Safety of dobutamine or adenosine stress cardiac magnetic resonance imaging in patients with left ventricular thrombus
- PMID: 37843560
- PMCID: PMC10881726
- DOI: 10.1007/s00392-023-02317-x
Safety of dobutamine or adenosine stress cardiac magnetic resonance imaging in patients with left ventricular thrombus
Abstract
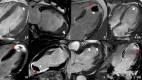
Background: Left ventricular (LV) thrombus formation is a common but potentially serious complication, typically occurring after myocardial infarction. Due to perceived high thromboembolic risk and lack of safety data, stress cardiac magnetic resonance (CMR) imaging especially with dobutamine is usually avoided despite its high diagnostic yield. This study aimed to investigate the characteristics, safety and outcome of patients with LV thrombus undergoing dobutamine or vasodilator stress CMR.
Methods: Patients undergoing stress CMR with concomitant LV thrombus were retrospectively included. Risk factors, comorbidities, and previous embolic events were recorded. Periprocedural safety was assessed for up to 48 h following the examination. Major adverse cardiac events (MACE) 12 months before the diagnosis were compared to 12 months after the exam and between patients and a matched control group. Additionally, patients were followed up for all-cause mortality.
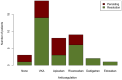
Results: 95 patients (78 male, 65 ± 10.7 years) were included. Among them, 43 patients underwent dobutamine (36 high-dose, 7 low-dose) and 52 vasodilator stress CMR. Periprocedural safety was excellent with no adverse events. During a period of 24 months, 27 MACE (14.7%) occurred in patients and controls with no statistical difference between groups. During a median follow-up of 33.7 months (IQR 37.6 months), 6 deaths (6.3%) occurred. Type of stress agent, thrombus mobility, or protrusion were not correlated to embolic events or death.
Conclusion: The addition of a stress test to a CMR exam is safe and does increase the generally high cardioembolic event rate in LV thrombus patients. Therefore, it is useful to support reperfusion decision-making.
Keywords: Adenosine; CMR; Cardiovascular imaging; Dobutamine; LV thrombus; Stroke.
© 2023. The Author(s).
Conflict of interest statement
The authors declare that they have no conflict of interests.
Figures

Similar articles
-
Left ventricular thrombus formation after acute myocardial infarction as assessed by cardiovascular magnetic resonance imaging.Eur J Radiol. 2012 Dec;81(12):3900-4. doi: 10.1016/j.ejrad.2012.06.029. Epub 2012 Sep 17. Eur J Radiol. 2012. PMID: 22995173 Clinical Trial.
-
Long-Term Embolic Outcomes After Detection of Left Ventricular Thrombus by Late Gadolinium Enhancement Cardiovascular Magnetic Resonance Imaging: A Matched Cohort Study.Circ Cardiovasc Imaging. 2019 Nov;12(11):e009723. doi: 10.1161/CIRCIMAGING.119.009723. Epub 2019 Nov 11. Circ Cardiovasc Imaging. 2019. PMID: 31707810 Free PMC article.
-
Detection of Left Ventricular Thrombus by Cardiac Magnetic Resonance in Embolic Stroke of Undetermined Source.Stroke. 2017 Sep;48(9):2434-2440. doi: 10.1161/STROKEAHA.117.018263. Epub 2017 Aug 17. Stroke. 2017. PMID: 28818863
-
Prognostic value of stress cardiac magnetic resonance imaging in patients with known or suspected coronary artery disease: a systematic review and meta-analysis.J Am Coll Cardiol. 2013 Aug 27;62(9):826-38. doi: 10.1016/j.jacc.2013.03.080. Epub 2013 May 30. J Am Coll Cardiol. 2013. PMID: 23727209 Free PMC article.
-
Cardiovascular magnetic resonance imaging for assessment of cardiac thrombus.Methodist Debakey Cardiovasc J. 2013 Jul-Sep;9(3):132-6. doi: 10.14797/mdcj-9-3-132. Methodist Debakey Cardiovasc J. 2013. PMID: 24066195 Free PMC article. Review.
References
-
- Bulluck H, Chan MHH, Paradies V, Yellon RL, Ho HH, Chan MY, et al. Incidence and predictors of left ventricular thrombus by cardiovascular magnetic resonance in acute ST-segment elevation myocardial infarction treated by primary percutaneous coronary intervention: a meta-analysis. J Cardiovasc Magnetic Resonance Off J Soc Cardiovasc Magnetic Resonance. 2018;20(1):72. doi: 10.1186/s12968-018-0494-3. - DOI - PMC - PubMed
-
- Keren A, Goldberg S, Gottlieb S, Klein J, Schuger C, Medina A, et al. Natural history of left ventricular thrombi: their appearance and resolution in the posthospitalization period of acute myocardial infarction. J Am Coll Cardiol. 1990;15(4):790–800. doi: 10.1016/0735-1097(90)90275-T. - DOI - PubMed
-
- Boivin-Proulx LA, Ieroncig F, Demers SP, Nozza A, Soltani M, Ghersi I, et al. Contemporary incidence and predictors of left ventricular thrombus in patients with anterior acute myocardial infarction. Clin Res Cardiol Off J German Cardiac Soc. 2023;112(4):558–565. - PubMed
-
- Hemetsberger R, Mankerious N, Toelg R, Abdelghani M, Farhan S, Garcia-Garica HM, et al. Patients with higher-atherothrombotic risk vs lower-atherothrombotic risk undergoing coronary intervention with newer-generation drug-eluting stents: an analysis from the randomized BIOFLOW trials. Clin Res Cardiol. 2023 doi: 10.1007/s00392-023-02205-4. - DOI - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

