Moderate-to-severe lower respiratory tract infection in early life is associated with increased risk of polysensitization and atopic dermatitis: Findings from the CHILD Study
- PMID: 37780586
- PMCID: PMC10509933
- DOI: 10.1016/j.jacig.2021.12.005
Moderate-to-severe lower respiratory tract infection in early life is associated with increased risk of polysensitization and atopic dermatitis: Findings from the CHILD Study
Abstract
Background: Respiratory infections in infancy are associated with the development of allergic asthma and atopy. Delineating whether symptomatic infections are a marker of atopic predisposition or contribute to atopic development is important for preventive strategies. We hypothesized that early, severe lower respiratory tract infections (LRTIs) may be a risk factor for the development of atopic disease.
Objective: Our aim was to determine whether clinically defined, moderate-to-severe LRTIs in infancy are associated with the development of atopic dermatitis and allergic sensitization at preschool age.
Methods: LRTI timing and severity in the first 18 months of life was defined by using the Canadian Healthy Infant Longitudinal Development study questionnaires. Polysensitization and atopic dermatitis were determined by standardized skin prick testing and structured clinical assessments. Longitudinal associations between LRTI severity and clinical outcomes at ages 3 years and 5 years were determined by adjusted repeated measures generalized estimation equations.
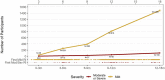
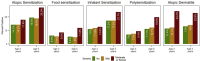
Results: Moderate-to-severe LRTIs were associated with increased odds of polysensitization (odds ratio = 1.91 [95% CI = 1.16-3.15]; P = .014) and atopic dermatitis (odds ratio = 2.19 [95% CI 1.41-3.39]; P < .001) as compared with the odds in children with no history of LRTI in the first 18 months of life. The association between moderate-to-severe LRTI and polysensitization or atopic dermatitis remained robust after adjusting for sex; study site; breast-feeding duration; and mother, father, or both-parent atopy or asthma.
Conclusions: These results highlight severe infant LRTI as an important risk factor for allergic and atopic disease (ie, polysensitization and atopic dermatitis), and they suggest that this risk is independent of maternal in utero environment, both-parent history of asthma, and both-parent genetic predisposition.
Keywords: Respiratory infection; allergy; atopic dermatitis; atopy; food allergy; pediatrics.
Crown Copyright © 2022 Published by Elsevier Inc. on behalf of the American Academy of Allergy, Asthma & Immunology.
Figures
Similar articles
-
Predicting the atopic march: Results from the Canadian Healthy Infant Longitudinal Development Study.J Allergy Clin Immunol. 2018 Feb;141(2):601-607.e8. doi: 10.1016/j.jaci.2017.08.024. Epub 2017 Nov 15. J Allergy Clin Immunol. 2018. PMID: 29153857 Clinical Trial.
-
Early life environmental exposure in relation to new onset and remission of allergic diseases in school children: Polish Mother and Child Cohort Study.Allergy Asthma Proc. 2019 Sep 1;40(5):329-337. doi: 10.2500/aap.2019.40.4237. Allergy Asthma Proc. 2019. PMID: 31514791
-
Development of allergies and asthma in infants and young children with atopic dermatitis--a prospective follow-up to 7 years of age.Allergy. 2000 Mar;55(3):240-5. doi: 10.1034/j.1398-9995.2000.00391.x. Allergy. 2000. PMID: 10753014
-
Prevention of allergic disease in childhood: clinical and epidemiological aspects of primary and secondary allergy prevention.Pediatr Allergy Immunol. 2004 Jun;15 Suppl 16:4-5, 9-32. doi: 10.1111/j.1399-3038.2004.0148b.x. Pediatr Allergy Immunol. 2004. PMID: 15125698 Review.
-
Complementary feeding and food allergy, atopic dermatitis/eczema, asthma, and allergic rhinitis: a systematic review.Am J Clin Nutr. 2019 Mar 1;109(Suppl_7):890S-934S. doi: 10.1093/ajcn/nqy220. Am J Clin Nutr. 2019. PMID: 30982864
Cited by
-
Respiratory Syncytial Virus-Specific Antibodies and Atopic Diseases in Children: A 10-Year Follow-Up.Pathogens. 2023 Apr 1;12(4):546. doi: 10.3390/pathogens12040546. Pathogens. 2023. PMID: 37111432 Free PMC article.
-
Progressive accumulation of hyperinflammatory NKG2Dlow NK cells in early childhood severe atopic dermatitis.Sci Immunol. 2024 Sep 2;9(92):eadd3085. doi: 10.1126/sciimmunol.add3085. Epub 2024 Feb 9. Sci Immunol. 2024. PMID: 38335270 Free PMC article.
-
From Fetus to Eight: the CHILD Cohort Study.Am J Epidemiol. 2024 Oct 11;194(7):1984-98. doi: 10.1093/aje/kwae397. Online ahead of print. Am J Epidemiol. 2024. PMID: 39393830 Free PMC article.
-
Prevalence and risk factors for allergic sensitization: 3 cross-sectional studies among schoolchildren from 1996 to 2017.J Allergy Clin Immunol Glob. 2023 Jul 19;2(4):100150. doi: 10.1016/j.jacig.2023.100150. eCollection 2023 Nov. J Allergy Clin Immunol Glob. 2023. PMID: 37781648 Free PMC article.
-
Exploring the potential mediating role of systemic antibiotics in the association between early-life lower respiratory tract infections and asthma at age 5 in the CHILD study.Front Allergy. 2025 Jan 21;5:1463867. doi: 10.3389/falgy.2024.1463867. eCollection 2024. Front Allergy. 2025. PMID: 39906720 Free PMC article.
References
-
- Henderson J., Hilliard T.N., Sherriff A., Stalker D., Al Shammari N., Thomas H.M. Hospitalization for RSV bronchiolitis before 12 months of age and subsequent asthma, atopy and wheeze: a longitudinal birth cohort study. Pediatr Allergy Immunol. 2005;16:386–392. - PubMed
LinkOut - more resources
Full Text Sources

