Reattribution to Mind-Brain Processes and Recovery From Chronic Back Pain: A Secondary Analysis of a Randomized Clinical Trial
- PMID: 37768666
- PMCID: PMC10539987
- DOI: 10.1001/jamanetworkopen.2023.33846
Reattribution to Mind-Brain Processes and Recovery From Chronic Back Pain: A Secondary Analysis of a Randomized Clinical Trial
Abstract
Importance: In primary chronic back pain (CBP), the belief that pain indicates tissue damage is both inaccurate and unhelpful. Reattributing pain to mind or brain processes may support recovery.
Objectives: To test whether the reattribution of pain to mind or brain processes was associated with pain relief in pain reprocessing therapy (PRT) and to validate natural language-based tools for measuring patients' symptom attributions.
Design, setting, and participants: This secondary analysis of clinical trial data analyzed natural language data from patients with primary CBP randomized to PRT, placebo injection control, or usual care control groups and treated in a US university research setting. Eligible participants were adults aged 21 to 70 years with CBP recruited from the community. Enrollment extended from 2017 to 2018, with the current analyses conducted from 2020 to 2022.
Interventions: PRT included cognitive, behavioral, and somatic techniques to support reattributing pain to nondangerous, reversible mind or brain causes. Subcutaneous placebo injection and usual care were hypothesized not to affect pain attributions.
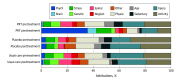
Main outcomes and measures: At pretreatment and posttreatment, participants listed their top 3 perceived causes of pain in their own words (eg, football injury, bad posture, stress); pain intensity was measured as last-week average pain (0 to 10 rating, with 0 indicating no pain and 10 indicating greatest pain). The number of attributions categorized by masked coders as reflecting mind or brain processes were summed to yield mind-brain attribution scores (range, 0-3). An automated scoring algorithm was developed and benchmarked against human coder-derived scores. A data-driven natural language processing (NLP) algorithm identified the dimensional structure of pain attributions.
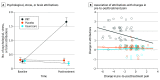
Results: We enrolled 151 adults (81 female [54%], 134 White [89%], mean [SD] age, 41.1 [15.6] years) reporting moderate severity CBP (mean [SD] intensity, 4.10 [1.26]; mean [SD] duration, 10.0 [8.9] years). At pretreatment, 41 attributions (10%) were categorized as mind- or brain-related across intervention conditions. PRT led to significant increases in mind- or brain-related attributions, with 71 posttreatment attributions (51%) in the PRT condition categorized as mind- or brain-related, as compared with 22 (8%) in control conditions (mind-brain attribution scores: PRT vs placebo, g = 1.95 [95% CI, 1.45-2.47]; PRT vs usual care, g = 2.06 [95% CI, 1.57-2.60]). Consistent with hypothesized PRT mechanisms, increases in mind-brain attribution score were associated with reductions in pain intensity at posttreatment (standardized β = -0.25; t127 = -2.06; P = .04) and mediated the effects of PRT vs control on 1-year follow-up pain intensity (β = -0.35 [95% CI, -0.07 to -0.63]; P = .05). The automated word-counting algorithm and human coder-derived scores achieved moderate and substantial agreement at pretreatment and posttreatment (Cohen κ = 0.42 and 0.68, respectively). The data-driven NLP algorithm identified a principal dimension of mind and brain vs biomechanical attributions, converging with hypothesis-driven analyses.
Conclusions and relevance: In this secondary analysis of a randomized trial, PRT increased attribution of primary CBP to mind- or brain-related causes. Increased mind-brain attribution was associated with reductions in pain intensity.
Conflict of interest statement
Figures

References
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials

