Skull Base Collision Tumors: Giant Non-functioning Pituitary Adenoma and Olfactory Groove Meningioma
- PMID: 37809125
- PMCID: PMC10552590
- DOI: 10.7759/cureus.44710
Skull Base Collision Tumors: Giant Non-functioning Pituitary Adenoma and Olfactory Groove Meningioma
Abstract
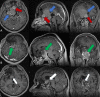
A collision tumor complex is composed of at least two different tumors, benign or malignant, with at least two different histopathological features located adjacent to each other in the exact anatomical localization. Pathologies such as meningiomas, pituitary adenomas, gliomas, and schwannomas may be involved in a collision tumor complex. However, co-occurrence of pituitary adenomas and meningiomas as skull base collision tumors is rare. Here, we present a 65-year-old male patient who presented with olfactory groove meningioma and non-functioning pituitary adenoma as a collision tumor. The patient was admitted with a headache and right-sided vision loss. The patient's first neurologic examination was consistent with temporal anopsia in the right eye. Subsequent contrast-enhanced cranial MRI revealed a 65x55x40 mm heterogeneously contrast-enhanced lesion in the anterior skull base extending from the sellar region to the corpus callosum. Because of the tumor size, a two-staged operation was planned. First, the tumor was partially excised via a right frontal craniotomy with a transcranial approach, and the tumor in the sellar region was left as a residue. The pathology reports after the first surgery showed pituitary adenoma and meningeal epithelial type meningioma (WHO Grade I). The residual tumor tissue was resected seven months later via an endoscopic endonasal approach, except for the part that invaded the right anterior cerebral artery. The optic nerve was decompressed. The patient was then referred to the radiation oncology clinic for radiosurgery. Collision tumors should be considered in the differential diagnosis in preoperative evaluation and surgical planning when heterogeneously contrast-enhanced areas significantly localized adjacent to each other are seen on cranial MRI. On the other hand, when the surgeon encounters sudden changes in the appearance or consistency of the tumor during the surgery, they should suspect these tumor complexes. The diagnosis of collision tumors is quite challenging but is of great importance regarding the patient's need for postoperative radiation therapy or the recurrence characteristics of tumors. However, more studies are needed on these complexes' etiology, surgical planning, and postoperative management.
Keywords: collision tumor; nonfunctioning pituitary adenoma; olfactory groove meningoma; sella turcica; skull base collision tumors.
Copyright © 2023, Aydin et al.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures


References
-
- Collision tumors of the adrenal gland: demonstration and characterization at MR imaging. Schwartz LH, Macari M, Huvos AG, Panicek DM. Radiology. 1996;201:757–760. - PubMed
-
- Two primary tumours metastasizing to the liver in a collision phenomenon. Gravante G, Ong SL, Cameron IC, Richards C, Metcalfe MS, Dennison AR, Lloyd DM. ANZ J Surg. 2010;80:368–369. - PubMed
-
- Risk of second brain tumor after conservative surgery and radiotherapy for pituitary adenoma: update after an additional 10 years. Minniti G, Traish D, Ashley S, Gonsalves A, Brada M. J Clin Endocrinol Metab. 2005;90:800–804. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
