Cardiac magnetic resonance as a risk re-stratification tool in apical hypertrophic cardiomyopathy
- PMID: 37780950
- PMCID: PMC10538924
- DOI: 10.47487/apcyccv.v4i2.289
Cardiac magnetic resonance as a risk re-stratification tool in apical hypertrophic cardiomyopathy
Abstract
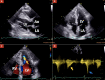
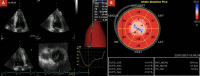
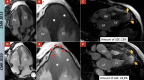
Apical hypertrophic cardiomyopathy (ApHCM) can result in the formation of a left ventricular apical aneurysm and progressive myocardial fibrosis, which is associated with a worse prognosis. We present the case of a 76-year-old man previously diagnosed with ApHCM seven years ago, who has been under clinical follow-up. Serial cardiac magnetic resonance (CMR) imaging was performed in 2013 and 2020 due to suspected apical aneurysm formation based on echocardiographic evaluation. The 2020 CMR imaging revealed an increase in myocardial fibrosis observed through late-gadolinium enhancement images and, for the first time, a small apical aneurysm that was not clearly visualized on two-dimensional echocardiography. The time course leading to the development of an ApHCM aneurysm is not well-defined and may impact the clinical course.
La miocardiopatía hipertrófica apical (MCHap) puede provocar la formación de un aneurisma apical del ventrículo izquierdo (LV) y una fibrosis miocárdica progresiva que se relaciona con un peor pronóstico. Se presenta el relato de un paciente de 76 años con diagnóstico previo de MCHap hace siete años en seguimiento clínico. Se realizó una resonancia magnética cardíaca (RMC) seriada en 2013 y 2020, ante la sospecha de formación de aneurisma apical mediante ecocardiografía. Las imágenes RMC del 2020 demostraron un aumento de la fibrosis miocárdica mediante imágenes de realce tardío con gadolinio y, por primera vez, un pequeño aneurisma apical que no fue definido en forma precisa en la ecocardiografía bidimensional. El tiempo de progresión hasta el desarrollo del aneurisma en la MCHap no está claramente definido y puede relacionarse con cambios en el curso clínico.
Keywords: Apical Hypertrophic Cardiomyopathy; Cardiac Aneurysm; Cardiac Magnetic Resonance; Echocardiography.
Conflict of interest statement
Conflicts of interest: The authors declare that they have no conflicts of interest
Figures

References
-
- Elliott PM, Anastasakis A, Borger MA, Borggrefe M, Cecchi F, Charron P, et al. 2014 ESC Guidelines on diagnosis and management of hypertrophic cardiomyopathy the Task Force for the Diagnosis and Management of Hypertrophic Cardiomyopathy of the European Society of Cardiology (ESC) Eur Heart J. 2014;35(39):2733–2779. doi: 10.1093/eurheartj/ehu284. - DOI - PubMed
Publication types
LinkOut - more resources
Full Text Sources
