Noninvasive Bioelectronic Treatment of Postcesarean Pain: A Randomized Clinical Trial
- PMID: 37862016
- PMCID: PMC10589807
- DOI: 10.1001/jamanetworkopen.2023.38188
Noninvasive Bioelectronic Treatment of Postcesarean Pain: A Randomized Clinical Trial
Abstract
Importance: Improved strategies are needed to decrease opioid use after cesarean delivery but still adequately control postoperative pain. Although transcutaneous electrical stimulation devices have proven effective for pain control after other surgical procedures, they have not been tested as part of a multimodal analgesic protocol after cesarean delivery, the most common surgical procedure in the United States.
Objective: To determine whether treatment with a noninvasive high-frequency electrical stimulation device decreases opioid use and pain after cesarean delivery.
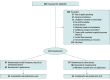
Design, setting, and participants: This triple-blind, sham-controlled randomized clinical trial was conducted from April 18, 2022, to January 31, 2023, in the labor and delivery unit at a single tertiary academic medical center in Ohio. Individuals were eligible for the study if they had a singleton or twin gestation and underwent a cesarean delivery. Of 267 people eligible for the study, 134 (50%) were included.
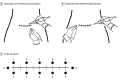
Intervention: Participants were randomly assigned in a 1:1 ratio to a high-frequency (20 000 Hz) electrical stimulation device group or to an identical-appearing sham device group and received 3 applications at the incision site in the first 20 to 30 hours postoperatively.
Main outcomes and measures: The primary outcome was inpatient postoperative opioid use, measured in morphine milligram equivalents (MME). Secondary outcomes included pain scores, measured with the Brief Pain Inventory questionnaire (scale, 0-10, with 0 representing no pain), MME prescribed at discharge, and receipt of additional opioid prescriptions in the postpartum period. Normally distributed data were assessed using t tests; otherwise via Mann-Whitney or χ2 tests as appropriate. Analyses were completed following intention-to-treat principles.
Results: Of 134 postpartum individuals who underwent a cesarean delivery (mean [SD] age, 30.5 [4.6] years; mean [SD] gestational age at delivery, 38 weeks 6 days [8 days]), 67 were randomly assigned to the functional device group and 67 to the sham device group. Most were multiparous, had prepregnancy body mass index (calculated as weight in kilograms divided by height in meters squared) higher than 30, were privately insured, and received spinal anesthesia. One participant in the sham device group withdrew consent prior to treatment. Individuals assigned to the functional device used significantly less opioid medication prior to discharge (median [IQR], 19.75 [0-52.50] MME) than patients in the sham device group (median [IQR], 37.50 [7.50-67.50] MME; P = .046) and reported similar rates of moderate to severe pain (85% vs 91%; relative risk [RR], 0.77 [95% CI, 0.55-1.29]; P = .43) and mean pain scores (3.59 [95% CI, 3.21-3.98] vs 4.46 [95% CI, 4.01-4.92]; P = .004). Participants in the functional device group were prescribed fewer MME at discharge (median [IQR], 82.50 [0-90.00] MME vs 90.00 [75.00-90.00] MME; P < .001). They were also more likely to be discharged without an opioid prescription (25% vs 10%; RR, 1.58 [95% CI, 1.08-2.13]; P = .03) compared with the sham device group. No treatment-related adverse events occurred in either group.
Conclusions and relevance: In this randomized clinical trial of postoperative patients following cesarean delivery, use of a high-frequency electrical stimulation device as part of a multimodal analgesia protocol decreased opioid use in the immediate postoperative period and opioids prescribed at discharge. These findings suggest that the use of this device may be a helpful adjunct to decrease opioid use without compromising pain control after cesarean delivery.
Conflict of interest statement
Figures
Similar articles
-
Opioid prescribing patterns among postpartum women.Am J Obstet Gynecol. 2018 Jul;219(1):103.e1-103.e8. doi: 10.1016/j.ajog.2018.04.003. Epub 2018 Apr 7. Am J Obstet Gynecol. 2018. PMID: 29630887 Free PMC article.
-
A personalized protocol for prescribing opioids after cesarean delivery: leveraging the electronic medical record to reduce outpatient opioid prescriptions.Am J Obstet Gynecol. 2024 Apr;230(4):446.e1-446.e6. doi: 10.1016/j.ajog.2023.09.092. Epub 2023 Sep 29. Am J Obstet Gynecol. 2024. PMID: 37778679
-
A comparison of acute pain management strategies after cesarean delivery.Am J Obstet Gynecol. 2022 Mar;226(3):407.e1-407.e7. doi: 10.1016/j.ajog.2021.09.003. Epub 2021 Sep 14. Am J Obstet Gynecol. 2022. PMID: 34534504
-
Perioperative gabapentin and post cesarean pain control: A systematic review and meta-analysis of randomized controlled trials.Eur J Obstet Gynecol Reprod Biol. 2019 Feb;233:98-106. doi: 10.1016/j.ejogrb.2018.11.026. Epub 2018 Dec 12. Eur J Obstet Gynecol Reprod Biol. 2019. PMID: 30583095
-
Comparing Three Ways to Help Patients with Acute Pain Learn about Opioid Risks — The Life STORRIED Study [Internet].Washington (DC): Patient-Centered Outcomes Research Institute (PCORI); 2021 Oct. Washington (DC): Patient-Centered Outcomes Research Institute (PCORI); 2021 Oct. PMID: 39383261 Free Books & Documents. Review.
References
-
- Agency for Healthcare Research and Quality. Overview of operating room procedures during inpatient stays in U.S. hospitals, 2018. Accessed September 25, 2023. https://hcup-us.ahrq.gov/reports/statbriefs/sb281-Operating-Room-Procedu... - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

