Pathophysiologic Basis of Connected Health Systems
- PMID: 37733435
- PMCID: PMC10557002
- DOI: 10.2196/42405
Pathophysiologic Basis of Connected Health Systems
Abstract
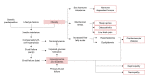
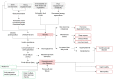
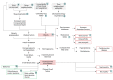
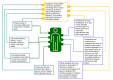
Since the start of the COVID-19 pandemic, there has been a rapid transition to telehealth across the United States, primarily involving virtual clinic visits. Additionally, the proliferation of consumer technologies related to health reveals that for many people health and care in the contemporary world extends beyond the boundaries of a clinical interaction and includes sensors and devices that facilitate health in personal environments. The ideal connected environment is networked and intelligent, personalized to promote health and prevent disease. The combination of sensors, devices, and intelligence constitutes a connected health system around an individual that is optimized to improve and maintain health, deliver care, and predict and reduce risk of illness. Just as modern medicine uses the pathophysiology of disease as a framework for the basis of pharmacologic therapy, a similar clinically reasoned approach can be taken to organize and architect technological elements into therapeutic systems. In this work, we introduce a systematic methodology for the design of connected health systems grounded in the pathophysiologic basis of disease. As the digital landscape expands with the ubiquity of health devices, it is pivotal to enable technology-agnostic clinical reasoning to guide the integration of technological innovations into systems of health and care delivery that extend beyond the boundaries of a clinical interaction. Applying clinical reasoning in a repeatable and systematic way to organizing technology into therapeutic systems can yield potential benefits including expanding the study of digital therapeutics from individual devices to networked technologies as therapeutic interventions; empowering physicians who are not technological experts to still play a significant role in using clinical reasoning for architecting therapeutic networks of sensors and devices; and developing platforms to catalog and share combinations of technologies that can form therapeutic networks and connected health systems.
Keywords: architecting connected health systems; clinic; community; connected health; design; digital therapeutic; environment; pathophysiology; smart health; system; systematic methodology; technology; therapeutic systems.
©Yahya Shaikh, Michael Christopher Gibbons. Originally published in the Journal of Medical Internet Research (https://www.jmir.org), 21.09.2023.
Conflict of interest statement
Conflicts of Interest: None declared.
Figures
Similar articles
-
The future of Cochrane Neonatal.Early Hum Dev. 2020 Nov;150:105191. doi: 10.1016/j.earlhumdev.2020.105191. Epub 2020 Sep 12. Early Hum Dev. 2020. PMID: 33036834
-
New and emerging technology for adult social care - the example of home sensors with artificial intelligence (AI) technology.Health Soc Care Deliv Res. 2023 Jun;11(9):1-64. doi: 10.3310/HRYW4281. Health Soc Care Deliv Res. 2023. PMID: 37470136
-
Clinical Integration of Digital Solutions in Health Care: An Overview of the Current Landscape of Digital Technologies in Cancer Care.JCO Clin Cancer Inform. 2018 Dec;2:1-9. doi: 10.1200/CCI.17.00159. JCO Clin Cancer Inform. 2018. PMID: 30652580 Review.
-
Digital Orientation of Health Systems in the Post-COVID-19 "New Normal" in the United States: Cross-sectional Survey.J Med Internet Res. 2021 Aug 16;23(8):e30453. doi: 10.2196/30453. J Med Internet Res. 2021. PMID: 34254947 Free PMC article.
-
COVID-19 what have we learned? The rise of social machines and connected devices in pandemic management following the concepts of predictive, preventive and personalized medicine.EPMA J. 2020 Jul 30;11(3):311-332. doi: 10.1007/s13167-020-00218-x. eCollection 2020 Sep. EPMA J. 2020. PMID: 32839666 Free PMC article. Review.
Cited by
-
Opportunities for digitally-enabled personalization and decision support for pediatric growth hormone therapy.Front Endocrinol (Lausanne). 2024 Oct 15;15:1436778. doi: 10.3389/fendo.2024.1436778. eCollection 2024. Front Endocrinol (Lausanne). 2024. PMID: 39473505 Free PMC article. Review.
-
A Digital Mask-Voiceprint System for Postpandemic Surveillance and Tracing Based on the STRONG Strategy.J Med Internet Res. 2023 Nov 6;25:e44795. doi: 10.2196/44795. J Med Internet Res. 2023. PMID: 37856760 Free PMC article.
References
-
- Koonin LM, Hoots B, Tsang CA, Leroy Z, Farris K, Jolly B, Antall P, McCabe B, Zelis CBR, Tong I, Harris AM. Trends in the use of telehealth during the emergence of the COVID-19 pandemic—United States, January-March 2020. MMWR Morb Mortal Wkly Rep. 2020;69(43):1595–1599. doi: 10.15585/mmwr.mm6943a3. https://www.cdc.gov/mmwr/volumes/69/wr/mm6943a3.htm?s_cid=mm6943a3_w - DOI - PMC - PubMed
-
- Shen YT, Chen L, Yue WW, Xu HX. Digital technology-based telemedicine for the COVID-19 pandemic. Front Med (Lausanne) 2021;8:646506. doi: 10.3389/fmed.2021.646506. https://www.frontiersin.org/articles/10.3389/fmed.2021.646506/full - DOI - DOI - PMC - PubMed
-
- Franchini M, Pieroni S, Martini N, Ripoli A, Chiappino D, Denoth F, Liebman MN, Molinaro S, Della Latta D. Shifting the paradigm: the Dress-COV telegram bot as a tool for participatory medicine. Int J Environ Res Public Health. 2020;17(23):8786. doi: 10.3390/ijerph17238786. https://www.mdpi.com/1660-4601/17/23/8786 ijerph17238786 - DOI - PMC - PubMed
-
- Franchini M, Molinaro S, Caiolfa M, Salvatori M, Pieroni S. Facing the national recovery and resilience plan: sources of data, indicators, and participatory strategies in healthcare and social fields. Int J Environ Res Public Health. 2021;18(19):10457. doi: 10.3390/ijerph181910457. https://www.mdpi.com/1660-4601/18/19/10457 ijerph181910457 - DOI - PMC - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials

