Team-based continuity of care for patients with hypertension: a retrospective primary care cohort study in Hong Kong
- PMID: 37845086
- PMCID: PMC10587903
- DOI: 10.3399/BJGP.2023.0150
Team-based continuity of care for patients with hypertension: a retrospective primary care cohort study in Hong Kong
Abstract
Background: Continuity of care (COC) is associated with improved health outcomes in patients with hypertension. Team-based COC allows more flexibility in service delivery but there is a lack of research on its effectiveness for patients with hypertension.
Aim: To investigate the effectiveness of team-based COC on the prevention of cardiovascular disease (CVD) and mortality in patients with hypertension.
Design and setting: A retrospective cohort study in a primary care setting in Hong Kong.
Method: Eligible patients included those visiting public primary care clinics in Hong Kong from 2008 to 2018. The usual provider continuity index (UPCI) was used to measure the COC provided by the most visited physician team. Cox regression and restricted cubic splines were applied to model the association between the COC and the risk for CVDs and all-cause mortality.
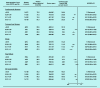
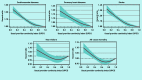
Results: This study included 421 640 eligible patients. Compared with participants in the lowest quartile of UPCI, the hazard ratios for overall CVD were 0.94 (95% CI = 0.92 to 0.96), 0.91(95% CI = 0.89 to 0.93), and 0.90 (95% CI = 0.88 to 0.92) in the second, third, and fourth quartiles, respectively. A greater effect size on CVD risk reduction was observed among the patients with unsatisfactory blood pressure control, patients aged <65 years, and those with a Charlson comorbidity index of <4 at baseline (Pinteraction<0.05 in these subgroup analyses), but the effect was insignificant among the participants with an estimated glomerular filtration rate of <60 ml/ min/1.73 m2 at baseline.
Conclusion: Team-based COC via a coordinated physician team was associated with reduced risks of CVD and all-cause mortality among patients with hypertension, especially for the patients with unsatisfactory blood pressure control. Early initiation of team-based COC may also achieve extra benefits.
Keywords: cardiovascular diseases; continuity of patient care; hypertension; primary health care.
© The Authors.
Conflict of interest statement
Eric Yuk Fai Wan has received research grants from the Food and Health Bureau of the Government of the Hong Kong SAR and the Hong Kong Research Grant Council, outside the submitted work. Esther Yee Tak Yu has received research grants from the Food and Health Bureau of the Government of the Hong Kong SAR, outside the submitted work. Cindy Lo Kuen Lam has received research grants from the Health Bureau of the Government of the Hong Kong SAR, the Hong Kong Research Grant Council, the Hong Kong College of Family Physicians, and Kerry Group Kuok Foundation outside the submitted work.
Figures


Comment in
-
Inequities in hypertension: we can do better ... but how?Br J Gen Pract. 2023 Oct 26;73(736):486-487. doi: 10.3399/bjgp23X735261. Print 2023 Nov. Br J Gen Pract. 2023. PMID: 37884376 Free PMC article. No abstract available.
References
-
- Khanam MA, Kitsos A, Stankovich J, et al. Association of continuity of care with blood pressure control in patients with chronic kidney disease and hypertension. Aust J Gen Pract. 2019;48(5):300–306. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous
