Laparoscopic Management of Blunt Pancreatic Trauma in Adults and Pediatric Patients: A Systematic Review
- PMID: 37810623
- PMCID: PMC10555496
- DOI: 10.1155/2023/9296570
Laparoscopic Management of Blunt Pancreatic Trauma in Adults and Pediatric Patients: A Systematic Review
Abstract
Background: Pancreatic trauma is an uncommon injury that occurs usually in a young population and is frequently overlooked and not readily appreciated on initial examination. Nowadays, the diagnosis and management of pancreatic trauma are still controversial, and there is no gold standard for the treatment. The aim of this study is to describe our experience in the management of blunt pancreatic trauma with a laparoscopic approach and review the literature on laparoscopic management of pancreatic trauma.
Methods: A systematic literature review was performed, and 40 cases were reported and analysed; 10 cases were excluded because the complete data were not retrievable. We also reported our experience with the case of an 18-year-old male diagnosed with a deep laceration of the pancreas between body and tail, involving the main pancreatic duct, and with a concomitant hematoma. The patient underwent exploratory laparoscopy with abdominal toilet, necrosectomy, and suture of main pancreatic duct; the total blood loss was less than 200 ml, and the total operative time was 180 minutes. The patient recovered uneventfully and was discharged on the 6th postoperative day.
Results: 30 patients with pancreatic trauma, 10 adults and 20 pediatrics (mean age 28.2 years and 10.5 years), underwent a total laparoscopic approach: 2 distal pancreatic-splenectomy, 22 spleen-preserving distal pancreatectomy, and 6 laparoscopic drainage. The mean operative time for the adult and pediatric populations was 160.6 and 214.5 minutes, the mean estimated blood loss was 400 ml and 75 ml, and the mean hospital stay was 14.9 and 9 days, respectively.
Conclusion: Laparoscopic management for pancreatic trauma can be considered feasible and safe when performed by an experienced laparoscopic pancreatic team, and in such a setting, it can be considered a viable alternative to open surgery, offering the well-known benefits of minimally invasive surgery.
Copyright © 2023 Barbara Catellani et al.
Conflict of interest statement
Authors have no competing interests to disclose.
Figures

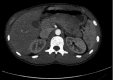
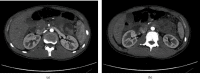
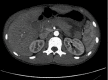
References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

