Prevalence and Risk Factors for High-Risk Human Papillomavirus Infection and Cervical Disorders: Baseline Findings From an Human Papillomavirus Cohort Study
- PMID: 37751562
- PMCID: PMC10524074
- DOI: 10.1177/10732748231202925
Prevalence and Risk Factors for High-Risk Human Papillomavirus Infection and Cervical Disorders: Baseline Findings From an Human Papillomavirus Cohort Study
Abstract
Background: A persistent infection by high-risk human papillomavirus (HR-HPV) is a prerequisite for the development of cervical neoplasms; however, most studies have focused on risk factors associated with HPV-16 and HPV-18 only.
Objectives: We assessed the association of risk factors with the prevalence of HPV-16, HPV-18, and non-16/18 HR-HPV infection and with the occurrence of cervical lesions in the baseline of a cohort study of HPV persistence in a Mexican population.
Methods: Cross-sectional study within the baseline of a 5-year dynamic cohort study of HR-HPV persistence in women with an abnormal cytology study result from 2015 to 2021. HPV DNA was detected using the Anyplex II HPV 28 kit. Data on lifestyle, sociodemographic, and reproductive factors were assessed using bivariate and multivariate analyses to determine the association of risk factors with HR-HPV infection status and histopathologic diagnosis.
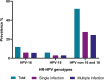
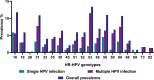
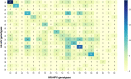
Results: A total of 373 women were included in the study. The overall prevalence of HR-HPV infection was 69.97%. The most prevalent HR-HPV genotypes, including single and multiple infections, were HPV-53 (13.4%), HPV-16 (11.8%), HPV-58 (10.9%), HPV-31 (10.9%), and HPV-66 (10.7%). We found 90 multiple HR-HPV infection patterns, all of them with α-6 and -9 species. Significant associations of multiple HPV-16 and non-16/18 HR-HPV infections were found with marital status, number of lifetime sexual partners, and smoking history. The most prevalent genotype in CIN1 and CIN2 patients was HPV-16. No association was found between biological plausibility risk factors and cervical lesions.
Conclusions: The risk factors for non-16/18 HR-HPV multiple infections are no different than those linked to HPV-16 multiple infections.
Keywords: cervical neoplasm; human papillomavirus infection; risk factors; squamous intraepithelial lesions.
Conflict of interest statement
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Figures

Similar articles
-
Assessment of high-risk human papillomavirus infections and associated cervical dysplasia in HIV-positive pregnant women in Germany: a prospective cross-sectional two-centre study.Arch Gynecol Obstet. 2023 Jul;308(1):207-218. doi: 10.1007/s00404-022-06890-w. Epub 2022 Dec 28. Arch Gynecol Obstet. 2023. PMID: 36576558
-
Prevalence of Human Papillomavirus Genotypes Among Women With High-Grade Cervical Lesions in Beijing, China.Medicine (Baltimore). 2016 Jan;95(3):e2555. doi: 10.1097/MD.0000000000002555. Medicine (Baltimore). 2016. PMID: 26817906 Free PMC article.
-
[Association between high risk human papillomavirus DNA load and cervical lesions in different infection status].Zhonghua Zhong Liu Za Zhi. 2018 Jun 23;40(6):475-480. doi: 10.3760/cma.j.issn.0253-3766.2018.06.015. Zhonghua Zhong Liu Za Zhi. 2018. PMID: 29936777 Chinese.
-
Prevalence and genotype distribution of human papillomavirus infection among female outpatients in Northeast China: a population-based survey of 110,927 women.Arch Gynecol Obstet. 2023 Jul;308(1):35-41. doi: 10.1007/s00404-022-06653-7. Epub 2022 Jul 29. Arch Gynecol Obstet. 2023. PMID: 35904609 Review.
-
Distribution patterns of human papillomavirus genotypes among women in Guangzhou, China.Infect Agent Cancer. 2023 Oct 31;18(1):67. doi: 10.1186/s13027-023-00541-8. Infect Agent Cancer. 2023. PMID: 37907979 Free PMC article. Review.
Cited by
-
HPV prevalence and genotype distribution among women in sanming, China: a retrospective analysis before large-scale vaccination.Infect Agent Cancer. 2025 Jul 9;20(1):45. doi: 10.1186/s13027-025-00678-8. Infect Agent Cancer. 2025. PMID: 40635065 Free PMC article.
-
Investigation and analysis of female HPV infection and genotype distribution in Xuhui District, Shanghai.Virol J. 2025 Mar 5;22(1):59. doi: 10.1186/s12985-025-02663-4. Virol J. 2025. PMID: 40045415 Free PMC article.
-
Cervical cancer screening and risk factor prevalence by sexual identity: A comparison across three national surveys in the United States.Prev Med. 2025 May;194:108262. doi: 10.1016/j.ypmed.2025.108262. Epub 2025 Mar 15. Prev Med. 2025. PMID: 40096895
-
Factors associated with CIN2-3 recurrence: A single center retrospective analysis.Hum Vaccin Immunother. 2025 Dec;21(1):2469410. doi: 10.1080/21645515.2025.2469410. Epub 2025 Feb 21. Hum Vaccin Immunother. 2025. PMID: 39982437 Free PMC article.
-
Characterization of human papillomavirus genotypes and their coverage in vaccine delivered to Ethiopian women.Sci Rep. 2024 Apr 4;14(1):7976. doi: 10.1038/s41598-024-57085-z. Sci Rep. 2024. PMID: 38575600 Free PMC article.
References
MeSH terms
Supplementary concepts
LinkOut - more resources
Full Text Sources

