Advances in the design, generation, and application of tissue-engineered myocardial equivalents
- PMID: 37811368
- PMCID: PMC10559975
- DOI: 10.3389/fbioe.2023.1247572
Advances in the design, generation, and application of tissue-engineered myocardial equivalents
Abstract
Due to the limited regenerative ability of cardiomyocytes, the disabling irreversible condition of myocardial failure can only be treated with conservative and temporary therapeutic approaches, not able to repair the damage directly, or with organ transplantation. Among the regenerative strategies, intramyocardial cell injection or intravascular cell infusion should attenuate damage to the myocardium and reduce the risk of heart failure. However, these cell delivery-based therapies suffer from significant drawbacks and have a low success rate. Indeed, cardiac tissue engineering efforts are directed to repair, replace, and regenerate native myocardial tissue function. In a regenerative strategy, biomaterials and biomimetic stimuli play a key role in promoting cell adhesion, proliferation, differentiation, and neo-tissue formation. Thus, appropriate biochemical and biophysical cues should be combined with scaffolds emulating extracellular matrix in order to support cell growth and prompt favorable cardiac microenvironment and tissue regeneration. In this review, we provide an overview of recent developments that occurred in the biomimetic design and fabrication of cardiac scaffolds and patches. Furthermore, we sift in vitro and in situ strategies in several preclinical and clinical applications. Finally, we evaluate the possible use of bioengineered cardiac tissue equivalents as in vitro models for disease studies and drug tests.
Keywords: cardiac tissue engineering; cardiovascular diseases; disease modeling; myocardium; regenerative medicine.
Copyright © 2023 Bernava and Iop.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures


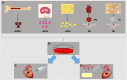

References
-
- Abbasi N., Hamlet S., Love R. M., Nguyen N. T. (2020). Porous scaffolds for bone regeneration. J. Sci. Adv. Mater Devices 5, 1–9. 10.1016/j.jsamd.2020.01.007 - DOI
Publication types
LinkOut - more resources
Full Text Sources

