Contribution of the Medial Hamstrings to Valgus Stability of the Knee
- PMID: 37840900
- PMCID: PMC10571687
- DOI: 10.1177/23259671231202767
Contribution of the Medial Hamstrings to Valgus Stability of the Knee
Abstract
Background: Multiligament knee injuries involving the medial side are common. When performing surgical reconstruction, use of the medial hamstrings (HS) as grafts remains controversial in this setting.
Purpose: To determine the role of the medial HS in stabilizing the valgus knee for different types of medial-sided knee injury.
Study design: Controlled laboratory study.
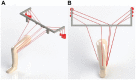
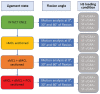
Methods: A biomechanical study on 10 cadaveric knees was performed. Valgus load (force moment of 10 N/m) was applied at 0°, 30°, and 60° of flexion, and the resultant rotation was recorded using an optoelectronic motion analysis system. Measurements were repeated for 4 different knee states: intact knee, superficial medial collateral ligament (sMCL) injury, deep medial collateral ligament (dMCL) injury, and posterior oblique ligament (POL) injury. For each state, 4 loading conditions (+ loaded; - unloaded) of the semitendinosus (ST) and gracilis (GRA) tendons were tested: ST+/GRA+, ST+/GRA-, ST-/GRA+, and ST-/GRA-.
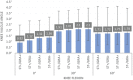
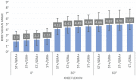
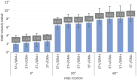
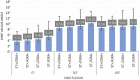
Results: At 0° of flexion, combined unloading of the ST and GRA (ST-/GRA-) increased valgus laxity on the intact knee compared with the ST+/GRA+ condition (P < .05). For all medial-sided injury states (isolated sMCL; combined sMCL and dMCL; and combined sMCL, dMCL, and POL damage), ST-/GRA- increased valgus laxity at 0° and 30° of flexion versus ST+/GRA+ (P < .05 for all). The absolute value of valgus laxity increased with the severity of medial-sided ligament injury. Isolated ST unloading increased valgus laxity for the intact knee and the MCL-injured knee (combined sMCL and dMCL) at 0° of flexion (P < .05 vs ST+/GRA+). Isolated unloading of the GRA had no effect on valgus knee stability.
Conclusion: The medial HS tendons contributed to the stabilization of the knee in valgus, and this was even more important when the medial side was severely affected (POL damage). This stabilizing effect was greater between 0° and 30°, in which the POL is the main valgus stabilizer.
Clinical relevance: When deciding on graft selection for multiligament knee injury reconstruction, the surgeon should be aware of the effect of harvesting the medial HS tendon on valgus laxity.
Keywords: MCL; POL; hamstring; knee; multiligament knee injury.
© The Author(s) 2023.
Conflict of interest statement
One or more of the authors has declared the following potential conflict of interest or source of funding: A.K. has received consulting fees from Stryker and speaking fees from Implantcast. R.P. has received consulting fees from Lepine. B.S.-C. has received consulting fees and royalties from Arthrex. T.N. has received consulting fees from Lepine. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto. Ethical approval was not sought for the present study.
Figures
Similar articles
-
Single-Strand "Short Isometric Construct" Medial Collateral Ligament Reconstruction Restores Valgus and Rotational Stability While Isolated Deep MCL and Superficial MCL Reconstruction Do Not.Am J Sports Med. 2024 Mar;52(4):968-976. doi: 10.1177/03635465231224477. Epub 2024 Feb 11. Am J Sports Med. 2024. PMID: 38343203
-
A Triple-Strand Anatomic Medial Collateral Ligament Reconstruction Restores Knee Stability More Completely Than a Double-Strand Reconstruction: A Biomechanical Study In Vitro.Am J Sports Med. 2022 Jun;50(7):1832-1842. doi: 10.1177/03635465221090612. Epub 2022 May 3. Am J Sports Med. 2022. PMID: 35503457 Free PMC article.
-
Medial Collateral Ligament Reconstruction for Anteromedial Instability of the Knee: A Biomechanical Study In Vitro.Am J Sports Med. 2022 Jun;50(7):1823-1831. doi: 10.1177/03635465221092118. Epub 2022 May 5. Am J Sports Med. 2022. PMID: 35511430 Free PMC article.
-
The Effect of Hamstring Tendon Autograft Harvest on the Restoration of Knee Stability in the Setting of Concurrent Anterior Cruciate Ligament and Medial Collateral Ligament Injuries.Am J Sports Med. 2018 Jan;46(1):163-170. doi: 10.1177/0363546517732743. Epub 2017 Oct 19. Am J Sports Med. 2018. PMID: 29048929
-
From Anatomy to Complex Reconstruction: A Modern Review on the Medial Collateral Ligament of the Knee.Arch Bone Jt Surg. 2022 Oct;10(10):818-826. doi: 10.22038/ABJS.2022.66697.3179. Arch Bone Jt Surg. 2022. PMID: 36452420 Free PMC article. Review.
Cited by
-
Effect of Graft Choice for ACL Reconstruction on Clinical Outcomes in Combined ACL and MCL Injuries: Comparison Between Bone-Patellar Tendon-Bone and Hamstring Autografts.J Clin Med. 2024 Oct 22;13(21):6316. doi: 10.3390/jcm13216316. J Clin Med. 2024. PMID: 39518456 Free PMC article.
-
Medial collateral ligament section during unicompartmental knee arthroplasty managed by direct repair and fascia lata augmentation autograft: a case report and surgical technique.AME Case Rep. 2024 Sep 10;8:108. doi: 10.21037/acr-24-30. eCollection 2024. AME Case Rep. 2024. PMID: 39380873 Free PMC article.
-
Current trends in the medial side of the knee: not only medial collateral ligament (MCL).J Orthop Traumatol. 2024 Dec 20;25(1):69. doi: 10.1186/s10195-024-00808-9. J Orthop Traumatol. 2024. PMID: 39704918 Free PMC article. Review.
-
Dynamic valgus after ACL reconstruction: quadriceps- vs. semitendinosus tendon grafts.Arch Orthop Trauma Surg. 2025 Jul 17;145(1):377. doi: 10.1007/s00402-025-05917-6. Arch Orthop Trauma Surg. 2025. PMID: 40676276
References
LinkOut - more resources
Full Text Sources

