Dapagliflozin Improved Cardiac Function and Structure in Diabetic Patients with Preserved Ejection Fraction: Results of a Single Centre, Observational Prospective Study
- PMID: 37892836
- PMCID: PMC10607224
- DOI: 10.3390/jcm12206698
Dapagliflozin Improved Cardiac Function and Structure in Diabetic Patients with Preserved Ejection Fraction: Results of a Single Centre, Observational Prospective Study
Abstract
Sodium-glucose cotransporter inhibitors (SGLT2i) have demonstrated a reduction in cardiovascular events in diabetes and heart failure (HF). The mechanisms underlying this benefit are not well known and data are contradictory. The purpose of this study is to analyse the effect of dapagliflozin on cardiac structure and function in patients with normal ejection fraction. Between October 2020 and October 2021, we consecutively included 31 diabetic patients without prior history of SGLT2i use. In all of them, dapagliflozin treatment was started. At inclusion and during six months of follow-up, different clinical, ECG, analytical, and echocardiographic (standard, 3D, and speckle tracking) variables were recorded. After a follow-up period of 6.6 months, an average reduction of 18 g (p = 0.028) in 3D-estimated left ventricle mass was observed. An increase in absolute left ventricle global longitudinal strain (LV-GLS) of 0.3 (p = 0.036) was observed, as well as an increase in isovolumetric relaxation time (IVRT) of 10.5 ms (p = 0.05). Moreover, dapagliflozin decreased the levels of plasma creatin-kinase (CK-MB) and atrial natriuretic peptide (ANP). In conclusion, our data show that the use of SGLT2i is associated with both structural (myocardial mass) and functional (IVRT, LV-GLS) cardiac improvements in a population of diabetic patients with normal ejection fraction.
Keywords: biomarkers; dapagliflozin; echocardiography; sodium-glucose cotransporter type 2 inhibitors; speckle tracking.
Conflict of interest statement
The authors declare no conflict of interest.
Figures


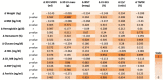
References
-
- Cavender M.A., Steg P.G., Smith S.C., Jr., Eagle K., Ohman E.M., Goto S., Kuder J., Im K., Wilson P.W.F., Bhatt D.L., et al. Impact of diabetes mellitus on hospitalization for heart failure, cardiovascular events, and death: Outcomes at 4 years from the Reduction of Atherothrombosis for Continued Health (REACH) Registry. Circulation. 2015;132:923–931. doi: 10.1161/CIRCULATIONAHA.114.014796. - DOI - PubMed
-
- Inzucchi S.E., Bergenstal R.M., Buse J.B., Diamant M., Ferrannini E., Nauck M., Peters A.L., Tsapas A., Wender R., Matthews D.R. Management of hyperglycemia in type 2 diabetes, 2015: A patient-centered approach: Update to a position statement of the American Diabetes Association and the European Association for the Study of Diabetes. Diabetes Care. 2015;38:140–149. doi: 10.2337/dc14-2441. - DOI - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

