Transperineal laser ablation as a new minimally invasive surgical therapy for benign prostatic hyperplasia: a systematic review of existing literature
- PMID: 37745187
- PMCID: PMC10515526
- DOI: 10.1177/17562872231198634
Transperineal laser ablation as a new minimally invasive surgical therapy for benign prostatic hyperplasia: a systematic review of existing literature
Abstract
Introduction: Transperineal laser ablation (TPLA) of the prostate is a new, minimally invasive technique for benign prostatic hyperplasia (BPH) with promising effectiveness and safety outcomes. This systematic review aims to provide an update of existing literature.
Methods: A literature review was performed in Pubmed/MEDLINE, Embase, Cochrane Library, and clinicaltrials.gov from January 2000 up to April 2023. Data extraction and risk of bias were performed independently by three authors.
Results: A total of 11 studies were included, among which 9 were observational, 1 randomized controlled trial, 1 animal study, while 2 of them were comparative (1 with prostatic artery embolization and 1 with transurethral resection of the prostate). Functional outcomes were improved in the majority of studies both for objective (maximum flow rate and post-void residual) and subjective outcomes (improvement of International Prostate Symptom Score and quality of life). Complication rates ranged between 1.9% and 2.3% for hematuria, 3.7% and 36.3% for dysuria, 1.9% and 19% for acute urinary retention, 0.6% and 9.1% for orchitis/urinary tract infections, and 0.6% and 4.8% for prostatic abscess formation. Regarding sexual function, >95% of patients retained their ejaculation while erectile function was maintained or improved.
Conclusion: TPLA of the prostate is an innovative, minimally invasive technique for managing patients with BPH. Existing studies indicate an effective technique in reducing International Prostate Symptom Score and quality of life scores, post-void residual reduction, and increase in Qmax, albeit the measured improvements in terms of Qmax are not equal to transurethral resection of the prostate. Although sexual function is maintained, the mean catheterization time is 7 days, and no long-term data are available for most patients.
Keywords: BPH; LUTS; TPLA; laser; laser ablation; prostate.
© The Author(s), 2023.
Conflict of interest statement
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Figures

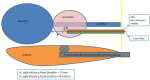


References
-
- Gravas SCJ, Gacci M, Gratzke C, et al.. EAU Guidelines on management of non-neurogenic male lower urinary tract symptoms (LUTS), incl. benign prostatic obstruction (BPO). In: Paper presented at the EAU annual congress, Amsterdam, 2022. Available at: https://d56bochluxqnz.cloudfront.net/documents/full-guideline/EAU-Guidel.... accessed 1 May 2023.
-
- Egan KB, Burnett AL, McVary KT, et al.. The co-occurring syndrome-coexisting erectile dysfunction and benign prostatic hyperplasia and their clinical correlates in aging men: results from the national health and nutrition examination survey. Urology 2015; 86: 570–580. - PubMed
-
- Herrmann TRW. Enucleation is enucleation is enucleation is enucleation. World J Urol 2016; 34: 1353–1355. - PubMed
-
- Ahyai SA, Gilling P, Kaplan SA, et al.. Meta-analysis of functional outcomes and complications following transurethral procedures for lower urinary tract symptoms resulting from benign prostatic enlargement. Eur Urol 2010; 58: 384–397. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous

