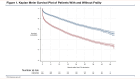
The Long-Term Impact of Frailty After an Intensive Care Unit Admission Due to Chronic Obstructive Pulmonary Disease
- PMID: 37931590
- PMCID: PMC10913924
- DOI: 10.15326/jcopdf.2023.0453
The Long-Term Impact of Frailty After an Intensive Care Unit Admission Due to Chronic Obstructive Pulmonary Disease
Abstract
Rationale: Frailty is an increasingly recognized aspect of chronic obstructive pulmonary disease (COPD). The impact of frailty on long-term survival after admission to an intensive care unit (ICU) due to an exacerbation of COPD has not been described.
Objective: The objective was to quantify the impact of frailty on time to death up to 4 years after admission to the ICU in Australia and New Zealand for an exacerbation of COPD.
Methods: We performed a multicenter retrospective cohort study of adult patients admitted to 179 ICUs with a primary diagnosis of an exacerbation of COPD using the Australian and New Zealand Intensive Care Society Adult Patient Database from January 1, 2018, through December 31, 2020, in New Zealand, and March 31, 2022, in Australia. Frailty was measured using the clinical frailty scale (CFS). The primary outcome was survival up to 4 years after ICU admission. The secondary outcome was readmission to the ICU due to an exacerbation of COPD.
Measurements and main results: We examined 7126 patients of which 3859 (54.1%) were frail (CFS scores of 5-8). Mortality in not-frail individuals versus frail individuals at 1 and 4 years was 19.8% versus 40.4%, and 56.8% versus 77.3% respectively (both p<0.001). Frailty was independently associated with a shorter time to death (adjusted hazard ratio 1.66; 95% confidence interval 1.54-1.80).There was no difference in the proportion of survivors with or without frailty who were readmitted to the ICU during a subsequent hospitalization.
Conclusions: Frailty was independently associated with poorer long-term survival in patients admitted to the ICU with an exacerbation of COPD.
Keywords: COPD; frailty; intensive care; mortality; readmission.
JCOPDF © 2024.
Conflict of interest statement
The authors have no conflicts of interest to declare.
References
-
- Fried LP,Tangen CM,Walston J,et al. Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci. 2001;56(3):M146-156. doi: https://doi.org/10.1093/gerona/56.3.M146 - PubMed
-
- Rockwood K,Song X,MacKnight C,et al. A global clinical measure of fitness and frailty in elderly people. CMAJ. 2005;173(5):489-495. doi: https://doi.org/10.1503/cmaj.050051 - PMC - PubMed
-
- Clegg A,Young J,Iliffe S,Rikkert MO,Rockwood K. Frailty in elderly people. Lancet. 2013;381(9868):752-762. doi: https://doi.org/10.1016/S0140-6736(12)62167-9 - PMC - PubMed
-
- Peng Y,Zhong GC,Zhou X,Guan L,Zhou L. Frailty and risks of all-cause and cause-specific death in community-dwelling adults: a systematic review and meta-analysis. BMC Geriatr. 2022;22(1):725. doi: https://doi.org/10.1186/s12877-022-03404-w - PMC - PubMed
-
- Aguayo GA,Donneau AF,Vaillant MT,et al. Agreement between 35 published frailty scores in the general population. Am J Epidemiol. 2017;186(4):420-434. doi: https://doi.org/10.1093/aje/kwx061 - PMC - PubMed
LinkOut - more resources
Full Text Sources