Optimizing a Technology-Based Body and Mind Intervention to Prevent Falls and Reduce Health Disparities in Low-Income Populations: Protocol for a Clustered Randomized Controlled Trial
- PMID: 37788049
- PMCID: PMC10582821
- DOI: 10.2196/51899
Optimizing a Technology-Based Body and Mind Intervention to Prevent Falls and Reduce Health Disparities in Low-Income Populations: Protocol for a Clustered Randomized Controlled Trial
Abstract
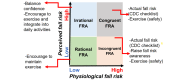
Background: The lack of health care coverage, low education, low motivation, and inconvenience remain barriers to participating in fall prevention programs, especially among low-income older adults. Low-income status also contributes to negative aging self-perceptions and is associated with a high perceived barrier to care. Existing fall prevention intervention technologies do not enable participants and practitioners to interact and collaborate, even with technologies that bring viable strategies to maintain independence, prevent disability, and increase access to quality care. Research is also limited on the use of technology to enhance motivation and help individuals align their perception with physiological fall risk. We developed a novel, 8-week Physio-Feedback Exercise Program (PEER), which includes (1) technology-based physio-feedback using a real-time portable innovative technology-the BTrackS Balance Tracking System, which is reliable and affordable, allows for home testing, and provides feedback and tracks balance progression; (2) cognitive reframing using the fall risk appraisal matrix; and (3) peer-led exercises focusing on balance, strength training, and incorporating exercises into daily activities.
Objective: This study consists of 3 aims. Aim 1 is to examine the effects of the technology-based PEER intervention on fall risk, dynamic balance, and accelerometer-based physical activity (PA). Aim 2 is to examine the effects of the PEER intervention on fall risk appraisal shifting and negative self-perceptions of aging. Aim 3 is to explore participants' experiences with the PEER intervention and potential barriers to accessing and adopting the technology-based PEER intervention to inform future research.
Methods: This is an intention-to-treat, single-blinded, parallel, 2-arm clustered randomized controlled trial study. We will collect data from 340 low-income older adults at baseline (T1) and measure outcomes after program completion (T2) and follow-up at 3 months (T3) and 6 months (T4). Participants will be enrolled if they meet all the following inclusion criteria: aged ≥60 years, cognitively intact, and able to stand without assistance. Exclusion criteria were as follows: a medical condition precluding exercise or PA, currently receiving treatment from a rehabilitation facility, plan to move within 1 year, hospitalized >3 times in the past 12 months, and does not speak English or Spanish.
Results: As of August 2023, the enrollment of participants is ongoing.
Conclusions: This study addresses the public health problem by optimizing a customized, technology-driven approach that can operate in low-resource environments with unlimited users to prevent falls and reduce health disparities in low-income older adults. The PEER is a novel intervention that combines concepts of physio-feedback, cognitive reframing, and peer-led exercise by motivating a shift in self-estimation of fall risk to align with physiological fall risk to improve balance, PA, and negative aging self-perception.
Trial registration: ClinicalTrials.gov NCT05778604; https://www.clinicaltrials.gov/ct2/show/study/NCT05778604.
International registered report identifier (irrid): DERR1-10.2196/51899.
Keywords: exercise; fall prevention; fear of falling; low income; older adults; technology.
©Ladda Thiamwong, Rui Xie, Joon-Hyuk Park, Nichole Lighthall, Victoria Loerzel, Jeffrey Stout. Originally published in JMIR Research Protocols (https://www.researchprotocols.org), 03.10.2023.
Conflict of interest statement
Conflicts of Interest: None declared.
Figures
Similar articles
-
Physio-Feedback and Exercise Program (PEER) Improves Balance, Muscle Strength, and Fall Risk in Older Adults.Res Gerontol Nurs. 2020 Nov 1;13(6):289-296. doi: 10.3928/19404921-20200324-01. Epub 2020 Apr 14. Res Gerontol Nurs. 2020. PMID: 32286669
-
Shifting Maladaptive Fall Risk Appraisal in Older Adults through an in-Home Physio-fEedback and Exercise pRogram (PEER): A Pilot Study.Clin Gerontol. 2020 Jul-Sep;43(4):378-390. doi: 10.1080/07317115.2019.1692120. Epub 2019 Nov 12. Clin Gerontol. 2020. PMID: 31713464
-
Pulmonary Rehabilitation With Balance Training for Fall Reduction in Chronic Obstructive Pulmonary Disease: Protocol for a Randomized Controlled Trial.JMIR Res Protoc. 2017 Nov 20;6(11):e228. doi: 10.2196/resprot.8178. JMIR Res Protoc. 2017. PMID: 29158206 Free PMC article.
