Predictors of Nocturnal Hypoxemic Burden in Patients Undergoing Elective Coronary Artery Bypass Grafting Surgery
- PMID: 37893039
- PMCID: PMC10603934
- DOI: 10.3390/biomedicines11102665
Predictors of Nocturnal Hypoxemic Burden in Patients Undergoing Elective Coronary Artery Bypass Grafting Surgery
Abstract
Background: Nocturnal hypoxemia has been linked to increased cardiovascular morbidity and mortality. Several common diseases, such as sleep-disordered breathing (SDB), heart failure (HF), obesity, and pulmonary disease, coincide with an elevated nocturnal hypoxemic burden with and without repetitive desaturations. Research question: This study aimed to evaluate the association of relevant common diseases with distinctive metrics of nocturnal hypoxemic burden with and without repetitive desaturations in patients undergoing coronary artery bypass grafting surgery. Study design and methods: In this subanalysis of the prospective observational study, CONSIDER-AF (NCT02877745) portable SDB monitoring was performed on 429 patients with severe coronary artery disease the night before cardiac surgery. Pulse oximetry was used to determine nocturnal hypoxemic burden, as defined by total recording time spent with oxygen saturation levels < 90% (T90). T90 was further characterized as T90 due to intermittent hypoxemia (T90desaturation) and T90 due to nonspecific and noncyclic SpO2-drifts (T90non-specific). Results: Multivariable linear regression analysis identified SDB (apnea-hypopnea-index ≥ 15/h; B [95% CI]: 6.5 [0.4; 12.5], p = 0.036), obesity (8.2 [2.5; 13.9], p = 0.005), and mild-to-moderate chronic obstructive pulmonary disease (COPD, 16.7 [8.5; 25.0], p < 0.001) as significant predictors of an increased nocturnal hypoxemic burden. Diseases such as SDB, obesity and HF were significantly associated with elevated T90desaturation. In contrast, obesity and mild-to-moderate COPD were significant modulators of T90non-specific. Interpretation: SDB and leading causes for SDB, such as obesity and HF, are associated with an increased nocturnal hypoxemic burden with repetitive desaturations. Potential causes for hypoventilation syndromes, such as obesity and mild-to-moderate COPD, are linked to an increased hypoxemic burden without repetitive desaturations. Clinical Trial Registration: ClinicalTrials.gov identifier: NCT02877745.
Keywords: T90; heart failure; nocturnal hypoxemia; sleep apnea.
Conflict of interest statement
M.A. received consulting and lecture fees from ResMed, Philips Respironics, NRI, Bresotec, Boehringer-Ingelheim, Novartis, JAZZ Pharmaceuticals, and Bayer. All other authors have no conflict of interest to declare that are relevant to the content of this article.
Figures

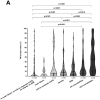


References
-
- Baumert M., A Immanuel S., Stone K.L., Harrison S.L., Redline S., Mariani S., Sanders P., McEvoy R.D., Linz D. Composition of nocturnal hypoxaemic burden and its prognostic value for cardiovascular mortality in older community-dwelling men. Eur. Heart J. 2020;41:533–541. doi: 10.1093/eurheartj/ehy838. - DOI - PMC - PubMed
-
- Azarbarzin A., A Sands S., Stone K.L., Taranto-Montemurro L., Messineo L., I Terrill P., Ancoli-Israel S., Ensrud K., Purcell S., White D.P., et al. The hypoxic burden of sleep apnoea predicts cardiovascular disease-related mortality: The Osteoporotic Fractures in Men Study and the Sleep Heart Health Study. Eur. Heart J. 2019;40:1149–1157. doi: 10.1093/eurheartj/ehy624. - DOI - PMC - PubMed
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

