Association between the Preoperative Standard Uptake Value (SUV) and Survival Outcomes after Robotic-Assisted Segmentectomy for Resectable Non-Small Cell Lung Cancer (NSCLC)
- PMID: 38001639
- PMCID: PMC10670906
- DOI: 10.3390/cancers15225379
Association between the Preoperative Standard Uptake Value (SUV) and Survival Outcomes after Robotic-Assisted Segmentectomy for Resectable Non-Small Cell Lung Cancer (NSCLC)
Abstract
Background: Lung-sparing procedures, specifically segmentectomies and wedge resections, have increased over the years to treat early-stage non-small cell lung cancer (NSCLC). We investigate here the perioperative and long-term outcomes of patients who underwent robotic-assisted segmentectomy (RAS) at an NCI-designated cancer center and aim to show associations between the preoperative standard update value (SUV) to tumor stage, recurrence patterns, and overall survival.
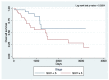
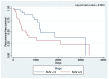
Methods: A retrospective analysis was performed on 166 consecutive patients who underwent RAS at a single institution from 2010 to 2021. Of this number, 121 robotic-assisted segmentectomies were performed for primary NSCLC, and a total of 101 patients were evaluated with a PET-CT scan. The SUV from the primary tumor was determined from the PET-CT. The clinical, surgical, and pathologic profiles and perioperative outcomes were summarized via descriptive statistics. Numerical variables were described as the median and interquartile range because all numerical variables were not normally distributed as assessed by the Shapiro-Wilk test of normality. Categorical variables were described as the count and proportion. Chi-square or Fisher's exact test was used for association. The main outcomes were overall survival (OS) and recurrence-free survival (RFS). Kaplan-Meier (KM) curves were constructed to visualize the OS and RFS, which were also stratified according to tumor histology, the pathologic stage, and standard uptake value. A log-rank test for the equality of survival curves was performed to determine significant differences between groups.
Results: The most common postoperative complications were atrial fibrillation (8.8%, 9/102), persistent air leak (7.84%, 8/102), and pneumonia (4.9%, 5/102). The median operative duration was 168.5 min (IQR 59), while the median estimated blood loss was 50 mL (IQR 125). The conversion rate to thoracotomy in this cohort was 3.9% (4/102). Intraoperative complications occurred in 2.9% (3/102). The median hospital length of stay was 3 days (IQR 3). The median chest tube duration was 3 days (IQR 2), but 4.9% (5/102) of patients were sent home with a chest tube. The recurrence for this cohort was 28.4% (29/102). The time to recurrence was 353 days (IQR 504), while the time to mortality was 505 days (IQR 761). The NSCLC patients were divided into the following two groups: low SUV (<5, n = 55) and high SUV (≥5, n = 47). Statistically significant associations were noted between SUV and the tumor histology (p = 0.019), tumor grade (p = 0.002), lymph-vascular invasion (p = 0.029), viscera-pleural invasion (p = 0.008), recurrence (p < 0.001) and the site of recurrence (p = 0.047). KM survival analysis showed significant differences in the curves for OS (log-rank p-value 0.0204) and RFS (log-rank p-value 0.0034) between the SUV groups.
Conclusion: Robotic-assisted segmentectomy for NSCLC has reasonable perioperative and oncologic outcomes. Furthermore, we demonstrate here the prognostic implication of preoperative SUV to pathologic outcomes, recurrence-free survival, and overall survival.
Keywords: lobectomy; non-small cell lung cancer (NSCLC); overall survival (OS); recurrence-free survival (RFS); segmentectomy; standard update value (SUV).
Conflict of interest statement
E.M.T. and J.P.F. have had financial relationships with Intuitive Surgical, Inc., in the form of an honoraria received as robotic thoracic surgery observation sites and proctors. None of the other authors have any conflict of interest to disclose.
Figures
Similar articles
-
Outcomes of robotic lobectomy for non-small cell lung cancer in a National Cancer Institute-Comprehensive Cancer Center vs. National Cancer Database.J Thorac Dis. 2023 Oct 31;15(10):5349-5361. doi: 10.21037/jtd-22-1340. Epub 2023 Sep 22. J Thorac Dis. 2023. PMID: 37969299 Free PMC article.
-
Oncologic outcomes of segmentectomy compared with lobectomy for clinical stage IA lung adenocarcinoma: propensity score-matched analysis in a multicenter study.J Thorac Cardiovasc Surg. 2013 Aug;146(2):358-64. doi: 10.1016/j.jtcvs.2013.02.008. Epub 2013 Mar 8. J Thorac Cardiovasc Surg. 2013. PMID: 23477694
-
Real-world survival outcomes of wedge resection versus lobectomy for cT1a/b cN0 cM0 non-small cell lung cancer: a single center retrospective analysis.Front Oncol. 2023 Aug 17;13:1226429. doi: 10.3389/fonc.2023.1226429. eCollection 2023. Front Oncol. 2023. PMID: 37664070 Free PMC article.
-
Clinical implication and prognostic significance of standardised uptake value of primary non-small cell lung cancer on positron emission tomography: analysis of 176 cases.Eur J Cardiothorac Surg. 2008 Oct;34(4):892-7. doi: 10.1016/j.ejcts.2008.07.023. Epub 2008 Aug 21. Eur J Cardiothorac Surg. 2008. PMID: 18722132 Review.
-
Robot-assisted thoracic surgery versus video-assisted thoracic surgery for lung lobectomy or segmentectomy in patients with non-small cell lung cancer: a meta-analysis.BMC Cancer. 2021 May 3;21(1):498. doi: 10.1186/s12885-021-08241-5. BMC Cancer. 2021. PMID: 33941112 Free PMC article.
References
-
- Brunelli A. Commentary: The ERS/ESTS clinical guidelines for evaluating fitness for radical treatment for lung cancer. Breathe. 2009;6:141–145. doi: 10.1183/18106838.0602.141. - DOI
LinkOut - more resources
Full Text Sources

