A Prediction Model for In-Hospital Mortality of Acute Exacerbations of Chronic Obstructive Pulmonary Disease Patients Based on Red Cell Distribution Width-to-Platelet Ratio
- PMID: 37750166
- PMCID: PMC10518148
- DOI: 10.2147/COPD.S418162
A Prediction Model for In-Hospital Mortality of Acute Exacerbations of Chronic Obstructive Pulmonary Disease Patients Based on Red Cell Distribution Width-to-Platelet Ratio
Abstract
Purpose: To explore the association between red cell distribution width (RDW)-to-platelet ratio (RPR) and in-hospital mortality of acute exacerbations of chronic obstructive pulmonary disease (AECOPD) patients and establish a prediction model based on RPR and other predictors.
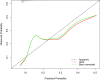
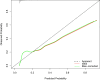
Material and methods: This cohort study included 1922 AECOPD patients aged ≥18 years in the Medical Information Mart for Intensive Care (MIMIC)-III and MIMIC-IV as well as 1738 AECOPD patients from eICU Collaborative Research Database (eICU-CRD). Possible confounding factors were screened out by univariate logistic regression, and multivariable logistic regression was applied to evaluate the association between RPR and in-hospital mortality of AECOPD patients. The area under the curve (AUC), calibration curve and decision curve analysis (DCA) curve were plotted to evaluate the predictive value of the model. The median follow-up time was 3.14 (1.87, 6.25) day.
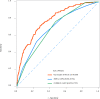
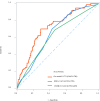
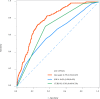
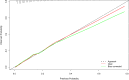
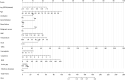
Results: At the end of follow-up, there were 1660 patients survived and 262 subjects died. After adjusting for confounders, we found that Log (RPR×1000) was linked with elevated risk of in-hospital mortality of AECOPD patients [odds ratio (OR)=1.36, 95% confidence interval (CI): 1.01-1.84]. The prediction model was constructed using predictors including Log (RPR×1000), age, malignant cancer, atrial fibrillation, ventilation, renal failure, diastolic blood pressure (DBP), temperature, Glasgow Coma Scale (GCS) score, white blood cell (WBC), creatinine, blood urea nitrogen (BUN), hemoglobin, infectious diseases and anion gap. The AUC of the prediction model was 0.785 (95% CI: 0.751-0.820) in the training set, 0.721 (95% CI: 0.662-0.780) in the testing set, and 0.795 (95% CI: 0.762-0.827) in the validation set.
Conclusion: RPR was associated with the in-hospital mortality of AECOPD patients. The prediction model for the in-hospital mortality of AECOPD patients based on RPR and other predictors presented good predictive performance, which might help the clinicians to quickly identify AECOPD patients at high risk of in-hospital mortality.
Keywords: acute exacerbations of chronic obstructive pulmonary disease; platelet ratio; red cell distribution width; red cell distribution width-to-platelet ratio.
© 2023 Chen et al.
Conflict of interest statement
The authors report no conflicts of interest in this work.
Figures
Similar articles
-
Red Blood Cell Distribution Width/Hematocrit Ratio: A New Predictor of 28 Days All-Cause Mortality of AECOPD Patients in ICU.Int J Chron Obstruct Pulmon Dis. 2024 Nov 22;19:2497-2516. doi: 10.2147/COPD.S492049. eCollection 2024. Int J Chron Obstruct Pulmon Dis. 2024. PMID: 39600310 Free PMC article.
-
[Establishment and evaluation of early in-hospital death prediction model for patients with acute pancreatitis in intensive care unit].Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2023 Aug;35(8):865-869. doi: 10.3760/cma.j.cn121430-20220713-00660. Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2023. PMID: 37593868 Chinese.
-
The Relationship Between Blood Urea Nitrogen to Creatinine Ratio and Severe Acute Exacerbation of COPD Patients: A Propensity Score Matching Study.Int J Chron Obstruct Pulmon Dis. 2024 Nov 25;19:2529-2543. doi: 10.2147/COPD.S488394. eCollection 2024. Int J Chron Obstruct Pulmon Dis. 2024. PMID: 39618501 Free PMC article.
-
DECAF score as a mortality predictor for acute exacerbation of chronic obstructive pulmonary disease: a systematic review and meta-analysis.BMJ Open. 2020 Oct 30;10(10):e037923. doi: 10.1136/bmjopen-2020-037923. BMJ Open. 2020. PMID: 33127631 Free PMC article.
-
A pooled analysis of the risk prediction models for mortality in acute exacerbation of chronic obstructive pulmonary disease.Clin Respir J. 2023 Aug;17(8):707-718. doi: 10.1111/crj.13606. Epub 2023 Mar 21. Clin Respir J. 2023. PMID: 36945821 Free PMC article. Review.
Cited by
-
Prognostic Significance of Red Blood Cell Distribution Width-to-Albumin Ratio in Predicting 1-Year Mortality for Critically Ill Chronic Obstructive Pulmonary Disease Patients.Balkan Med J. 2025 May 5;42(3):222-232. doi: 10.4274/balkanmedj.galenos.2025.2025-1-141. Balkan Med J. 2025. PMID: 40326842 Free PMC article.
-
Association between COPD and CKD: a systematic review and meta-analysis.Front Public Health. 2024 Dec 16;12:1494291. doi: 10.3389/fpubh.2024.1494291. eCollection 2024. Front Public Health. 2024. PMID: 39737452 Free PMC article.
-
Prognostic risk prediction model for patients with acute exacerbation of chronic obstructive pulmonary disease (AECOPD): a systematic review and meta-analysis.Respir Res. 2024 Nov 14;25(1):410. doi: 10.1186/s12931-024-03033-4. Respir Res. 2024. PMID: 39543648 Free PMC article.
-
Development and Validation of an In-Hospital Mortality Prediction Model for Patients with Acute Exacerbation of Chronic Obstructive Pulmonary Disease.Int J Chron Obstruct Pulmon Dis. 2024 Jun 12;19:1303-1314. doi: 10.2147/COPD.S461269. eCollection 2024. Int J Chron Obstruct Pulmon Dis. 2024. PMID: 38881715 Free PMC article.
-
Unveiling the Prognostic Power of HRR in ICU-Admitted COPD Patients: A MIMIC-IV Database Study.Int J Chron Obstruct Pulmon Dis. 2025 Jan 6;20:11-21. doi: 10.2147/COPD.S482344. eCollection 2025. Int J Chron Obstruct Pulmon Dis. 2025. PMID: 39802039 Free PMC article.
References
-
- Zhang D, Zhang H, Li X, et al. Pulmonary rehabilitation programmes within three days of hospitalization for acute exacerbation of chronic obstructive pulmonary disease: a systematic review and meta-analysis. Int J Chron Obstruct Pulmon Dis. 2021;16:3525–3538. doi:10.2147/COPD.S338074 - DOI - PMC - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

