Comparison of the Severity of Zoster-Associated Pain and Incidence of Postherpetic Neuralgia in Patients with and without Pre-Existing Spinal Disorders at the Same Spinal Nerve Level: A Retrospective Multicenter Study
- PMID: 37763054
- PMCID: PMC10532827
- DOI: 10.3390/jpm13091286
Comparison of the Severity of Zoster-Associated Pain and Incidence of Postherpetic Neuralgia in Patients with and without Pre-Existing Spinal Disorders at the Same Spinal Nerve Level: A Retrospective Multicenter Study
Abstract
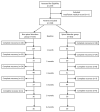
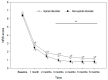
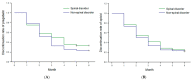
The incidences of herpes zoster (HZ) and postherpetic neuralgia (PHN) are significantly influenced by age. As individuals age, the occurrence of spinal disorders increases, thereby raising the likelihood of HZ and PHN coexistence. Considering this, our study aimed to explore the potential impact of pre-existing spinal disorders at the nerve level where HZ developed, on the severity of zoster-associated pain (ZAP) and the incidence of PHN. For our investigation, we retrospectively analyzed a total of 237 patients who presented with HZ and ZAP at various sensory levels (cervical, thoracic, lumbar, and sacral) with or without pre-existing spinal disorders. The presence or absence of spinal disorders at the sensory level affected by HZ was determined using computed tomography or magnetic resonance imaging. Our study results revealed that the group with spinal disorders at the sensory level where HZ developed did not exhibit an increased incidence of PHN. However, 3-6 months after HZ onset, this same group showed significantly higher ZAP scores compared to the group without spinal disorders. It implies a need for heightened pain management, as the coexistence of these conditions can increase pain severity. This study furnishes an initial standpoint to delve into intricate interactions between two diseases.
Keywords: herpes zoster; postherpetic neuralgia; spinal disease; varicella-zoster virus infection.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
References
-
- Xing X.-F., Zhen-Feng Z., Feng-Jiang Z., Yan M. The effect of early use of supplemental therapy on preventing postherpetic neuralgia: A systematic review and meta-analysis. Pain Physician. 2017;20:471. - PubMed
LinkOut - more resources
Full Text Sources
Research Materials

