Atrial septal defect closure is associated with improved clinical status in patients ≤ 10 kg with bronchopulmonary dysplasia
- PMID: 37868716
- PMCID: PMC10588322
- DOI: 10.1002/pul2.12299
Atrial septal defect closure is associated with improved clinical status in patients ≤ 10 kg with bronchopulmonary dysplasia
Abstract
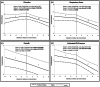
Patients with bronchopulmonary dysplasia (BPD) have shown clinical improvement after secundum atrial septal defect (ASD) closure. We sought to determine if this post-ASD closure improvement is secondary to the expected course in BPD patients or related to the closure itself. A novel BPD-ASD score was created to assess patients' clinical status (higher score = worse disease) and applied to 10 BPD-ASD inpatients weighing ≤ 10 kg who underwent ASD closure. The score and its subcomponents were retrospectively calculated serially ranging from 8 weeks pre- to 8 weeks post-intervention, and pre- and post-intervention score slopes were created. These slopes were compared using mixed regression modeling with an interaction term. There was a significant difference in pre- versus post-intervention slope with the most score drop the first week post-intervention (-2.1 + /- 0.8, p = 0.014). The mean score also dropped through weeks 2 (slope -0.8 + /- 0.8, p = 0.013) and 4 (slope -1.0 + /- 0.5, p = 0.001) post-intervention. There was a significant difference in pre- and post-intervention slopes for diuretics (p = 0.018) and the combined score of respiratory support, FiO2 need, and respiratory symptoms (p = 0.018). This study demonstrated significant improvement in BPD-ASD score, diuretic need, and respiratory status after ASD closure in BPD-ASD patients ≤ 10 kg that was outside of the natural course of BPD. Our study was limited by its small, single-center, retrospective nature. Future studies should be performed in a larger multicenter population to both validate the scoring system and compare to non-intervention infants.
Keywords: neonatal lung disease & BPD; pediatrics; pulmonary hypertension.
© 2023 The Authors. Pulmonary Circulation published by John Wiley & Sons Ltd on behalf of Pulmonary Vascular Research Institute.
Conflict of interest statement
Dr. Varghese receives royalties as an UptoDate reviewer; receives honoraria from Practice Point Communications as a speaker; receives research support from Janssen Pharmaceutical company; and receives an honoraria from the Pulmonary Hypertension Association for Professional development. Dr. Morris served on the scientific advisory board for Aytu Biopharma for a clinical trial for Vascular Ehlers‐Danlos syndrome until November 2022. Dr. Sexson Tejtel served on the Sobi scientific advisory board in 2022 and was provided a paid trip through the company regarding inflammatory heart conditions. The remaining authors declare no conflict of interest.
Figures


Similar articles
-
Successful Atrial Septal Defect Closure Subsequent to Medical Pulmonary Preconditioning in an Infant With Severe Pulmonary Hypertension Associated With Bronchopulmonary Dysplasia.Cureus. 2024 Mar 30;16(3):e57290. doi: 10.7759/cureus.57290. eCollection 2024 Mar. Cureus. 2024. PMID: 38690499 Free PMC article.
-
Early Surgical Closure of Atrial Septal Defect Improves Clinical Status of Symptomatic Young Children with Underlying Pulmonary Abnormalities.Pediatr Cardiol. 2020 Aug;41(6):1115-1124. doi: 10.1007/s00246-020-02361-8. Epub 2020 May 9. Pediatr Cardiol. 2020. PMID: 32388668 Free PMC article.
-
Association of Atrial Septal Defects and Bronchopulmonary Dysplasia in Premature Infants.J Pediatr. 2018 Nov;202:56-62.e2. doi: 10.1016/j.jpeds.2018.07.024. Epub 2018 Aug 29. J Pediatr. 2018. PMID: 30172431 Free PMC article.
-
Interventional Therapy Versus Medical Therapy for Secundum Atrial Septal Defect: A Systematic Review (Part 2) for the 2018 AHA/ACC Guideline for the Management of Adults With Congenital Heart Disease: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines.J Am Coll Cardiol. 2019 Apr 2;73(12):1579-1595. doi: 10.1016/j.jacc.2018.08.1032. Epub 2018 Aug 16. J Am Coll Cardiol. 2019. PMID: 30121241
-
Interventional Therapy Versus Medical Therapy for Secundum Atrial Septal Defect: A Systematic Review (Part 2) for the 2018 AHA/ACC Guideline for the Management of Adults With Congenital Heart Disease: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines.Circulation. 2019 Apr 2;139(14):e814-e830. doi: 10.1161/CIR.0000000000000605. Circulation. 2019. PMID: 30586769
Cited by
-
An interdisciplinary consensus approach to pulmonary hypertension in developmental lung disease.Eur Respir J. 2024 Sep 26;64(3):2400639. doi: 10.1183/13993003.00639-2024. Print 2024 Sep. Eur Respir J. 2024. PMID: 39147412 Free PMC article. Review.
-
Navigating Diagnostic and Treatment Challenges of Pulmonary Hypertension in Infants with Bronchopulmonary Dysplasia.J Clin Med. 2024 Jun 11;13(12):3417. doi: 10.3390/jcm13123417. J Clin Med. 2024. PMID: 38929946 Free PMC article. Review.
-
The pathogenesis of bronchopulmonary dysplasia: "It is never the heart, it is always the lung" - myth or maxim?Breathe (Sheff). 2025 Jul 15;21(3):240102. doi: 10.1183/20734735.0102-2024. eCollection 2025 Jul. Breathe (Sheff). 2025. PMID: 40673065 Free PMC article. Review.
-
Successful Atrial Septal Defect Closure Subsequent to Medical Pulmonary Preconditioning in an Infant With Severe Pulmonary Hypertension Associated With Bronchopulmonary Dysplasia.Cureus. 2024 Mar 30;16(3):e57290. doi: 10.7759/cureus.57290. eCollection 2024 Mar. Cureus. 2024. PMID: 38690499 Free PMC article.
References
-
- Lassus P, Turanlahti M, Heikkilä P, Andersson LC, Nupponen I, Sarnesto A, Andersson S. Pulmonary vascular endothelial growth factor and Flt‐1 in fetuses, in acute and chronic lung disease, and in persistent pulmonary hypertension of the newborn. Am J Respir Crit Care Med. 2001;164(10Pt1):1981–1987. - PubMed
-
- Kumar H. Growth factors in the fetal and neonatal lung. Front Biosci. 2004;9:464–480. - PubMed
-
- D'Angio T. The role of vascular growth factors in hyperoxia‐induced injury to the developing lung. Front Biosci. 2002;7:d1609–d1623. - PubMed
Associated data
LinkOut - more resources
Full Text Sources

