Free Flap Failure and Complications in Acute Burns: A Systematic Review and Meta-analysis
- PMID: 37817922
- PMCID: PMC10561810
- DOI: 10.1097/GOX.0000000000005311
Free Flap Failure and Complications in Acute Burns: A Systematic Review and Meta-analysis
Abstract
Background: Severe acute burn injuries represent a challenge to the reconstructive surgeon. Free flap reconstruction might be required in cases of significant critical structure exposure and soft tissue deficits, when local options are unavailable. This study aimed to determine the free flap complication rate in acute burn patients.
Methods: A systematic review and meta-analysis were conducted and reported according to Preferred Reporting Items for Systematic Reviews and Meta-Analysis guidelines and registered on the International Prospective Register of Systematic Reviews database (CRD42023404478). The following databases were accessed: Embase, PubMed, Web of Science, and Cochrane Library. The primary outcome was the free flap failure rate.
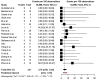
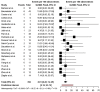
Results: The study identified 31 articles for inclusion. A total of 427 patients (83.3% men, 16.7% women) accounting for 454 free flaps were included. The mean patient age was 36.21 [95% confidence interval (CI), 31.25-41.16]. Total free flap loss rate was 9.91% [95% CI, 7.48%-13.02%], and partial flap loss was 4.76% [95% CI, 2.66%-8.39%]. The rate of venous thrombosis was 6.41% [95% CI, 3.90%-10.36%] and arterial thrombosis was 5.08% [95% CI, 3.09%-8.26%]. Acute return to the operating room occurred in 20.63% [16.33%-25.71%] of cases. Stratified by body region, free flaps in the lower extremity had a failure rate of 8.33% [95% CI, 4.39%-15.24%], whereas in the upper extremity, the failure rate was 6.74% [95% CI, 3.95%-11.25%].
Conclusion: This study highlights the high risk of free flap complications and failure in acute burn patients.
Copyright © 2023 The Authors. Published by Wolters Kluwer Health, Inc. on behalf of The American Society of Plastic Surgeons.
Conflict of interest statement
The authors have no financial interest to declare in relation to the content of this article. Disclosure statements are at the end of this article, following the correspondence information.
Figures









References
-
- Concannon E, Damkat-Thomas L, Rose E, et al. Use of a synthetic dermal matrix for reconstruction of 55 patients with nongraftable wounds and management of complications. J Burn Care Res. 2023;44:894–904. - PubMed
-
- Serror K, Boccara D, Chaouat M, et al. Dermal substitute: a safe and effective way in surgical management of adults post-burn dorsal foot contractures. Eur Rev Med Pharmacol Sci. 2023;27:29–36. - PubMed
LinkOut - more resources
Full Text Sources
