International Variations in Surgical Morbidity and Mortality Post Gynaecological Oncology Surgery: A Global Gynaecological Oncology Surgical Outcomes Collaborative Led Study (GO SOAR1)
- PMID: 37894368
- PMCID: PMC10605858
- DOI: 10.3390/cancers15205001
International Variations in Surgical Morbidity and Mortality Post Gynaecological Oncology Surgery: A Global Gynaecological Oncology Surgical Outcomes Collaborative Led Study (GO SOAR1)
Abstract
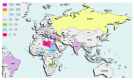
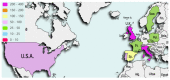
Gynaecological malignancies affect women in low and middle income countries (LMICs) at disproportionately higher rates compared with high income countries (HICs) with little known about variations in access, quality, and outcomes in global cancer care. Our study aims to evaluate international variation in post-operative morbidity and mortality following gynaecological oncology surgery between HIC and LMIC settings. Study design consisted of a multicentre, international prospective cohort study of women undergoing surgery for gynaecological malignancies (NCT04579861). Multilevel logistic regression determined relationships within three-level nested-models of patients within hospitals/countries. We enrolled 1820 patients from 73 hospitals in 27 countries. Minor morbidity (Clavien-Dindo I-II) was 26.5% (178/672) and 26.5% (267/1009), whilst major morbidity (Clavien-Dindo III-V) was 8.2% (55/672) and 7% (71/1009) for LMICs/HICs, respectively. Higher minor morbidity was associated with pre-operative mechanical bowel preparation (OR = 1.474, 95%CI = 1.054-2.061, p = 0.023), longer surgeries (OR = 1.253, 95%CI = 1.066-1.472, p = 0.006), greater blood loss (OR = 1.274, 95%CI = 1.081-1.502, p = 0.004). Higher major morbidity was associated with longer surgeries (OR = 1.37, 95%CI = 1.128-1.664, p = 0.002), greater blood loss (OR = 1.398, 95%CI = 1.175-1.664, p ≤ 0.001), and seniority of lead surgeon, with junior surgeons three times more likely to have a major complication (OR = 2.982, 95%CI = 1.509-5.894, p = 0.002). Of all surgeries, 50% versus 25% were performed by junior surgeons in LMICs/HICs, respectively. We conclude that LMICs and HICs were associated with similar post-operative major morbidity. Capacity to rescue patients from surgical complications is a tangible opportunity for meaningful intervention.
Keywords: collaborative research; gynaecological oncology; morbidity; mortality; surgery.
Conflict of interest statement
F.G. declares funding from The NHS Grampian Endowment Fund, British Gynaecological Cancer Society outside of this work and honorarium from AstraZeneca. All other authors declare no conflict of interest.
Figures
References
-
- Gaba F., Bizzarri N., Kamfwa P., Saiz A., Blyuss O., Paranjothy S., Ramirez P.T., Cibula D. Determining post-operative morbidity and mortality following gynecological oncology surgery: Protocol for a multicenter, international, prospective cohort study (Global Gynaecological Oncology Surgical Outcomes Collaborative-GO SOAR) Int. J. Gynecol. Cancer Off. J. Int. Gynecol. Cancer Soc. 2021;31:1287–1291. doi: 10.1136/ijgc-2021-002586. - DOI - PubMed
-
- Knight S.R., Shaw C.A., Pius R., Drake T.M., Norman L., Ademuyiwa A.O., Adisa A.O., Aguilera M.L., Al-Saqqa S.W., Al-Slaibi I., et al. Global variation in postoperative mortality and complications after cancer surgery: A multicentre, prospective cohort study in 82 countries. Lancet. 2021;397:387–397. doi: 10.1016/S0140-6736(21)00001-5. - DOI - PMC - PubMed
-
- ESGO ESGO Centre Accreditation For Gynaecological Oncology Training and Surgery. [(accessed on 30 August 2023)]. Available online: https://esgo.org/hospital-training-centre-accreditation/
Grants and funding
LinkOut - more resources
Full Text Sources