Predicting Maternal and Infant Tetrahydrocannabinol Exposure in Lactating Cannabis Users: A Physiologically Based Pharmacokinetic Modeling Approach
- PMID: 37896227
- PMCID: PMC10610403
- DOI: 10.3390/pharmaceutics15102467
Predicting Maternal and Infant Tetrahydrocannabinol Exposure in Lactating Cannabis Users: A Physiologically Based Pharmacokinetic Modeling Approach
Abstract
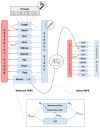
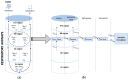
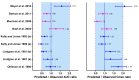
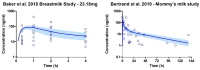
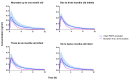
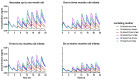
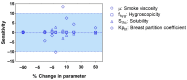
A knowledge gap exists in infant tetrahydrocannabinol (THC) data to guide breastfeeding recommendations for mothers who use cannabis. In the present study, a paired lactation and infant physiologically based pharmacokinetic (PBPK) model was developed and verified. The verified model was used to simulate one hundred virtual lactating mothers (mean age: 28 years, body weight: 78 kg) who smoked 0.32 g of cannabis containing 14.14% THC, either once or multiple times. The simulated breastfeeding conditions included one-hour post smoking and subsequently every three hours. The mean peak concentration (Cmax) and area under the concentration-time curve (AUC(0-24 h)) for breastmilk were higher than in plasma (Cmax: 155 vs. 69.9 ng/mL; AUC(0-24 h): 924.9 vs. 273.4 ng·hr/mL) with a milk-to-plasma AUC ratio of 3.3. The predicted relative infant dose ranged from 0.34% to 0.88% for infants consuming THC-containing breastmilk between birth and 12 months. However, the mother-to-infant plasma AUC(0-24 h) ratio increased up to three-fold (3.4-3.6) with increased maternal cannabis smoking up to six times. Our study demonstrated the successful development and application of a lactation and infant PBPK model for exploring THC exposure in infants, and the results can potentially inform breastfeeding recommendations.
Keywords: PBPK; THC in breastmilk; cannabinoids; cannabinoids in breastmilk; cannabis smoking; infant THC exposure; marijuana and breastfeeding; pediatric cannabis exposure; smoking and lactation; weed; weed and breastfeeding.
Conflict of interest statement
The authors declare no conflict of interest.
Figures





Similar articles
-
Cannabis use and measurement of cannabinoids in plasma and breast milk of breastfeeding mothers.Pediatr Res. 2021 Oct;90(4):861-868. doi: 10.1038/s41390-020-01332-2. Epub 2021 Jan 19. Pediatr Res. 2021. PMID: 33469174
-
Development and Verification of a Linked Δ 9-THC/11-OH-THC Physiologically Based Pharmacokinetic Model in Healthy, Nonpregnant Population and Extrapolation to Pregnant Women.Drug Metab Dispos. 2021 Jul;49(7):509-520. doi: 10.1124/dmd.120.000322. Epub 2021 May 5. Drug Metab Dispos. 2021. PMID: 33952608 Free PMC article.
-
Sertraline, citalopram and paroxetine in lactation: passage into breastmilk and infant exposure.Front Pharmacol. 2024 May 22;15:1414677. doi: 10.3389/fphar.2024.1414677. eCollection 2024. Front Pharmacol. 2024. PMID: 38841362 Free PMC article.
-
Is Breast Best? Examining the effects of alcohol and cannabis use during lactation.J Neonatal Perinatal Med. 2018;11(4):345-356. doi: 10.3233/NPM-17125. J Neonatal Perinatal Med. 2018. PMID: 29843260 Review.
-
[Tetrahydrocannabinol pharmacokinetics; new synthetic cannabinoids; road safety and cannabis].Bull Acad Natl Med. 2014 Mar;198(3):541-56; discussion 556-7. Bull Acad Natl Med. 2014. PMID: 26427296 Review. French.
Cited by
-
Pollutants in Breast Milk: A Scoping Review of the Most Recent Data in 2024.Healthcare (Basel). 2024 Mar 18;12(6):680. doi: 10.3390/healthcare12060680. Healthcare (Basel). 2024. PMID: 38540644 Free PMC article.
-
The Impact of Substance Use Disorder and Drug Transfer into Breast Milk: Implications for Maternal and Infant Health.Pharmaceutics. 2025 May 29;17(6):719. doi: 10.3390/pharmaceutics17060719. Pharmaceutics. 2025. PMID: 40574032 Free PMC article. Review.
-
Physiologically Based Pharmacokinetic Modeling of Cannabidiol, Delta-9-Tetrahydrocannabinol, and Their Metabolites in Healthy Adults After Administration by Multiple Routes.Clin Transl Sci. 2025 Jan;18(1):e70119. doi: 10.1111/cts.70119. Clin Transl Sci. 2025. PMID: 39748462 Free PMC article.
-
Physiologically based pharmacokinetic modeling of long-acting extended-release naltrexone in pregnant women with opioid use disorder.CPT Pharmacometrics Syst Pharmacol. 2024 Nov;13(11):1939-1952. doi: 10.1002/psp4.13252. Epub 2024 Oct 9. CPT Pharmacometrics Syst Pharmacol. 2024. PMID: 39380562 Free PMC article. Clinical Trial.
-
CBD and THC in Special Populations: Pharmacokinetics and Drug-Drug Interactions.Pharmaceutics. 2024 Apr 1;16(4):484. doi: 10.3390/pharmaceutics16040484. Pharmaceutics. 2024. PMID: 38675145 Free PMC article. Review.
References
-
- National Institute of Child Health and Human Development . Drugs and Lactation Database (LactMed®) National Institute of Child Health and Human Development; Bethesda MD, USA: 2006. Cannabis.
LinkOut - more resources
Full Text Sources
Miscellaneous

