Long-term health-related quality-of-life and psychosocial outcomes after uterus transplantation: a 5-year follow-up of donors and recipients
- PMID: 37995381
- PMCID: PMC10833084
- DOI: 10.1093/humrep/dead245
Long-term health-related quality-of-life and psychosocial outcomes after uterus transplantation: a 5-year follow-up of donors and recipients
Abstract
Study question: What are the outcomes regarding health-related quality-of-life, mood, and marital relationship of recipients and donors 5 years after uterus transplantation (UTx) and uterus donation?
Summary answer: Both recipients and donors generally demonstrated long-term stability regarding psychosocial outcomes but with negative deviations associated with unsuccessful outcomes.
What is known already: UTx is the first infertility treatment for women with absolute uterine factor infertility. The procedure can be performed with either a uterus donation from a live donor (LD), typically a close relative, or from a deceased, multi-organ donor. There are many potential stressful events over several years after UTx both for recipients and for LDs and these events may have impacts on quality-of-life and mental well-being.
Study design, size, duration: This, prospective observational cohort study includes the nine recipients and LDs of the first human UTx trial. They were assessed in 2017-2018 by questionnaires 5 years after UTx.
Participants/materials, setting, methods: The nine recipients (ages 32-43 years) and their respective LDs (ages 44-67 years) were either related (n = 8) or friends (n = 1). Eight recipients had congenital uterine absence and one was hysterectomized due to cervical cancer. For two recipients, UTx resulted in early graft failures, while six of the other seven recipients gave birth to a total of eight babies over the following 5 years. Physical and mental component summaries of health-related quality-of-life were measured with the SF-36 questionnaire. Mood was assessed by the Hospital Anxiety and Depression Scale. Relationship with partner was measured with the Dyadic Adjustment Scale. Comparisons were made between the values after 5 years and the values before uterus donation/transplantation.
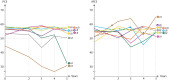
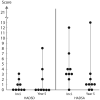
Main results and the role of chance: Five years after primary UTx, the majority of recipients scored above the predicted value of the general population on quality-of-life, except for two women, one of whom had a viable graft but no live birth and one recipient who was strained by quality-of-life changes, possibly related to parenthood transitions. Regarding mood, only one value (anxiety) was above the threshold for further clinical assessment. Recipients showed declining satisfaction with their marital relationships, but all reported scores above the 'at risk for divorce' threshold at the time of the final assessment in our study. The LDs were all found to be stable and above the predicted value of the general population regarding mental components of quality-of-life. Three LDs showed declined physical components, possibly related to older age. Only one LD reported a value in mood (anxiety) that would need further assessment. The marital satisfaction of LDs remained stable and unchanged compared to baseline values. Notably, the two recipients with early graft failures, and their related LDs, regained their mental well-being during the first years after graft failure and remained stable after 5 years.
Limitations, reasons for caution: The restricted sample size and the single-centre study-design are limitations of this study. Additionally the study was limited to LD UTx, as opposed to deceased donor UTx.
Wider implications of the findings: Our study shows that both LDs and recipients had acceptable or favourable quality-of-life outcomes, including mood assessment, at the 5-year follow-up mark, and that failure to achieve a live birth negatively affected these modalities both for LDs and recipients. Moreover, an important finding was that LDs and recipients are not reacting with depression after hysterectomy, which is common after hysterectomy in the general population.
Study funding/competing interest(s): Funding was provided by the Jane and Dan Olsson Foundation for Science, Knut and Alice Wallenberg Foundation, Handlanden Hjalmar Svensson Foundation, Swedish Governmental ALF Grant, and Swedish Research Council. There are no conflicts of interest to disclose.
Trial registration number: NCT01844362.
Keywords: infertility; psychology; quality-of-life; transplantation; uterus.
© The Author(s) 2023. Published by Oxford University Press on behalf of European Society of Human Reproduction and Embryology.
Conflict of interest statement
The authors of this manuscript have no conflicts of interest to disclose.
Figures


References
-
- Allyse M, Amer H, Coutifaris C, Falcone T, Famuyide A, Flyckt R, Gargiulo A, Heimbach J, Johannesson L, Jowsey-Gregoire S. et al. American Society for Reproductive Medicine position statement on uterus transplantation: a committee opinion. Fertil Steril 2018;110:605–610. - PubMed
-
- Bjelland I, Dahl AA, Haug TT, Neckelmann D.. The validity of the Hospital Anxiety and Depression Scale: an updated literature review. J Psychosom Res 2002;52:69–77. - PubMed
-
- Brännström M, Dahm-Kähler P, Kvarnström N, Enskog A, Olofsson JI, Olausson M, Mölne J, Akouri R, Järvholm S, Nilsson L. et al. Reproductive, obstetric, and long-term health outcome after uterus transplantation: results of the first clinical trial. Fertil Steril 2022;118:576–585. - PubMed
-
- Brännström M, Johannesson L, Bokström H, Kvarnström N, Mölne J, Dahm-Kähler P, Enskog A, Milenkovic M, Ekberg J, Diaz-Garcia C. et al. Livebirth after uterus transplantation. Lancet 2015;385:607–616. - PubMed
-
- Brännström M, Johannesson L, Dahm-Kähler P, Enskog A, Mölne J, Kvarnström N, Diaz-Garcia C, Hanafy A, Lundmark C, Marcickiewicz J. et al. First clinical uterus transplantation trial: a six-month report. Fertil Steril 2014;101:1228–1236. - PubMed
Publication types
MeSH terms
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

