Ventilatory limitations in patients with HFpEF and obesity
- PMID: 37758032
- PMCID: PMC11079902
- DOI: 10.1016/j.resp.2023.104167
Ventilatory limitations in patients with HFpEF and obesity
Abstract
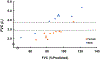
Heart failure with preserved ejection fraction (HFpEF) patients have an increased ventilatory demand. Whether their ventilatory capacity can meet this increased demand is unknown, especially in those with obesity. Body composition (DXA) and pulmonary function were measured in 20 patients with HFpEF (69 ± 6 yr;9 M/11 W). Cardiorespiratory responses, breathing mechanics, and ratings of perceived breathlessness (RPB, 0-10) were measured at rest, 20 W, and peak exercise. FVC correlated with %body fat (R2 =0.51,P = 0.0006), V̇O2peak (%predicted,R2 =0.32,P = 0.001), and RPB (R2 =0.58,P = 0.0004). %Body fat correlated with end-expiratory lung volume at rest (R2 =0.76,P < 0.001), 20 W (R2 =0.72,P < 0.001), and peak exercise (R2 =0.74,P < 0.001). Patients were then divided into two groups: those with lower ventilatory reserve (FVC<3 L,2 M/10 W) and those with higher ventilatory reserve (FVC>3.8 L,7 M/1 W). V̇O2peak was ∼22% less (p < 0.05) and RPB was twice as high at 20 W (p < 0.01) in patients with lower ventilatory reserve. Ventilatory reserves are limited in patients with HFpEF and obesity; indeed, the margin between ventilatory demand and capacity is so narrow that exercise capacity could be ventilatory limited in many patients.
Keywords: Aging; Breathing mechanics; Breathlessness; Exercise capacity; Exercise intolerance; Operational lung volumes; Pulmonary function.
Copyright © 2023 Elsevier B.V. All rights reserved.
Conflict of interest statement
Declaration of Competing Interest No conflicts of interest, financial or otherwise, are declared by the authors.
Figures

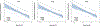

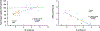
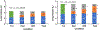
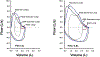
Similar articles
-
Dynamic Ventilatory Reserve During Incremental Exercise: Reference Values and Clinical Validation in Chronic Obstructive Pulmonary Disease.Ann Am Thorac Soc. 2023 Oct;20(10):1425-1434. doi: 10.1513/AnnalsATS.202304-303OC. Ann Am Thorac Soc. 2023. PMID: 37413694
-
Higher Work of Breathing During Exercise in Heart Failure With Preserved Ejection Fraction.Chest. 2023 Jun;163(6):1492-1505. doi: 10.1016/j.chest.2022.11.039. Epub 2022 Dec 5. Chest. 2023. PMID: 36470415 Free PMC article.
-
Haemodynamics, dyspnoea, and pulmonary reserve in heart failure with preserved ejection fraction.Eur Heart J. 2018 Aug 7;39(30):2810-2821. doi: 10.1093/eurheartj/ehy268. Eur Heart J. 2018. PMID: 29788047 Free PMC article.
-
Relative Impairments in Hemodynamic Exercise Reserve Parameters in Heart Failure With Preserved Ejection Fraction: A Study-Level Pooled Analysis.JACC Heart Fail. 2018 Feb;6(2):117-126. doi: 10.1016/j.jchf.2017.10.014. JACC Heart Fail. 2018. PMID: 29413366 Free PMC article. Review.
-
Impaired Exercise Tolerance in Heart Failure With Preserved Ejection Fraction: Quantification of Multiorgan System Reserve Capacity.JACC Heart Fail. 2020 Aug;8(8):605-617. doi: 10.1016/j.jchf.2020.03.008. Epub 2020 Jun 10. JACC Heart Fail. 2020. PMID: 32535122 Free PMC article. Review.
Cited by
-
Identifying the Mechanisms of a Peripherally Limited Exercise Phenotype in Patients With Heart Failure With Preserved Ejection Fraction.Circ Heart Fail. 2024 Aug;17(8):e011693. doi: 10.1161/CIRCHEARTFAILURE.123.011693. Epub 2024 Jul 25. Circ Heart Fail. 2024. PMID: 39051098 Free PMC article. Clinical Trial.
-
Pulmonary gas exchange in relation to exercise pulmonary hypertension in patients with heart failure with preserved ejection fraction.Eur Respir J. 2025 Feb 13;65(2):2400722. doi: 10.1183/13993003.00722-2024. Print 2025 Feb. Eur Respir J. 2025. PMID: 39510552 Free PMC article.
-
Physiologic Phenotyping of Responses to Exercise and Activity in Heart Failure.Circ Res. 2025 Jul 7;137(2):290-315. doi: 10.1161/CIRCRESAHA.125.325534. Epub 2025 Jul 3. Circ Res. 2025. PMID: 40608855 Review.
-
Respiratory symptom perception during exercise in patients with heart failure with preserved ejection fraction.Respir Physiol Neurobiol. 2024 Jul;325:104256. doi: 10.1016/j.resp.2024.104256. Epub 2024 Apr 6. Respir Physiol Neurobiol. 2024. PMID: 38583744 Free PMC article.
-
Heart-Lung Interactions in HFpEF: Dynamic Hyperinflation and Exercise PCWP.JACC Heart Fail. 2025 Aug;13(8):102523. doi: 10.1016/j.jchf.2025.102523. Epub 2025 Jun 26. JACC Heart Fail. 2025. PMID: 40578265 Clinical Trial.
References
-
- Babb TG, 1999. Mechanical ventilatory constraints in aging, lung disease, and obesity: perspectives and brief review. Med Sci. Sports Exerc 31 (1), S12–S22. - PubMed
-
- Babb TG, 2005. Estimation of mechanical ventilatory limitation. J. Qinghai Med. Coll 26, 145–152.
-
- Babb TG, Rodarte JR, 1992. Exercise capacity and breathing mechanics in patients with airflow limitation. Med Sci. Sports Exerc 24, 967–974. - PubMed
-
- Babb TG, Rodarte JR, 1993. Estimation of ventilatory capacity during submaximal exercise. J. Appl. Physiol 74, 2016–2022. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

