Inability to get needed health care during the COVID-19 pandemic among a nationally representative, diverse population of U.S. adults with and without chronic conditions
- PMID: 37752511
- PMCID: PMC10523792
- DOI: 10.1186/s12889-023-16746-w
Inability to get needed health care during the COVID-19 pandemic among a nationally representative, diverse population of U.S. adults with and without chronic conditions
Abstract
Background: Delays in health care have been observed in the U.S. during the COVID-19 pandemic; however, the prevalence of inability to get needed care and potential disparities in health care access have yet to be assessed.
Methods: We conducted a nationally representative, online survey of 5,500 American Indian/Alaska Native, Asian, Black/African American, Latino (English- and Spanish-speaking), Native Hawaiian/Pacific Islander, White, and multiracial adults between 12/2020-2/2021 (baseline) and 8/16/2021-9/9/2021 (6-month follow-up). Participants were asked "Since the start of the pandemic, was there any time when you did not get medical care that you needed?" Those who responded "Yes" were asked about the type of care and the reason for not receiving care. Poisson regression was used to estimate the association between sociodemographics and inability to receive needed care; all analyses were stratified by chronic condition status. Chronic conditions included: chronic obstructive pulmonary disease (COPD), heart conditions, type 2 diabetes, chronic kidney disease or on dialysis, sickle cell disease, cancer, and immunocompromised state (weakened immune system).
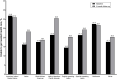
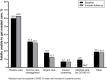
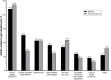
Results: Overall, 20.0% of participants at baseline and 22.7% at follow-up reported not getting needed care. The most common reasons for being unable to get needed care included fear of COVID-19 (baseline: 44.1%; follow-up: 47.2%) and doctors canceled appointment (baseline: 25.3%; follow-up: 14.1%). Routine care (baseline: 59.9%; follow-up: 62.6%) and chronic care management (baseline: 31.5%; follow-up: 30.1%) were the most often reported types of delayed care. Fair/poor self-reported physical health was significantly associated with being unable to get needed care despite chronic condition status (≥ 1 chronic condition: aPR = 1.36, 95%CI = 1.04-1.78); no chronic conditions: aPR = 1.52, 95% CI = 1.28-1.80). The likelihood of inability to get needed care differed in some instances by race/ethnicity, age, and insurance status. For example, uninsured adults were more likely to not get needed care (≥ 1 chronic condition: aPR = 1.76, 95%CI = 1.17-2.66); no chronic conditions: aPR = 1.25, 95% CI = 1.00-1.56).
Conclusions: Overall, about one fifth of participants reported being unable to receive needed care at baseline and follow-up. Delays in receiving needed medical care may exacerbate existing conditions and perpetuate existing health disparities among vulnerable populations who were more likely to have not received needed health care during the pandemic.
Keywords: COVID-19; Chronic diseases; Delayed medical care; Disparities; Unmet health care.
© 2023. BioMed Central Ltd., part of Springer Nature.
Conflict of interest statement
The authors declare no competing interests.
Figures
Similar articles
-
Positive and negative aspects of the COVID-19 pandemic among a diverse sample of US adults: an exploratory mixed-methods analysis of online survey data.BMC Public Health. 2024 Jan 2;24(1):22. doi: 10.1186/s12889-023-17491-w. BMC Public Health. 2024. PMID: 38166883 Free PMC article.
-
Racial/Ethnic Disparities in Financial Hardship During the First Year of the Pandemic.Health Equity. 2023 Aug 30;7(1):453-461. doi: 10.1089/heq.2022.0196. eCollection 2023. Health Equity. 2023. PMID: 37771448 Free PMC article.
-
Racial and ethnic disparities in the association between financial hardship and self-reported weight change during the first year of the pandemic in the U.S.Int J Equity Health. 2024 Jan 22;23(1):12. doi: 10.1186/s12939-023-02093-0. Int J Equity Health. 2024. PMID: 38254081 Free PMC article.
-
Racial and Ethnic Differences in COVID-19 Outcomes, Stressors, Fear, and Prevention Behaviors Among US Women: Web-Based Cross-sectional Study.J Med Internet Res. 2021 Jul 12;23(7):e26296. doi: 10.2196/26296. J Med Internet Res. 2021. PMID: 33819909 Free PMC article.
-
Race and Ethnicity Representation in Phase 2/3 Oncology Clinical Trial Publications: A Systematic Review.JAMA Health Forum. 2024 Jun 7;5(6):e241388. doi: 10.1001/jamahealthforum.2024.1388. JAMA Health Forum. 2024. PMID: 38848090 Free PMC article.
Cited by
-
Recognising the heterogeneity of Indigenous Peoples during the COVID-19 pandemic: a scoping review across Canada, Australia, New Zealand and the USA.BMJ Public Health. 2024 Dec 30;2(2):e001341. doi: 10.1136/bmjph-2024-001341. eCollection 2024 Dec. BMJ Public Health. 2024. PMID: 40018612 Free PMC article.
-
Trends and disparities in mortality due to hypertensive disease and coexisting obesity in the USA: 1999-2023.Egypt Heart J. 2025 Aug 26;77(1):81. doi: 10.1186/s43044-025-00677-5. Egypt Heart J. 2025. PMID: 40856971 Free PMC article.
-
Trends of lower-limb complications in patients with type 2 diabetes mellitus during the COVID-19 pandemic.Diabetes Res Clin Pract. 2025 Aug;226:112331. doi: 10.1016/j.diabres.2025.112331. Epub 2025 Jun 19. Diabetes Res Clin Pract. 2025. PMID: 40543573
-
Socioeconomic factors associated with use of telehealth services in outpatient care settings during the COVID-19.BMC Health Serv Res. 2024 Apr 9;24(1):446. doi: 10.1186/s12913-024-10797-4. BMC Health Serv Res. 2024. PMID: 38594743 Free PMC article.
-
The healthcare burden of pulmonary alveolar proteinosis (PAP).Orphanet J Rare Dis. 2025 Feb 14;20(1):73. doi: 10.1186/s13023-024-03478-2. Orphanet J Rare Dis. 2025. PMID: 39953603 Free PMC article.
References
-
- Factsheet: State action related to delay and resumption of “elective” procedures during COVID-19 pandemic. American Medical Association. 2020. https://www.ama-assn.org/system/files/2020-06/state-elective-procedure-c.... Accessed 12 May 2023.
-
- Centers for Medicare & Medicaid Services (CMS) Recommendations Re-opening Facilities to Provide Non-emergent Non-COVID-19 Healthcare: Phase I. Centers for Medicare & Medicaid Services. 2020. https://www.cms.gov/files/document/covid-flexibility-reopen-essential-no.... Accessed 10 May 2023.
-
- Gonzalez D, Karpman M, Kenney GM, Zuckerman S. Delayed and forgone health care for nonelderly adults during the COVID-19 pandemic. Urban Institute. 2021. https://www.urban.org/research/publication/delayed-and-forgone-health-ca.... Accessed 10 May 2023.
-
- Hamel L, Kearny A, Kirzinger A, Lopes L, Muñana C, Brodie M. Kaiser Family Foundation. KFF Health Tracking Poll - June 2020. https://www.kff.org/report-section/kff-health-tracking-poll-june-2020-so.... Accessed 10 May 2023.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

