Allopurinol for Secondary Prevention in Patients with Cardiovascular Disease: A Systematic Review and Meta-Analysis of Randomized Controlled Trials
- PMID: 37754808
- PMCID: PMC10532321
- DOI: 10.3390/jcdd10090379
Allopurinol for Secondary Prevention in Patients with Cardiovascular Disease: A Systematic Review and Meta-Analysis of Randomized Controlled Trials
Abstract
Background: The effects of allopurinol in patients with cardiovascular disease are not well defined; therefore, the latest evidence is summarized in this study.
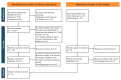
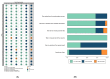
Methods: PubMed, Embase, Cochrane Library, and ClinicalTrials.gov databases were searched for randomized controlled trials (RCTs) of allopurinol in patients with cardiovascular disease published up to 11 February 2023. The primary outcome was cardiovascular death.
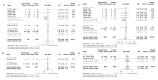
Results: We combined the results of 21 RCTs that included 22,806 patients. Compared to placebo/usual care, allopurinol treatment was not associated with a significant reduction in cardiovascular death (RR 0.60; 95% CI 0.33-1.11) or all-cause death (RR 0.90; 95% CI 0.72-1.12). However, evidence from earlier trials and studies with small sample sizes indicated that allopurinol might confer a protective effect in decreasing cardiovascular death (RR 0.34; 95% CI 0.15-0.76) across patients undergoing coronary artery bypass grafting (CABG) or having acute coronary syndrome (ACS). In comparisons between allopurinol and febuxostat, we observed no difference in cardiovascular death (RR 0.92; 95% CI 0.69-1.24) or all-cause death (RR 1.02; 95% CI 0.75-1.38).
Conclusion: Allopurinol could not reduce cardiovascular (CV) death or major adverse CV outcomes significantly in patients with existing cardiovascular diseases. Given the limitations of the original studies, the potential advantages of allopurinol observed in patients undergoing CABG or presenting with ACS necessitate further confirmation through subsequent RCTs. In the comparisons between allopurinol and febuxostat, our analysis failed to uncover any marked superiority of allopurinol in reducing the risk of adverse cardiovascular incidents.
Keywords: allopurinol; cardiovascular disease; cardiovascular outcomes; febuxostat.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

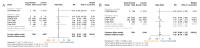

Similar articles
-
Cardiovascular Safety of Febuxostat and Allopurinol in Hyperuricemic Patients With or Without Gout: A Network Meta-Analysis.Front Med (Lausanne). 2021 Jun 15;8:698437. doi: 10.3389/fmed.2021.698437. eCollection 2021. Front Med (Lausanne). 2021. PMID: 34211992 Free PMC article.
-
The major cardiovascular events of febuxostat versus allopurinol in treating gout or asymptomatic hyperuricemia: a systematic review and meta-analysis.Ann Palliat Med. 2021 Oct;10(10):10327-10337. doi: 10.21037/apm-21-1564. Epub 2021 Sep 6. Ann Palliat Med. 2021. PMID: 34498481
-
Cardiovascular safety of febuxostat and allopurinol in patients with gout: A meta-analysis.Front Pharmacol. 2022 Sep 30;13:998441. doi: 10.3389/fphar.2022.998441. eCollection 2022. Front Pharmacol. 2022. PMID: 36249825 Free PMC article.
-
Cardiovascular events in hyperuricemia population and a cardiovascular benefit-risk assessment of urate-lowering therapies: a systematic review and meta-analysis.Chin Med J (Engl). 2020 Apr 20;133(8):982-993. doi: 10.1097/CM9.0000000000000682. Chin Med J (Engl). 2020. PMID: 32106120 Free PMC article.
-
Efficacy of Allopurinol in Cardiovascular Diseases: A Systematic Review and Meta-Analysis.Cardiol Res. 2020 Aug;11(4):226-232. doi: 10.14740/cr1066. Epub 2020 Jun 3. Cardiol Res. 2020. PMID: 32595807 Free PMC article.
Cited by
-
Uric acid elevation in pediatric patients with dilated cardiomyopathy and prediction of mortality.Front Cardiovasc Med. 2024 Jul 23;11:1404755. doi: 10.3389/fcvm.2024.1404755. eCollection 2024. Front Cardiovasc Med. 2024. PMID: 39108665 Free PMC article.
-
Oxidative stress and atrial fibrillation.J Mol Cell Cardiol. 2024 Nov;196:141-151. doi: 10.1016/j.yjmcc.2024.09.011. Epub 2024 Sep 21. J Mol Cell Cardiol. 2024. PMID: 39307416 Review.
-
Uric Acid, Colchicine and Chronic Inflammatory Diseases: A Cardiovascular Perspective.Metabolites. 2025 Jun 20;15(7):424. doi: 10.3390/metabo15070424. Metabolites. 2025. PMID: 40710524 Free PMC article. Review.
-
Uric acid is associated with increased risk of myocardial infarction: results from NHANES 2009-2018 and bidirectional two-sample Mendelian randomization analysis.Front Endocrinol (Lausanne). 2024 Oct 18;15:1424070. doi: 10.3389/fendo.2024.1424070. eCollection 2024. Front Endocrinol (Lausanne). 2024. PMID: 39493770 Free PMC article.
-
Allopurinol use predicts lower low-density lipoprotein cholesterol in patients with pre-dialysis chronic kidney disease-a prospective cohort study.Clin Kidney J. 2024 Dec 9;18(4):sfae400. doi: 10.1093/ckj/sfae400. eCollection 2025 Apr. Clin Kidney J. 2024. PMID: 40600069 Free PMC article.
References
-
- Vos T., Lim S.S., Abbafati C., Abbas K.M., Abbasi M., Abbasifard M., Abbasi-Kangevari M., Abbastabar H., Abd-Allah F., Abdelalim A., et al. Global burden of 369 diseases and injuries in 204 countries and territories, 1990–2019: A systematic analysis for the Global Burden of Disease Study 2019. Lancet. 2020;396:1204–1222. doi: 10.1016/S0140-6736(20)30925-9. - DOI - PMC - PubMed
Publication types
Grants and funding
- 2021YFS0330/Sichuan Science and Technology Program
- 2022ZDZX0030/Sichuan Science and Technology Program
- Sichuan Ganyan ZH2021-101/Sichuan Provincial Cadre Health Research Project, China
- 2021HXFH061/1·3·5 project for disciplines of excellence-Clinical Research Incubation Project, West China Hos-pital, Sichuan University
- 2021-YF05-00665-SN/Chengdu Science and Technology Project
LinkOut - more resources
Full Text Sources

