MDS-Related Anemia Is Associated with Impaired Quality of Life but Improvement Is Not Always Achieved by Increased Hemoglobin Level
- PMID: 37762806
- PMCID: PMC10532166
- DOI: 10.3390/jcm12185865
MDS-Related Anemia Is Associated with Impaired Quality of Life but Improvement Is Not Always Achieved by Increased Hemoglobin Level
Abstract
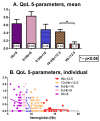
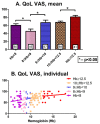
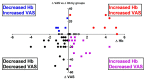
Quality of life is impaired in MDS, but the role of hemoglobin level is unclear. To study the Hb-QoL correlation at diagnosis and 1 year later, patients filled out the EQ-5D questionnaire, assessing their mobility, self care, daily activities, pain/discomfort, and anxiety/depression, using scores of 0 (normal), 1 (mild/moderate), or 2 (poor). They also evaluated their health using a visual analogue scale, scoring from 0 (poor) to 100 (excellent). The anemia subgroups were: none/normal (Hb ≥ 12.5 g/dL), mild (10 ≤ Hb < 12.5), moderate (9 ≤ Hb < 10), severe (8 ≤ Hb < 9), or very severe (Hb < 8). LR-MDS patients (n = 127) and inpatient controls (n = 141) participated. The anemic patients had a poor QoL and the MDS patients had a lower QoL with a lower Hb. The controls had no QoL difference among the various anemia subgroups. In addition, the MDS QoL sharply decreased with an Hb of < 9. The MDS patients showed a wide QoL variability, i.e., different QoL scores in the same Hb subgroup, suggesting that other factors affect QoL (e.g., age and comorbidities). After 1 year (n = 61), the QoL was still poor for most MDS patients (including 27 patients with an increased Hb). In summary: (1) a poor QoL in MDS-anemia is non-linear, suggesting other influencing factors on QoL. (2) The sharp QoL drop with Hb < 9 g/dL challenges the transfusion Hb threshold. (3) The QoL in anemic MDS patients might differ from that in non-MDS patients. (4) Raising Hb, while recommended, does not guarantee an improved QoL.
Keywords: anemia; myelodysplastic neoplasms; myelodysplastic syndrome; quality of life; transfusion.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

Similar articles
-
Association of anemia with worsened activities of daily living and health-related quality of life scores derived from the Minimum Data Set in long-term care residents.Health Qual Life Outcomes. 2012 Oct 19;10:129. doi: 10.1186/1477-7525-10-129. Health Qual Life Outcomes. 2012. PMID: 23083314 Free PMC article.
-
Clinical benefits of epoetin alfa (Eprex) 10,000 units subcutaneously thrice weekly in Thai cancer patients with anemia receiving chemotherapy.J Med Assoc Thai. 2005 May;88(5):607-12. J Med Assoc Thai. 2005. PMID: 16149676 Clinical Trial.
-
Early lenalidomide treatment for low and intermediate-1 International Prognostic Scoring System risk myelodysplastic syndromes with del(5q) before transfusion dependence.Cancer Med. 2015 Dec;4(12):1789-97. doi: 10.1002/cam4.523. Epub 2015 Sep 17. Cancer Med. 2015. PMID: 26376955 Free PMC article.
-
Standard of care for cancer-related anemia: improving hemoglobin levels and quality of life.Oncology. 2005;68 Suppl 1:22-32. doi: 10.1159/000083130. Oncology. 2005. PMID: 15855813 Review.
-
Postoperative red blood cell transfusion strategy in frail anemic elderly with hip fracture. A randomized controlled trial.Dan Med J. 2016 Apr;63(4):B5221. Dan Med J. 2016. PMID: 27034188 Review.
Cited by
-
Psychometric properties and meaningful change thresholds for the QOL-E instrument in patients with myelodysplastic neoplasms.Front Oncol. 2025 Feb 7;15:1507854. doi: 10.3389/fonc.2025.1507854. eCollection 2025. Front Oncol. 2025. PMID: 39990686 Free PMC article.
-
Survival and quality of life in patients with lower risk myelodysplastic syndromes exposed to erythropoiesis-stimulating agents: an observational cohort study.Lancet Haematol. 2025 Feb;12(2):e128-e137. doi: 10.1016/S2352-3026(24)00350-8. Lancet Haematol. 2025. PMID: 39909656 Free PMC article.
References
-
- UpToDate . Clinical Manifestations, Diagnosis, and Classification of Myelodysplastic Syndromes (MDS) UpToDate Inc.; Waltham, MA, USA: 2023. [(accessed on 5 June 2023)]. Available online: https://www.uptodate.com.
-
- Mittelman M. The myelodysplastic syndromes. Isr. J. Med. Sci. 1990;26:468–478. - PubMed
-
- Malcovati L., Hellstrom-Lindberg E., Bowen D., Adès L., Cermak J., del Cañizo C., Della Porta M.G., Fenaux P., Gattermann N., Germing U., et al. Diagnosis and treatment of primary myelodysplastic syndromes in adults: Recommendations from the European LeukemiaNet. Blood. 2013;122:2943–2964. doi: 10.1182/blood-2013-03-492884. - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

