Mechanisms and aetiology-dependent treatment of acute liver failure
- PMID: 37752801
- PMCID: PMC11815625
- DOI: 10.1111/liv.15739
Mechanisms and aetiology-dependent treatment of acute liver failure
Abstract
This review compiles the mechanisms of acute liver failure (ALF) as well as the current and potential therapeutic approaches, including aetiology-specific treatment, and the issues encountered with such approaches. On a cellular level, ALF is characterized by massive hepatocyte death due to different types of cellular demise. Compensatory hyperplasia and functional recovery are possible when the regenerative capacity is sufficient to sustain hepatic function. ALF has a high mortality of about 30% and can lead to death in a very short time despite maximum therapeutic intervention. Besides aetiology-specific therapy and intensive care, the therapeutic option of emergency liver transplantation has significantly improved the prognosis of patients with ALF. However, due to limiting factors such as organ shortage, many patients die on the waiting list. In addition to graft assessment, machine perfusion may have the potential to recondition marginal organs and thus expand the organ donor pool.
Keywords: acute liver failure; aetiology; liver transplantation; prediction of prognosis; rebalanced haemostasis; survival markers.
© 2023 The Authors. Liver International published by John Wiley & Sons Ltd.
Conflict of interest statement
The authors have no conflict of interest to disclose.
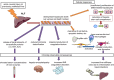
Figures

Similar articles
-
Adult-to-adult living donor liver transplantation for acute liver failure in China.World J Gastroenterol. 2012 Dec 28;18(48):7234-41. doi: 10.3748/wjg.v18.i48.7234. World J Gastroenterol. 2012. PMID: 23326128 Free PMC article.
-
Pediatric acute liver failure in Brazil: Is living donor liver transplantation the best choice for treatment?Liver Transpl. 2016 Jul;22(7):1006-13. doi: 10.1002/lt.24435. Liver Transpl. 2016. PMID: 26946330
-
[Acute liver failure in Korea: etiology, prognosis and treatment].Korean J Hepatol. 2010 Mar;16(1):5-18. doi: 10.3350/kjhep.2010.16.1.5. Korean J Hepatol. 2010. PMID: 20375638 Review. Korean.
-
Management of acute liver failure.Nat Rev Gastroenterol Hepatol. 2009 Sep;6(9):542-53. doi: 10.1038/nrgastro.2009.127. Epub 2009 Aug 4. Nat Rev Gastroenterol Hepatol. 2009. PMID: 19652652 Review.
-
Characteristics, management and outcomes of patients with acute liver failure admitted to Australasian intensive care units.Crit Care Resusc. 2019 Sep;21(3):188-199. Crit Care Resusc. 2019. PMID: 31462206
Cited by
-
Therapeutic effect of hUC-MSCs from different transplantation routes on acute liver failure in rats.Front Med (Lausanne). 2025 May 9;12:1525719. doi: 10.3389/fmed.2025.1525719. eCollection 2025. Front Med (Lausanne). 2025. PMID: 40417693 Free PMC article.
-
HNF4A ameliorates acute liver failure by inhibiting NCOA4-mediated ferritinophagy.Sci Rep. 2025 Aug 13;15(1):29714. doi: 10.1038/s41598-025-13798-3. Sci Rep. 2025. PMID: 40804084 Free PMC article.
-
Changes in TNF-α, IL-33, and MIP-1α before and after artificial liver support treatment and their prognostic value.Am J Transl Res. 2024 Mar 15;16(3):988-997. doi: 10.62347/CBKR4894. eCollection 2024. Am J Transl Res. 2024. PMID: 38586093 Free PMC article.
-
Unraveling the Role of Microcystin-LR in Ferroptosis and Sepsis Pathogenesis: A Comprehensive Review.Biomolecules. 2025 Jun 30;15(7):947. doi: 10.3390/biom15070947. Biomolecules. 2025. PMID: 40723819 Free PMC article. Review.
-
Overview of ferroptosis and pyroptosis in acute liver failure.World J Gastroenterol. 2024 Sep 14;30(34):3856-3861. doi: 10.3748/wjg.v30.i34.3856. World J Gastroenterol. 2024. PMID: 39350783 Free PMC article. Review.
References
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