-
The Effect of Mixed Reality Technologies for Falls Prevention Among Older Adults: Systematic Review and Meta-analysis.JMIR Aging. 2021 Jun 30;4(2):e27972. doi: 10.2196/27972. JMIR Aging. 2021. PMID: 34255643 Free PMC article. Review.
-
Smart health technologies used to support physical activity and nutritional intake in fall prevention among older adults: A scoping review.Exp Gerontol. 2023 Oct 1;181:112282. doi: 10.1016/j.exger.2023.112282. Epub 2023 Sep 8. Exp Gerontol. 2023. PMID: 37660762
Cited by
-
Application of Levi's Muscle Index in frailty assessment: comparison of bioimpedance measures among older adults.Front Med (Lausanne). 2025 Jun 26;12:1525569. doi: 10.3389/fmed.2025.1525569. eCollection 2025. Front Med (Lausanne). 2025. PMID: 40641985 Free PMC article.
-
Mechanism-Driven Strategies for Reducing Fall Risk in the Elderly: A Multidisciplinary Review of Exercise Interventions.Healthcare (Basel). 2024 Nov 29;12(23):2394. doi: 10.3390/healthcare12232394. Healthcare (Basel). 2024. PMID: 39685016 Free PMC article. Review.
-
Multimodal Factors Affect Longitudinal Changes in Dynamic Balance in Community-Dwelling Older Adults.Clin Interv Aging. 2025 Mar 20;20:335-348. doi: 10.2147/CIA.S495112. eCollection 2025. Clin Interv Aging. 2025. PMID: 40129901 Free PMC article.
-
Recreating Fall Risk Appraisal matrix using R to support fall prevention programs.JAMIA Open. 2024 Sep 18;7(3):ooae088. doi: 10.1093/jamiaopen/ooae088. eCollection 2024 Oct. JAMIA Open. 2024. PMID: 39297152 Free PMC article.
-
Comparing Sleep Quality, Duration, and Efficiency Among Low-Income Community-Dwelling Older Adults With and Without Physical Disabilities.J Gerontol Nurs. 2024 Jul;50(7):12-18. doi: 10.3928/00989134-20240618-03. Epub 2024 Jul 1. J Gerontol Nurs. 2024. PMID: 38959511 Free PMC article.
References
-
- Poverty grew in 2020 as Americans lost income and health insurance. USA Facts. 2021. Sep 23, [2020-01-10]. https://usafacts.org/articles/poverty-grew-in-2020-as-americans-lost-inc... .
-
- STEDI-older adult fall prevention. Centers for Disease Control and Prevention. 2017. Nov 29, [2021-11-15]. https://www.cdc.gov/steadi/
-
- Wehner-Hewson N, Watts P, Buscombe R, Bourne N, Hewson D. Racial and ethnic differences in falls among older adults: a systematic review and meta-analysis. J Racial Ethn Health Disparities. 2022 Dec 16;9(6):2427–40. doi: 10.1007/s40615-021-01179-1. https://europepmc.org/abstract/MED/34786654 10.1007/s40615-021-01179-1 - DOI - PMC - PubMed
-
- Silva AD, Faleiros HH, Shimizu WA, Nogueira Lde M, Nhãn LL, Silva BA, Otuyama PM. [The prevalence of falls and associated factors among the elderly according to ethnicity] Cien Saude Colet. 2012 Aug;17(8):2181–90. doi: 10.1590/s1413-81232012000800028. https://www.scielo.br/scielo.php?script=sci_arttext&pid=S1413-8123201200... S1413-81232012000800028 - DOI - PubMed
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous