Factors Associated with Obstetric Violence Implicated in the Development of Postpartum Depression and Post-Traumatic Stress Disorder: A Systematic Review
- PMID: 37987409
- PMCID: PMC10661273
- DOI: 10.3390/nursrep13040130
Factors Associated with Obstetric Violence Implicated in the Development of Postpartum Depression and Post-Traumatic Stress Disorder: A Systematic Review
Abstract
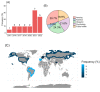
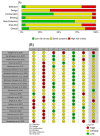
Postpartum depression (PPD) and post-traumatic stress disorder (PTSD) continue to be prevalent, and disabling women with mental disorders and obstetric violence (OV) may be a trigger for them, particularly during maternity. We aimed to analyze the association between manifestations of OV with the development of PPD and PTSD during pregnancy, childbirth, and postpartum. This systematic review was based on the PRISMA 2020 statement and explored original articles published between 2012 and 2022. A total of 21 articles were included in the analysis, and bias was assessed by the Effective Public Health Practice Project's Quality Assessment Tool. The highest rate of PPD symptoms appeared in women under 20 years old, multiparous, and with low education levels. The higher PTSD ratio was present in women under 35 years, primiparous, and with secondary studies. The mode of labor (instrumental or C-section) was identified as a major risk factor of PPD, being mediator variables of the informal coercion of health professionals and dissatisfaction with newborn healthcare. Instead, partner support during labor and high satisfaction with healthcare during birth were protective factors. Regarding PTSD, the mode of labor, several perineal tears, and the Kristeller technique were risk factors, and loss of autonomy and coercion modulated PTSD symptomatology. The protective factors for PTSD were respect for the labor plan, adequate communication with health professionals, social support during labor, and the skin-to-skin procedure. This systematic review provides evidence that OV contributes to PPD and PTSD, being important in developing standardized tools to prevent it. This study recommends changes in maternal healthcare policies, such as individualized healthcare assistance, humanized pregnancy protocols, and women's mental health follow-up, and improvements in the methodological quality of future research.
Keywords: maternal mental health; obstetric violence; obstetric vulnerability; post-traumatic stress disorder; postpartum depression; women’s health.
Conflict of interest statement
The authors declare no conflict of interest. The funders had no role in the design of the study; in the collection, analyses, or interpretation of data; in the writing of the manuscript; or in the decision to publish the results.
Figures

References
-
- World Health Organization (WHO) The Prevention and Elimination of Disrespect and Abuse during Facility-Based Childbirth: WHO Statement. [(accessed on 16 August 2023)]. Available online: https://www.who.int/publications/i/item/WHO-RHR-14.23.
-
- Corral-Manzano G.M. El Derecho Penal Como Medio de Prevención de La Violencia Obstétrica En México. Resultados al 2018. MUSAS. 2019;4:2. doi: 10.1344/musas2019.vol4.num2.6. - DOI
-
- Jojoa-Tobar E., Cuchumbe-Sánchez Y.D., Ledesma-Rengifo J.B., Muñoz-Mosquera M.C., Suarez-Bravo J.P. Violencia Obstétrica: Haciendo Visible Lo Invisible. Rev. Univ. Ind. Santander Salud. 2019;51:136–147. doi: 10.18273/revsal.v51n2-2019006. - DOI
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources

