Patient-reported outcome, perception and satisfaction after laparoscopic cholecystectomy in Kigali, Rwanda
- PMID: 37745196
- PMCID: PMC10514211
- DOI: 10.1016/j.sopen.2023.09.008
Patient-reported outcome, perception and satisfaction after laparoscopic cholecystectomy in Kigali, Rwanda
Abstract
Background: Laparoscopic surgery is the gold standard for many abdominal surgeries. Laparoscopic programs in low- and middle-income countries (LMICs) and in sub-Saharan Africa face many constraints, although its use is safe, feasible, and clinically beneficial. The authors assessed patient-reported outcomes and the experience of patients operated on at the University Teaching Hospital of Kigali (CHUK).
Methods: This is a retrospective cross-sectional study combining medical data from medical files and information collected from telephone calls to 288 patients who underwent laparoscopic cholecystectomy at CHUK from January 2015 to December 2020.
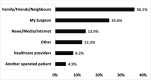
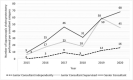
Results: Among 446 laparoscopic surgeries performed at CHUK over 6 years, cholecystectomies accounted for 64.6 % of cases (288/446). Postoperative complications and mortality after laparoscopic cholecystectomy were low, respectively 1.7 % and 0.7 %, while the median length of stay was 3 days. About 74 % of surveyed patients had never heard of laparoscopic surgery prior to their procedure. Knowledge of laparoscopic surgery was associated with patient education level (p < 0.001). Half of patients had not been involved in the choice of the surgical technique. Overall satisfaction was over 95 % and >90 % of patients consider laparoscopic surgery as the best surgical approach in Rwanda, and for this reason they declared to be ready to promote this new technology despite its higher cost. However, patients reported some weaknesses and made recommendations for improving public awareness of laparoscopy and its benefits, patient-provider relationships, training of surgical workforce, laparoscopic equipment, and infrastructure.
Conclusion: Laparoscopic cholecystectomy can be performed with a low rate of postoperative complications in a resource-limited setting like Rwanda. Patient satisfaction was high, but efforts should be made to improve public awareness of laparoscopic surgery, improve surgical capacity, laparoscopic equipment, and infrastructure.
Keywords: Complications; Experience; Laparoscopic cholecystectomy laparoscopic surgery; Minimally invasive surgery; Outcome; Satisfaction.
© 2023 The Authors.
Conflict of interest statement
Dr. Martin Nyundo, Dr. King Kayondo, Dr. Miguel Gasakure, Dr. Jean Christian Urimubabo, Prof. Jean Jacques Houben, Dr. Augustin Limgba, Dr. Antoine Nifasha, Prof. Julien Gashegu and Prof. Olivier Detry declare that they have no conflicts of interest or financial ties to disclose.
Figures
References
-
- Cuschieri A. Laparoscopic surgery: current status, issues and future developments. Surgeon. 2005;3(3):125–138. - PubMed
-
- Mayol J., Garcia-Aguilar J., Ortiz-Oshiro E. Risks of the minimal access approach for laparoscopic surgery: multivariate analysis of morbidity related to umbilical trocar insertion. World J Surg. 1997;21(5):529–533. - PubMed
-
- Manning R.G., Aziz A.Q. Should laparoscopic cholecystectomy be practiced in the developing world? The experience of the first training program in Afghanistan. Ann Surg. 2009;249(5):794–798. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous