/14651858.CD010127.pub2. Cochrane Database Syst Rev. 2019. PMID: 31107970 Free PMC article.
-
Perioperative alcohol cessation intervention for postoperative complications.Cochrane Database Syst Rev. 2018 Nov 8;11(11):CD008343. doi: 10.1002/14651858.CD008343.pub3. Cochrane Database Syst Rev. 2018. PMID: 30408162 Free PMC article.
Cited by
-
Injectable bioactive scaffold able to stimulate oral bone regeneration on demand.J Mater Sci Mater Med. 2025 Apr 8;36(1):31. doi: 10.1007/s10856-025-06879-2. J Mater Sci Mater Med. 2025. PMID: 40198381 Free PMC article.
References
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

