Conduction System Pacing for Cardiac Resynchronization Therapy
- PMID: 37998506
- PMCID: PMC10672305
- DOI: 10.3390/jcdd10110448
Conduction System Pacing for Cardiac Resynchronization Therapy
Abstract
Cardiac resynchronization therapy (CRT) via biventricular pacing (BiVP-CRT) is considered a mainstay treatment for symptomatic heart failure patients with reduced ejection fraction and wide QRS. However, up to one-third of patients receiving BiVP-CRT are considered non-responders to the therapy. Multiple strategies have been proposed to maximize the percentage of CRT responders including two new physiological pacing modalities that have emerged in recent years: His bundle pacing (HBP) and left bundle branch area pacing (LBBAP). Both pacing techniques aim at restoring the normal electrical activation of the ventricles through the native conduction system in opposition to the cell-to-cell activation of conventional right ventricular myocardial pacing. Conduction system pacing (CSP), including both HBP and LBBAP, appears to be a promising pacing modality for delivering CRT and has proven to be safe and feasible in this particular setting. This article will review the current state of the art of CSP-based CRT, its limitations, and future directions.
Keywords: His bundle pacing; cardiac resynchronization therapy; conduction system pacing; left bundle branch pacing.
Conflict of interest statement
Cano has received consultant fees from Biotronik, Boston Scientific, Medtronic, and Microport. All other authors have nothing to disclose.
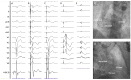
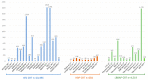
Figures
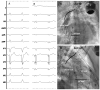
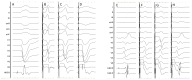
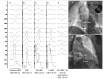
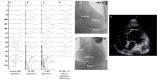
Similar articles
-
Is Conduction System Pacing Going to Be the New Gold Standard for Cardiac Resynchronization Therapy?J Clin Med. 2024 Jul 24;13(15):4320. doi: 10.3390/jcm13154320. J Clin Med. 2024. PMID: 39124587 Free PMC article. Review.
-
Conduction system pacing versus biventricular pacing in heart failure with reduced ejection fraction and electrical dyssynchrony.Front Cardiovasc Med. 2024 Dec 5;11:1495689. doi: 10.3389/fcvm.2024.1495689. eCollection 2024. Front Cardiovasc Med. 2024. PMID: 39703884 Free PMC article. Review.
-
Conduction System Pacing Versus Conventional Cardiac Resynchronization Therapy in Congenital Heart Disease.JACC Clin Electrophysiol. 2023 Mar;9(3):385-393. doi: 10.1016/j.jacep.2022.10.012. Epub 2022 Nov 30. JACC Clin Electrophysiol. 2023. PMID: 36752449
-
Left bundle branch pacing set to outshine biventricular pacing for cardiac resynchronization therapy?World J Cardiol. 2024 Apr 26;16(4):186-190. doi: 10.4330/wjc.v16.i4.186. World J Cardiol. 2024. PMID: 38690215 Free PMC article.
-
Sex Differences in Left Bundle Branch Area Pacing Versus Biventricular Pacing for Cardiac Resynchronization Therapy.JACC Clin Electrophysiol. 2024 Jul;10(7 Pt 2):1736-1749. doi: 10.1016/j.jacep.2024.05.011. Epub 2024 May 16. JACC Clin Electrophysiol. 2024. PMID: 38842969
Cited by
-
Left Bundle Branch Area Pacing to Overcome Coronary Sinus Anatomy-Related Technical Problems Encountered during Implantation of Biventricular CRT-A Case Report.J Clin Med. 2024 Jun 4;13(11):3307. doi: 10.3390/jcm13113307. J Clin Med. 2024. PMID: 38893018 Free PMC article.
-
Computational Medicine: What Electrophysiologists Should Know to Stay Ahead of the Curve.Curr Cardiol Rep. 2024 Dec;26(12):1393-1403. doi: 10.1007/s11886-024-02136-0. Epub 2024 Sep 20. Curr Cardiol Rep. 2024. PMID: 39302590 Review.
References
-
- Glikson M., Nielsen J.C., Kronborg M.B., Michowitz Y., Auricchio A., Barbash I.M., Barrabés J.A., Boriani G., Braunschweig F., Brignole M., et al. 2021 ESC Guidelines on cardiac pacing and cardiac resynchronization therapy. Eur. Heart J. 2021;42:3427–3520. doi: 10.1093/eurheartj/ehab364. Erratum in Eur. Heart J. 2022, 43, 1651. - DOI - PubMed
-
- Blanc J.J., Etienne Y., Gilard M., Mansourati J., Munier S., Boschat J., Benditt D.G., Lurie K.G. Evaluation of different ventricular pacing sites in patients with severe heart failure: Results of an acute hemodynamic study. Circulation. 1997;96:3273–3277. doi: 10.1161/01.CIR.96.10.3273. - DOI - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

