Posterior reversible encephalopathy syndrome (PRES) associated with SARS-CoV-2 infection in a patient under maintenance haemodialysis: a case report
- PMID: 37773103
- PMCID: PMC10542676
- DOI: 10.1186/s12882-023-03319-7
Posterior reversible encephalopathy syndrome (PRES) associated with SARS-CoV-2 infection in a patient under maintenance haemodialysis: a case report
Abstract
Background: Endothelial dysfunction is common in patients undergoing chronic haemodialysis, and is a major cause of posterior reversible encephalopathy syndrome (PRES). Recently, Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) has been shown to cause endothelial dysfunction by infecting vascular endothelial cells. Several cases of neurological complications in patients without kidney dysfunction, and only a few cases in patients with chronic kidney disease, have been reported in the literature. However, no previous report has yet described PRES associated with SARS-CoV-2 infection among patients undergoing maintenance dialysis.
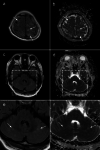
Case presentation: A 54-year-old woman undergoing maintenance haemodialysis was admitted to our hospital for status epilepticus. She had developed end-stage kidney disease (ESKD) secondary to diabetic nephropathy. Seven days prior to admission, she had developed fever and was diagnosed with COVID-19. Subsequently her blood pressure increased from 160/90 mmHg to 190/100 mmHg. On admission, she presented with severe hypertension (> 220/150 mmHg), unconsciousness, and epilepticus. CT tomography revealed no signs of brain haemorrhage. Cranio-spinal fluid (CSF) examination revealed no signs of encephalitis, and CSF polymerase chain reaction (PCR) for SARS-CoV-2 was negative. MRI findings revealed focal T2/FLAIR hyperintensity in the bilateral parietooccipital regions, leading to the diagnosis of PRES. Deep sedation and strict blood pressure control resulted in a rapid improvement of her symptoms, and she was discharged without sequelae.
Conclusions: We report the first case of PRES associated with SARS-CoV-2 infection in a patient undergoing maintenance haemodialysis. Patients undergoing maintenance haemodialysis are at high risk of PRES because of several risk factors. SARS-CoV-2 infection causes direct invasion of endothelial cells by binding to angiotensin-converting enzyme 2 (ACE2), initiating cytokine release, and hypercoagulation, leading to vascular endothelial cell injury and increased vascular leakage. In the present case, SARS-CoV-2 infection possibly be associated with the development of PRES.
Keywords: End-stage kidney disease; Haemodialysis; Intravascular endothelial cell injury; Posterior reversible encephalopathy syndrome; Status epilepticus.
© 2023. BioMed Central Ltd., part of Springer Nature.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures


Similar articles
-
Posterior reversible encephalopathy syndrome during convalescence from COVID-19.Int J Neurosci. 2023 Jun;133(6):672-675. doi: 10.1080/00207454.2021.1966629. Epub 2021 Aug 19. Int J Neurosci. 2023. PMID: 34370958
-
SARS-CoV-2 may play a direct role in the pathogenesis of posterior reversible encephalopathy syndrome (PRES) associated with COVID-19: A CARE-compliant case report and literature review.Medicine (Baltimore). 2024 Feb 2;103(5):e37192. doi: 10.1097/MD.0000000000037192. Medicine (Baltimore). 2024. PMID: 38306528 Free PMC article. Review.
-
Posterior reversible encephalopathy syndrome - A pathology that should not be overlooked in the era of COVID-19.Am J Emerg Med. 2022 Jun;56:393.e5-393.e8. doi: 10.1016/j.ajem.2022.03.005. Epub 2022 Mar 13. Am J Emerg Med. 2022. PMID: 35346531 Free PMC article.
-
Posterior reversible encephalopathy syndrome (PRES) associated with COVID-19.J Clin Neurosci. 2021 Jun;88:108-112. doi: 10.1016/j.jocn.2021.03.028. Epub 2021 Mar 23. J Clin Neurosci. 2021. PMID: 33992168 Free PMC article.
-
Posterior Reversible Encephalopathy Syndrome and brain haemorrhage as COVID-19 complication: a review of the available literature.J Neurol. 2021 Dec;268(12):4407-4414. doi: 10.1007/s00415-021-10709-0. Epub 2021 Jul 21. J Neurol. 2021. PMID: 34291313 Free PMC article. Review.
Cited by
-
A case of bilateral cortical blindness followed by generalised tonic-clonic seizure epilepsy in a patient with posterior reversible encephalopathy syndrome.Heliyon. 2024 Sep 7;10(18):e37642. doi: 10.1016/j.heliyon.2024.e37642. eCollection 2024 Sep 30. Heliyon. 2024. PMID: 39309783 Free PMC article.
References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

