Association Between Urologist Merit-Based Incentive Payment System Performance and Quality of Prostate Cancer Care
- PMID: 37748132
- PMCID: PMC10842494
- DOI: 10.1097/UPJ.0000000000000463
Association Between Urologist Merit-Based Incentive Payment System Performance and Quality of Prostate Cancer Care
Abstract
Introduction: We performed a study to evaluate the association between urologist performance in the Merit-Based Incentive Payment System (MIPS), and quality and spending for prostate cancer care.
Methods: Medicare beneficiaries with prostate cancer diagnosed between 2017 and 2019 were assigned to their primary urologist. Associated MIPS scores were identified and categorized based on thresholds for payment adjustment as low (worst), moderate, and high (best). Multivariable mixed effects models were used to measure the association between MIPS performance and adherence to quality measures and price standardized spending for prostate cancer.
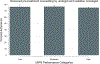
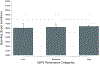
Results: Adherence to quality measures did not vary across MIPS performance groups for pretreatment counselling by both a urologist and radiation oncologist (low-76%, [95% CI 73%-80%], moderate-77% [95% CI 74%-79%], and high-75% [95% CI 74%-76%]) and avoiding treatment in men with a high risk of noncancer mortality within 10 years of diagnosis (low-40% [95% CI 35%-45%], moderate-39% [95% CI 36%-43%], high-38% [95% CI 36%-39%]). Men on active surveillance managed by high performers more likely received a confirmatory test (44% [95% CI 43%-46%]) compared to those managed by moderate (38% [95% CI 33%-42%]) performers, but not low performers (36% [95% CI 29%-44%]). There was no difference in adjusted spending across MIPS performance groups.
Conclusions: Better performance in MIPS is associated with a higher rate of confirmatory testing in men initiating active surveillance for prostate cancer. However, performance was not associated with other dimensions of quality nor spending.
Keywords: Medicare; prostate cancer; quality; value-based care.
Figures



Comment in
-
Editorial Comment.Urol Pract. 2024 Jan;11(1):215-216. doi: 10.1097/UPJ.0000000000000463.02. Epub 2023 Nov 9. Urol Pract. 2024. PMID: 37943982 No abstract available.
Similar articles
-
Value-based payment models and management of newly diagnosed prostate cancer.Cancer Med. 2024 Jan;13(1):e6810. doi: 10.1002/cam4.6810. Epub 2023 Dec 26. Cancer Med. 2024. PMID: 38146905 Free PMC article.
-
Implications of the Merit-Based Incentive Payment System for Urology Practices.Urology. 2022 Nov;169:84-91. doi: 10.1016/j.urology.2022.05.052. Epub 2022 Aug 3. Urology. 2022. PMID: 35932872 Free PMC article.
-
How Did Orthopaedic Surgeons Perform in the 2018 Centers for Medicaid & Medicare Services Merit-based Incentive Payment System?Clin Orthop Relat Res. 2022 Jan 1;480(1):8-22. doi: 10.1097/CORR.0000000000001981. Clin Orthop Relat Res. 2022. PMID: 34543249 Free PMC article.
-
The Merit-based Incentive Payment System (MIPS): A Primer for Otolaryngologists.Otolaryngol Head Neck Surg. 2018 Sep;159(3):410-413. doi: 10.1177/0194599818774033. Epub 2018 May 8. Otolaryngol Head Neck Surg. 2018. PMID: 29734874 Review.
-
MACRA 2.0: are you ready for MIPS?J Neurointerv Surg. 2017 Jul;9(7):714-716. doi: 10.1136/neurintsurg-2016-012845. Epub 2016 Nov 24. J Neurointerv Surg. 2017. PMID: 27884928 Review.
Cited by
-
Spillover Effects of Medicare Advantage on Traditional Medicare Beneficiaries With Prostate Cancer.Cancer Med. 2025 Mar;14(6):e70796. doi: 10.1002/cam4.70796. Cancer Med. 2025. PMID: 40111071 Free PMC article.
-
Commercial prices and their influence on urology practices: Prostate cancer care among men with Medicare.Cancer. 2025 Jan 1;131(1):e35633. doi: 10.1002/cncr.35633. Epub 2024 Nov 5. Cancer. 2025. PMID: 39501423
-
Physician Payment Incentives and Active Surveillance in Low-Risk Prostate Cancer.JAMA Netw Open. 2025 Jan 2;8(1):e2453658. doi: 10.1001/jamanetworkopen.2024.53658. JAMA Netw Open. 2025. PMID: 39775806 Free PMC article.
References
-
- Key Statistics for Prostate Cancer | Prostate Cancer Facts. Accessed February 15, 2023. https://www.cancer.org/cancer/prostate-cancer/about/key-statistics.html
-
- CMS. Merit-based Incentive Payment System (MIPS) Overview - QPP. Accessed November 15, 2021. https://qpp.cms.gov/mips/overview
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

