Harnessing the Native Extracellular Matrix for Periodontal Regeneration Using a Melt Electrowritten Biphasic Scaffold
- PMID: 37754893
- PMCID: PMC10531993
- DOI: 10.3390/jfb14090479
Harnessing the Native Extracellular Matrix for Periodontal Regeneration Using a Melt Electrowritten Biphasic Scaffold
Abstract
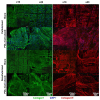
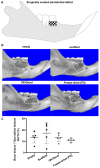
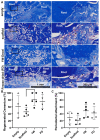
Scaffolds have been used to promote periodontal regeneration by providing control over the spacio-temporal healing of the periodontium (cementum, periodontal ligament (PDL) and alveolar bone). This study proposes to enhance the biofunctionality of a biphasic scaffold for periodontal regeneration by means of cell-laid extracellular matrix (ECM) decoration. To this end, a melt electrowritten scaffold was cultured with human osteoblasts for the deposition of bone-specific ECM. In parallel, periodontal ligament cells were used to form a cell sheet, which was later combined with the bone ECM scaffold to form a biphasic PDL-bone construct. The resulting biphasic construct was decellularised to remove all cellular components while preserving the deposited matrix. Decellularisation efficacy was confirmed in vitro, before the regenerative performance of freshly decellularised constructs was compared to that of 3-months stored freeze-dried scaffolds in a rodent periodontal defect model. Four weeks post-surgery, microCT revealed similar bone formation in all groups. Histology showed higher amounts of newly formed cementum and periodontal attachment in the fresh and freeze-dried ECM functionalised scaffolds, although it did not reach statistical significance. This study demonstrated that the positive effect of ECM decoration was preserved after freeze-drying and storing the construct for 3 months, which has important implications for clinical translation.
Keywords: ECM decoration; additive manufacturing; extracellular matrix; melt electrowriting; polycaprolactone.
Conflict of interest statement
The authors declare no conflict of interest.
Figures


Similar articles
-
Melt electrowriting scaffolds with fibre-guiding features for periodontal attachment.Acta Biomater. 2024 May;180:337-357. doi: 10.1016/j.actbio.2024.04.006. Epub 2024 Apr 5. Acta Biomater. 2024. PMID: 38583749
-
A biphasic scaffold design combined with cell sheet technology for simultaneous regeneration of alveolar bone/periodontal ligament complex.Biomaterials. 2012 Aug;33(22):5560-73. doi: 10.1016/j.biomaterials.2012.04.038. Epub 2012 May 9. Biomaterials. 2012. PMID: 22575832
-
Effect of In Vitro Culture Length on the Bone-Forming Capacity of Osteoblast-Derived Decellularized Extracellular Matrix Melt Electrowritten Scaffolds.Biomacromolecules. 2023 Aug 14;24(8):3450-3462. doi: 10.1021/acs.biomac.2c01504. Epub 2023 Jul 17. Biomacromolecules. 2023. PMID: 37458386
-
Developmental pathways of periodontal tissue regeneration: Developmental diversities of tooth morphogenesis do also map capacity of periodontal tissue regeneration?J Periodontal Res. 2019 Feb;54(1):10-26. doi: 10.1111/jre.12596. Epub 2018 Sep 12. J Periodontal Res. 2019. PMID: 30207395 Review.
-
Multiphasic scaffolds for periodontal tissue engineering.J Dent Res. 2014 Dec;93(12):1212-21. doi: 10.1177/0022034514544301. Epub 2014 Aug 19. J Dent Res. 2014. PMID: 25139362 Free PMC article. Review.
Cited by
-
E7-Conjugated Bio-Inspired Microspheres as a Biological Barrier for Guided Tissue Regeneration.ACS Appl Mater Interfaces. 2023 Dec 20;15(50):58136-58150. doi: 10.1021/acsami.3c12213. Epub 2023 Dec 8. ACS Appl Mater Interfaces. 2023. PMID: 38063848 Free PMC article.
-
The 3-dimensional printing for dental tissue regeneration: the state of the art and future challenges.Front Bioeng Biotechnol. 2024 Feb 22;12:1356580. doi: 10.3389/fbioe.2024.1356580. eCollection 2024. Front Bioeng Biotechnol. 2024. PMID: 38456006 Free PMC article. Review.
References
-
- Jepsen S., Eberhard J., Herrera D., Needleman I. A systematic review of guided tissue regeneration for periodontal furcation defects. What is the effect of guided tissue regeneration compared with surgical debridement in the treatment of furcation defects? J. Clin. Periodontol. 2002;29((Suppl. S3)):103–116; discussion 160–162. doi: 10.1034/j.1600-051X.29.s3.6.x. - DOI - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources

